Resource library
Practical teaching assets for interventional pulmonology educators, learners, and clinician-builders.

Radiation Protection – Operator shielding

Atelectasis Severity (ASSESS Scoring Schematic)


CBCT – Brush Catheter Adjacent to Pleura (Axial)

CBCT – Brush Catheter Adjacent to Pleura (Sagittal)

CT – Features Predicting SSN Growth
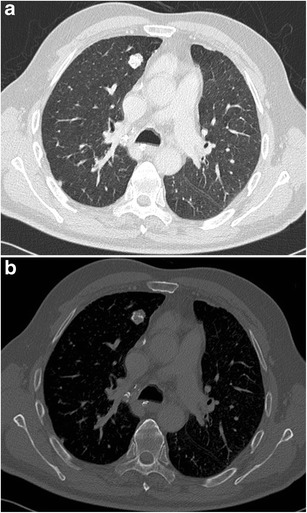
CT – Hamartoma with Popcorn Calcifications
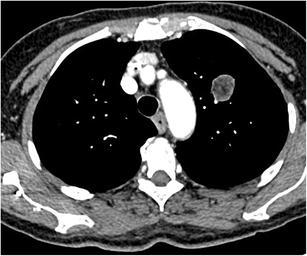
CT – Hamartoma with Popcorn Calcifications
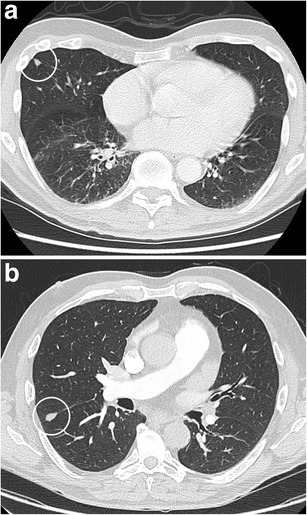
CT – Intrapulmonary Lymph Nodes (Triangular)
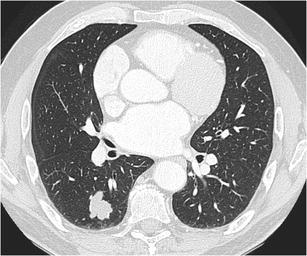
CT – Lobulated RLL Nodule (Adenocarcinoma)
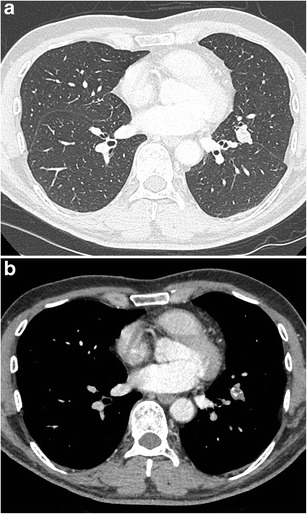
CT – LUL Lobulated Nodule (Hamartoma)

CT – LUL Mass (Contrast; Axial/Coronal/Sagittal)
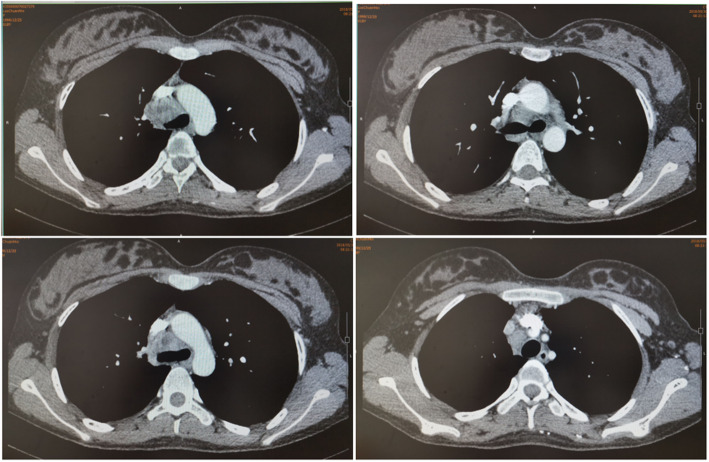
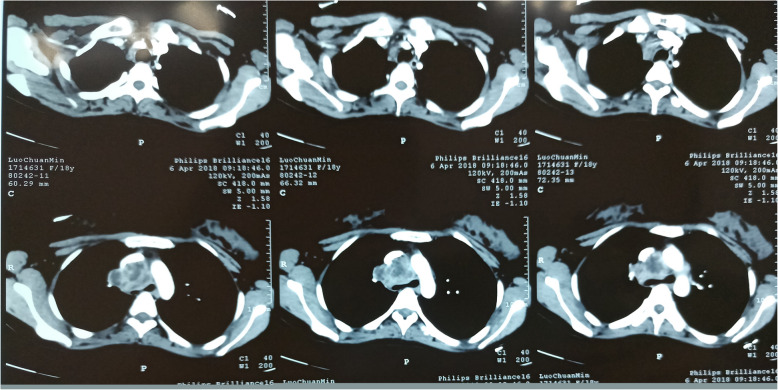
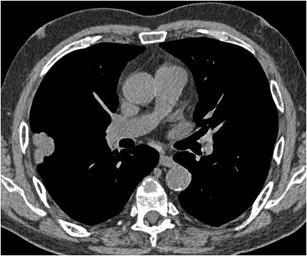
CT – Subpleural Lobulated Nodule (Adenocarcinoma)

CT – Suspicious Pulmonary Nodule (Right Lung)

CT – SVC/PA Encasement (Middle Mediastinal Mass)
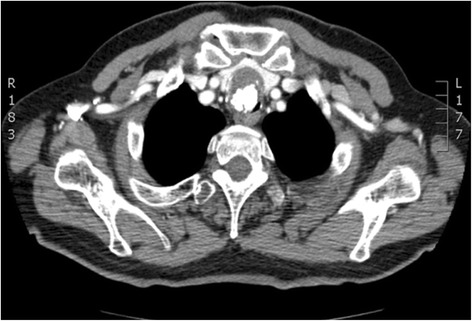
CT – Tracheal Lesion (At Presentation)


CXR/CT – Lobar Obstruction




PET/CT/Clinical – Mediastinal mass with tracheal compression (Ultraflex stent deployment, post-CTA)

PET-CT – Abnormal cartilage metabolism (thyroid, tracheal, rib cartilage)

CT – Airway stent migration to stomach

CT – Atelectasis/ventilation change pre/post stent

CT – Bilateral SEMS (pre/post comparison, coronal views with patent stents)

CT – Bilateral SEMS cases (multiplanar reconstruction, five patients)
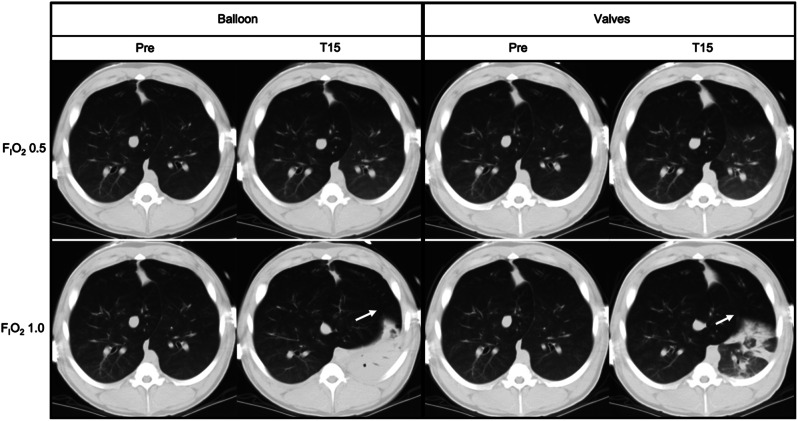
CT – BLVR occlusion methods (balloon vs valves, atelectasis patterns, accessory lobe expansion)

CT – Bronchus signs (truncation, passage, no bronchus)
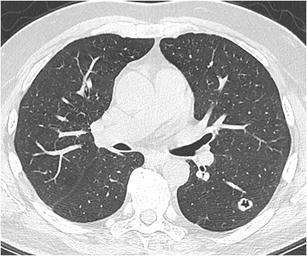
CT – Cavitary nodule (LLL squamous cell carcinoma)
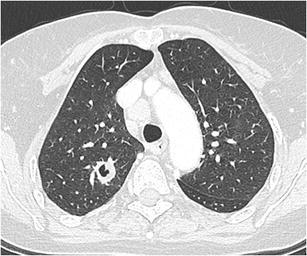
CT – Cavitary nodule (RUL aspergilloma)

CT – Central tumor progression (vascular and bronchial compression)
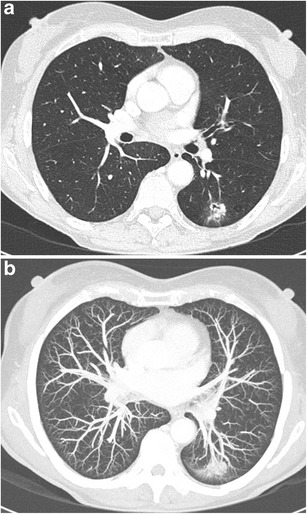
CT – Complex nodule with bronchial interruption sign (LLL invasive adenocarcinoma, MIP vessel convergence)
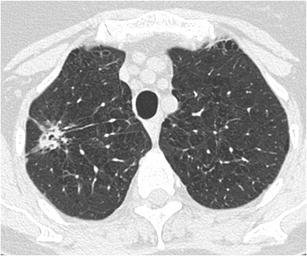
CT – Complex nodule with bubble-like lucencies (RUL adenocarcinoma, mixed growth patterns)
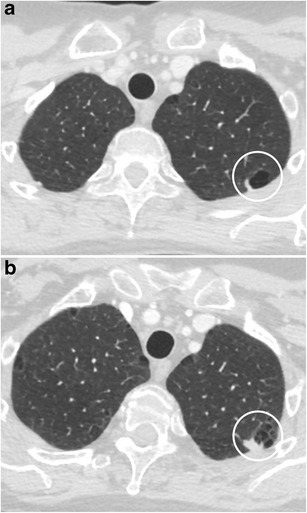
CT – Cystic airspace with mural nodule (LUL adenocarcinoma)

CT – Cystic lesion (right superior mediastinum, posterior SVC)
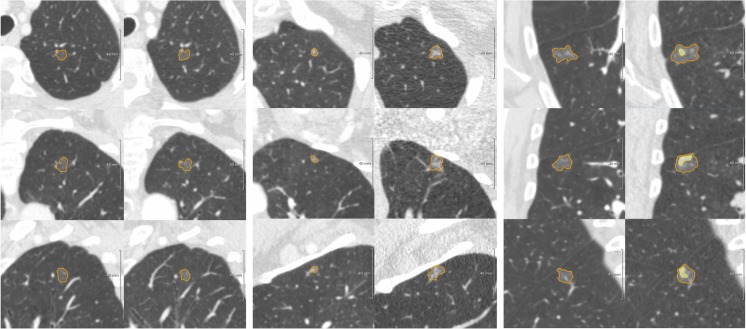
CT – Ground glass nodule evolution (stable, progressive, part-solid transformation)


CT – IASLC stations 4L/5/5
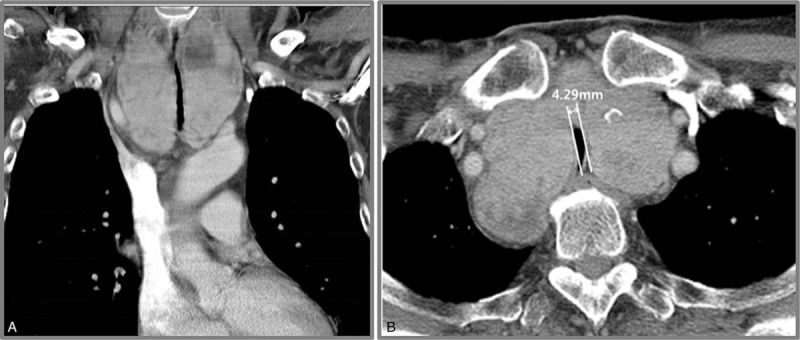
CT – Intrathoracic goiter (diffuse tracheal narrowing, severe obstruction)

CT – Large left-sided pleural effusion

CT – Large tracheal lesion (95% obstruction, inferior third)
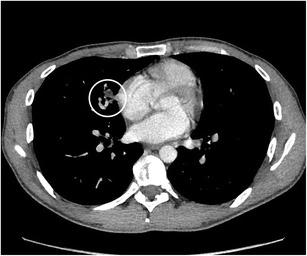
CT – Lipoid pneumonia (RML with fat component)
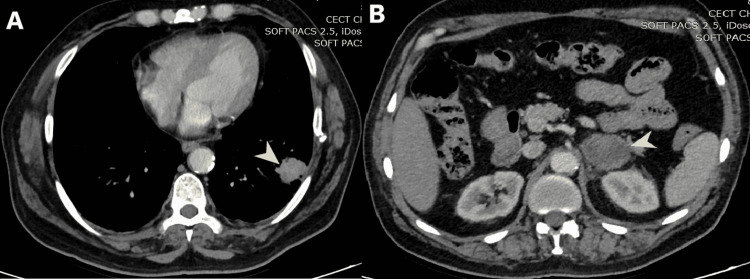
CT – LLL mass with left adrenal enlargement (heterogeneous enhancement)
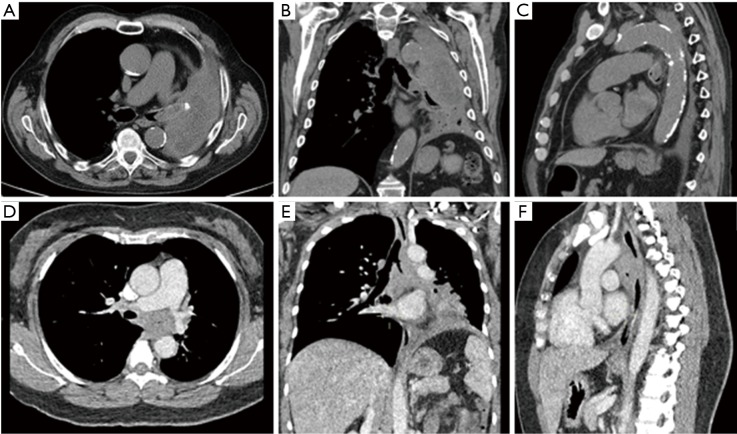

CT – Loculated empyema
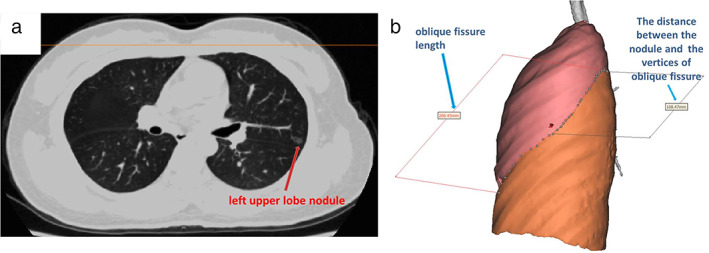
CT – LUL pulmonary nodule (oblique fissure measurement)
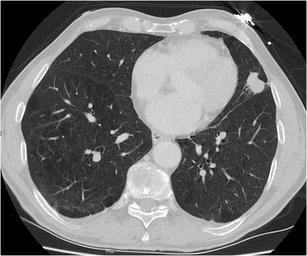
CT – Lung nodule with notch sign (lingula, large cell neuroendocrine carcinoma)
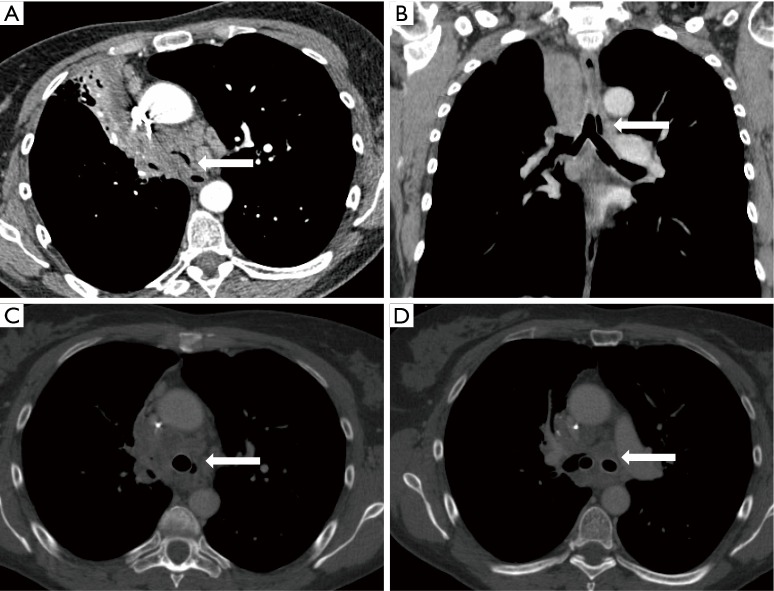
CT – Malignant CAO stenting (Dumon Y stent, post-laser and debulking, multiplanar views)
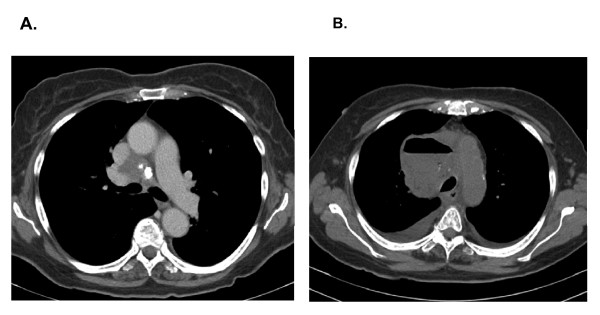
CT – Mediastinal abscess (post-EBUS TBNA complication)


CT – Mediastinal cyst wall enhancement (axial)

CT – Mediastinal mass (tracheal invasion, esophageal mass, chest wall and cervical involvement)
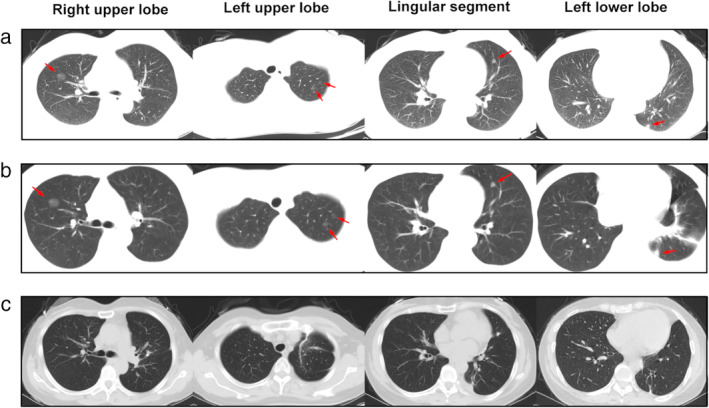
CT – Multiple ground glass nodules (post-trauma, follow-up, post-surgical changes)
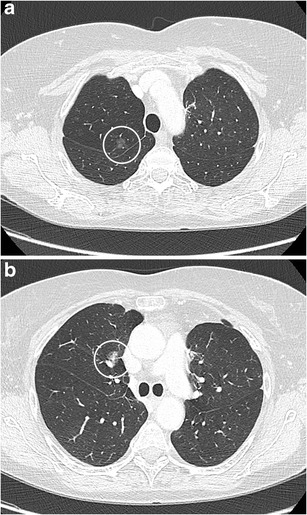
CT – Multiple subsolid nodules (pure GGN vs part-solid, adenocarcinoma in situ vs minimally invasive)

CT – Navigation planning (PlanPoint software, segmented views with target pathway)
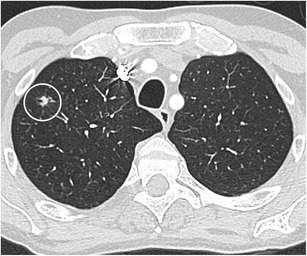
CT – Nodule with bronchial interruption sign (RLL NSCLC with adrenal metastasis)
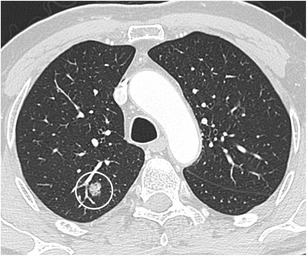
CT – Nodule with bubble-like lucencies (RUL adenocarcinoma with lepidic growth)
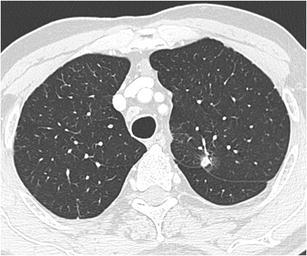
CT – Nodule with fissure retraction (adenocarcinoma)
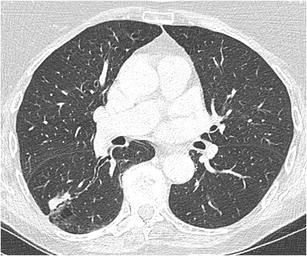
CT – Nodule with irregular air bronchogram (RLL adenocarcinoma)

CT – Pleural effusion (contiguous to primary lesion)

CT – Pneumomediastinum and Subcutaneous Empysema


CT – Post‑EBUS timeline: cyst enlargement

CT – Post‑EBUS timeline: cyst smaller post‑TBNA


CT – Post‑EBUS timeline: pleural effusion


CT – Post‑op neck soft tissue: diffuse tracheal calcification

CT – Post-operative bronchial kinking (lower lobar bronchus)

CT – Post-SBRT (11-month follow-up, ground-glass appearance)

CT – Post-SBRT (2-month and 8-month follow-up)

CT – Post-stent removal (tracheal patency)


CT – Preoperative planning (RFID tag placement for S8a GGN, 3D reconstruction)

CT – RFA treatment (3D thermodynamic reconstruction maps, pre/post comparison)

CT – RFID tag deviation (target vs actual placement site, 20.8mm distance)

CT – RLL mass with pleural effusion (compressive atelectasis, mass-like opacity)
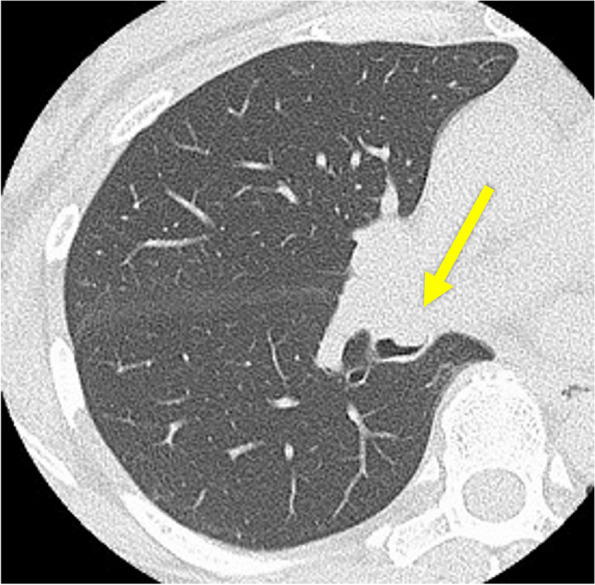
CT – RML orifice tumor with atelectasis
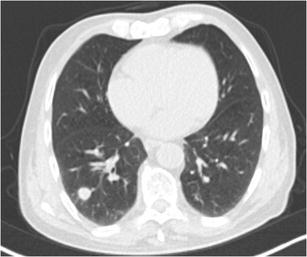
CT – Round well-delineated solid nodule (RLL squamous cell carcinoma)

CT – RUL nodule with mediastinal adenopathy

CT – Septated pleural effusion & “bubble sign”
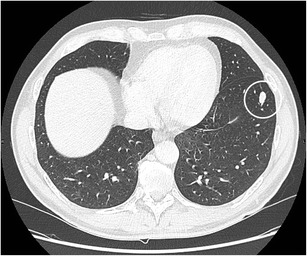
CT – Sharply delineated oval nodule (LLL typical carcinoid)
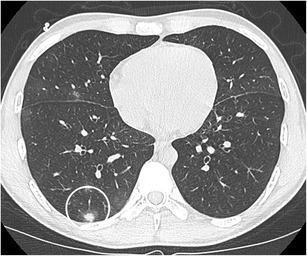
CT – Solid nodule with ground glass halo (RLL invasive aspergillosis)

CT – Solitary lung nodule (2D and 3D MSCT with distance measurement)
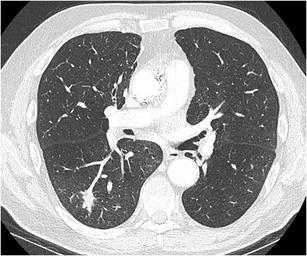
CT – Spiculated nodule (RLL squamous cell carcinoma)
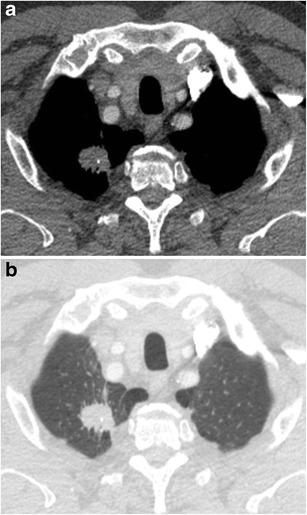
CT – Spiculated nodule with calcifications (RUL apex, squamous cell carcinoma)
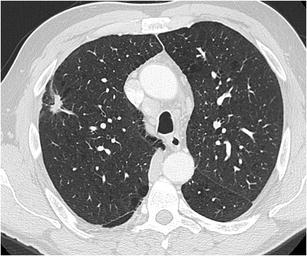
CT – Spiculated nodule with notch sign (RUL small cell lung cancer with lymphadenopathy)
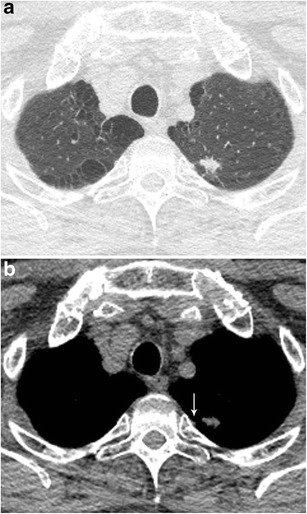
CT – Spiculated nodule with pleural tags (LUL adenocarcinoma with pleural invasion)

CT – Spiculated subpleural nodule (RUL apex with paraseptal emphysema)

CT – Squamous cell lung cancer (extrinsic obstruction, alveolus stent placement)

CT – Station 4R adenopathy

CT – Subpleural reticulation & cysts (MIP selection)
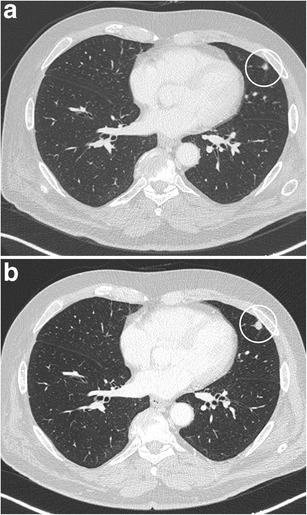
CT – Subpleural solid nodule (intrapulmonary lymph node, lingula)

CT – SVC and right pulmonary artery compression (mediastinal mass)

CT – Temporal evolution of LMB obstruction & stenting

CT – Thyroid mass with tracheal deviation

CT – Tracheal and bilateral main bronchi stenosis (soft tissue thickening)

CT – Tracheal and bronchial wall thickening (left lung atelectasis and bronchiectasis)

CT – Tracheal patency (post-stent and chemotherapy, 5-year follow-up)

CT – Tracheal schwannoma causing obstruction

CT – Tracheal stenosis
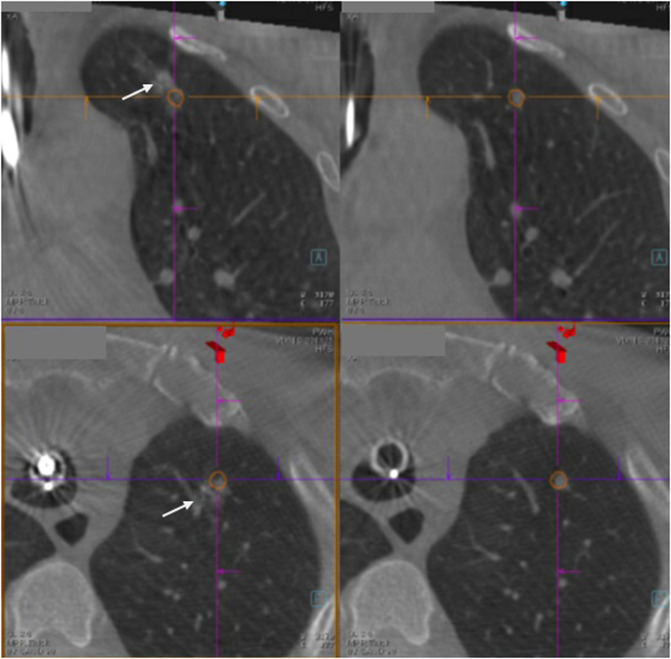
CT – Triple dye injection (iodinated contrast, ICG, methylene blue near lung lesion)

CT – Tumor response after chemoradiation (tracheobronchial)
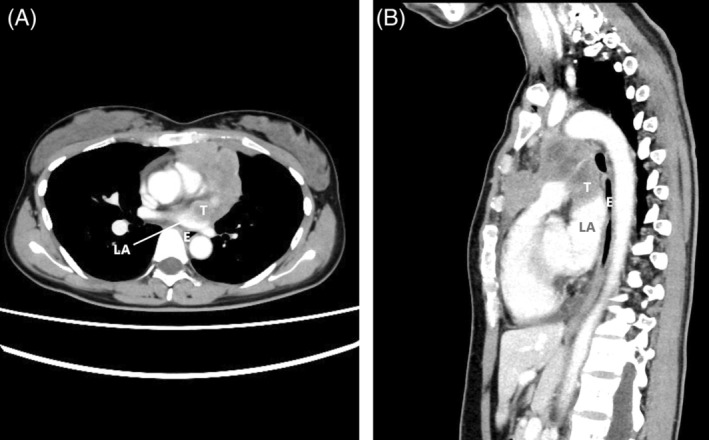
CT – Tumor with cardiac invasion (left atrial involvement)

CT – Upper tracheal stenosis (axial and coronal views)

CT Angio – Azygos vein ectasia

Chest X-ray – Postoperative Lobectom

Chest X-ray – Coil placement (post-interventional)

Chest X-ray – Edema/effusions resolving after diuresis
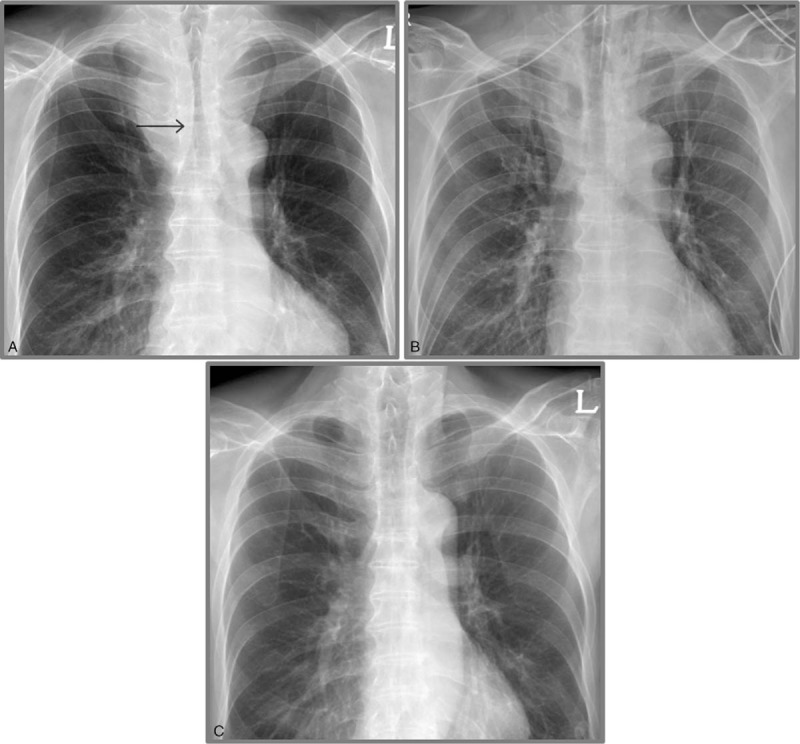
Chest X-ray – Intrathoracic goiter management (ECMO support, ETT positioning, post-extubation)
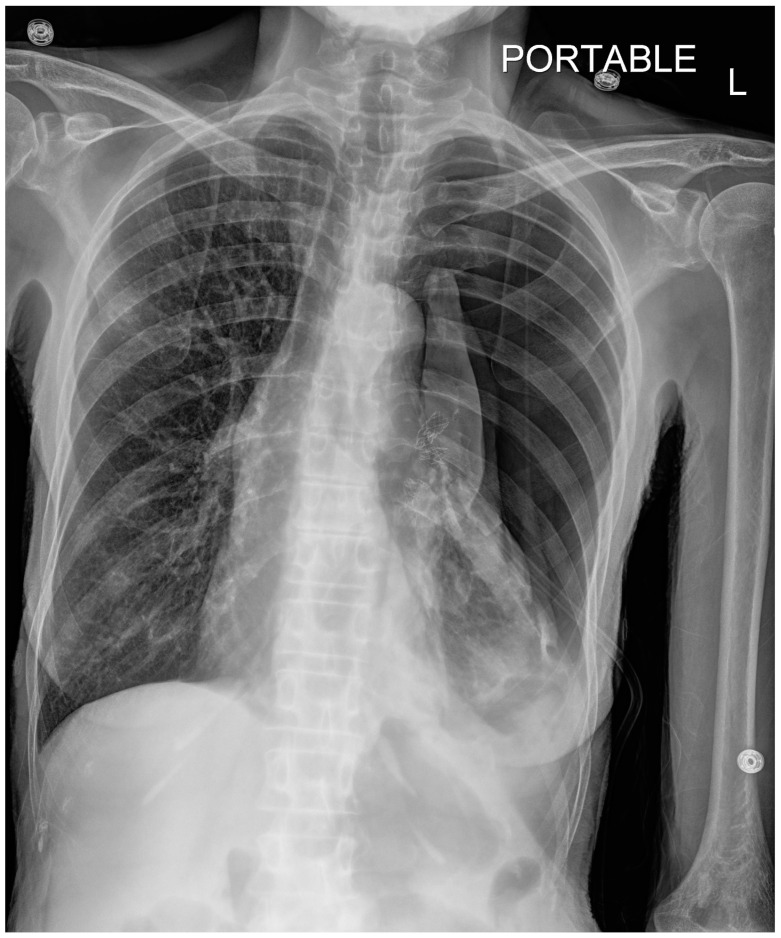
Chest X-ray – Large left pneumothorax (post-bronchial valve, mediastinal shift)
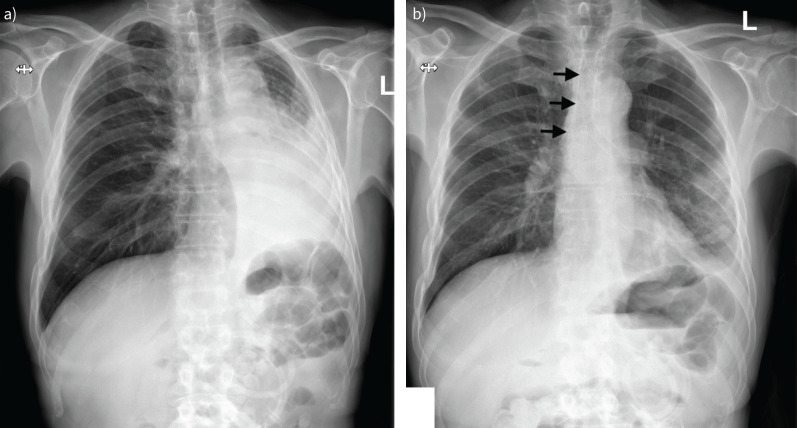
Chest X-ray – Left lung atelectasis (pre/post stent for LMB stenosis)

Chest X-ray – Post-chest tube placement (residual loculated pneumothorax)

Chest X-ray – Postoperative Lobectomy with atelectasis of residual parenchyma

Chest X-ray – Post-valve LUL volume loss (hemothorax, endobronchial valves)

Chest X-ray – Pre-procedure COPD (bronchial valve candidate)

Chest X-ray – RLL mass (initial and follow-up with pleural effusion)

Chest X-ray – Stent placement (LLL re-expansion)

Chest X-ray – Thoracoscopy pre/post comparison (loculated empyema resolution)

Chest X-ray – Tracheal deviation & mediastinal shift

Chest X-ray – Tracheal shadow (bilateral pulmonary infiltrates)

Chest X-ray /CT – RMS endobronchial tumor

Chest X-ray/CT – LMB total occlusion (hilar mass with post-obstructive pneumonia)

Chest X-ray/CT Timeline – Pneumothorax management (drainage, stent placement, resolution)

Chest X-ray/CT – Left spontaneous pneumothorax (chest tube, air-fluid level, specimen)

Ultrasound – A lines (reverberation artifacts of pleuropulmonary interface)

Ultrasound – B lines (comet-tail artifacts, interlobular septa)

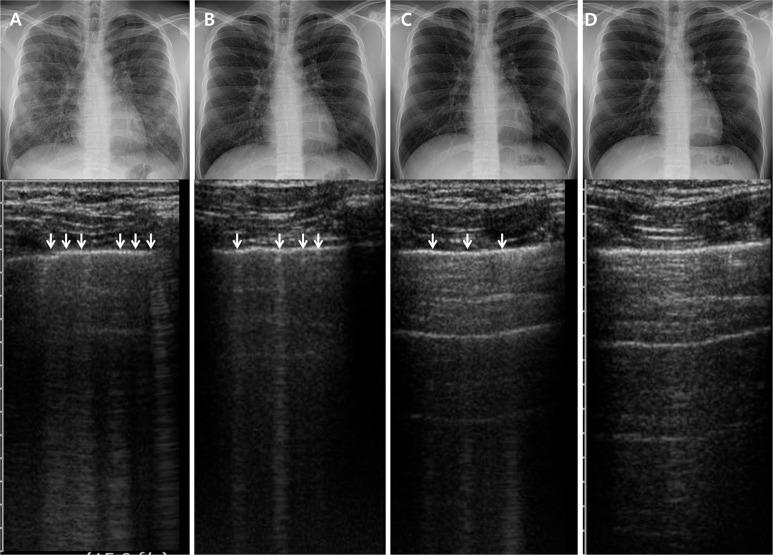
Ultrasound – B-lines timeline (days 1, 4, 7, 14)





Ultrasound – Floating visceral pleura (atelectasis)

Ultrasound – Complex nonseptated pleural effusion (heterogeneous hyperechoic spots)

Ultrasound – Malignant pleural effusion (fibrinous septation)
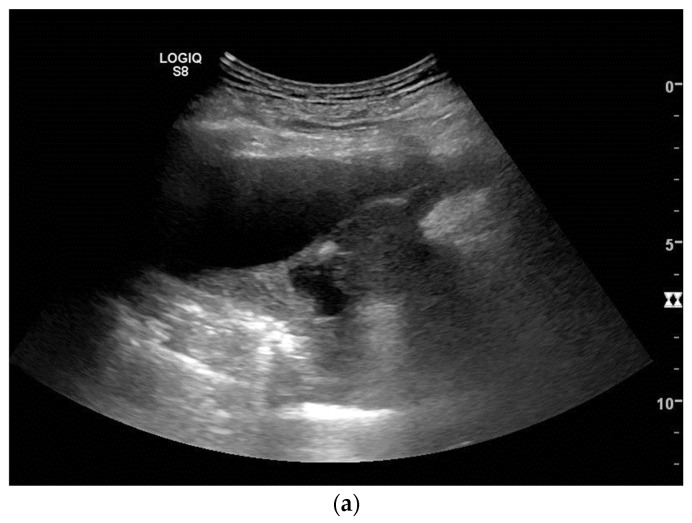
Ultrasound – Mesothelioma (pleural effusion, tumor masses, diaphragm infiltration, rib fracture)
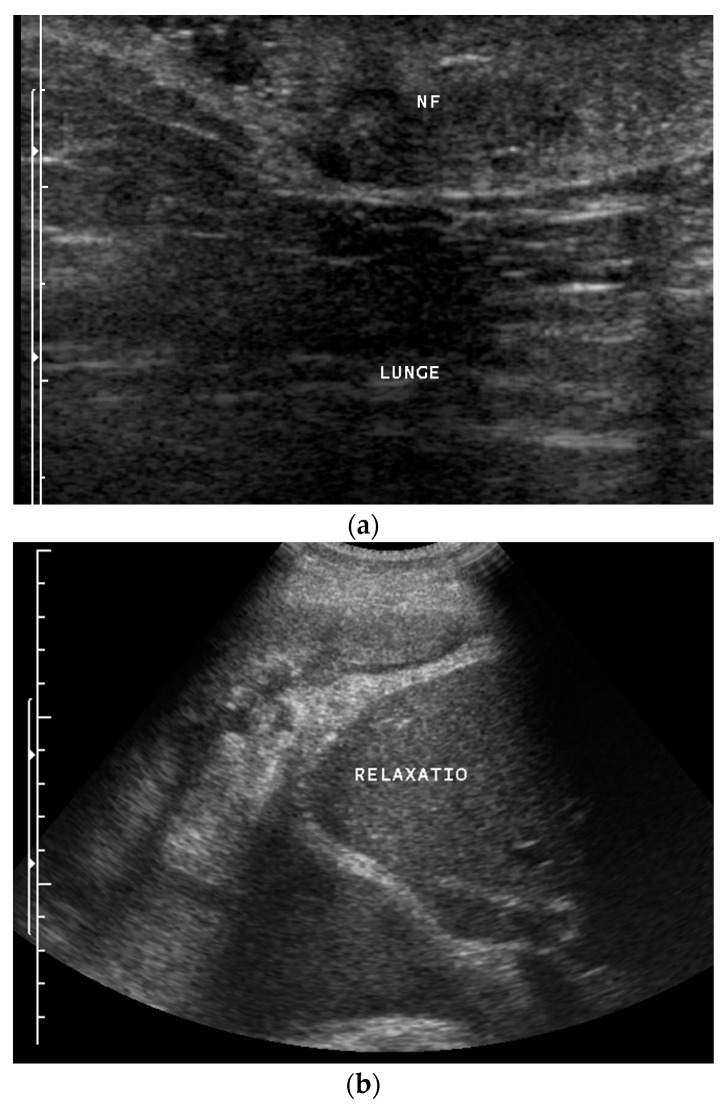
Ultrasound – Neurofibrosarcoma and neurofibroma (diaphragm paralysis, liver bulging)

Ultrasound – Pleural adhesions (diaphragmatic to collapsed lung)

Ultrasound – Pleural thickening (bat sign, oblique approach for rib shadow avoidance)

Ultrasound – Pleural thickening technique (transverse/longitudinal probe positioning)

Ultrasound – Pneumothorax (absent lung sliding at pleural line)

Ultrasound – Sonographic anatomy (chest wall layers, pleural line, probe comparison)

Spirometry/CT – Pre/post treatment comparison (tracheal tumor, flow-volume curves)

Post‑transplant – Stent for anastomotic dehiscence
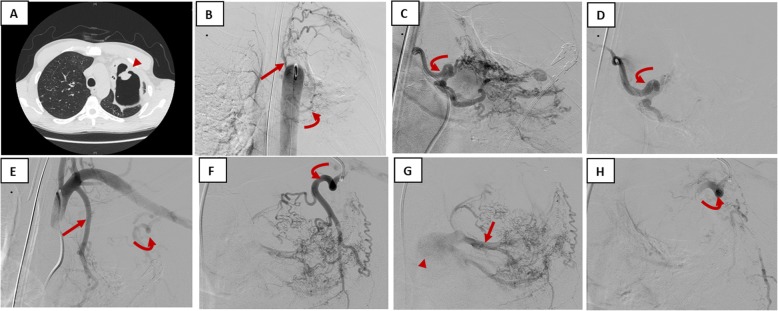
IR – Bronchial artery embolization for hemoptysis

Localization – CBCT‑assisted ENB marking


Localization – Lipiodol (CT‑guided)

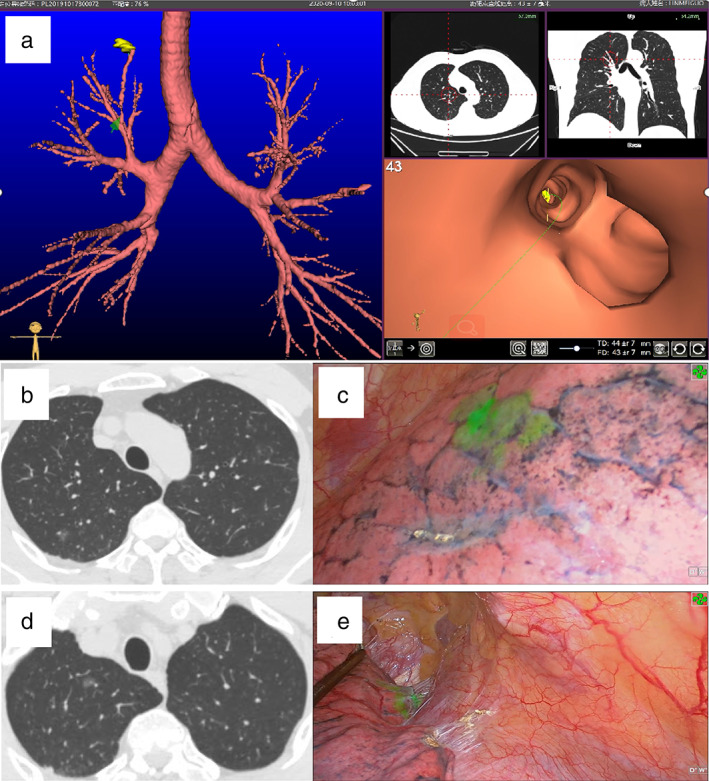
Localization – VNB‑guided ICG fluorescence

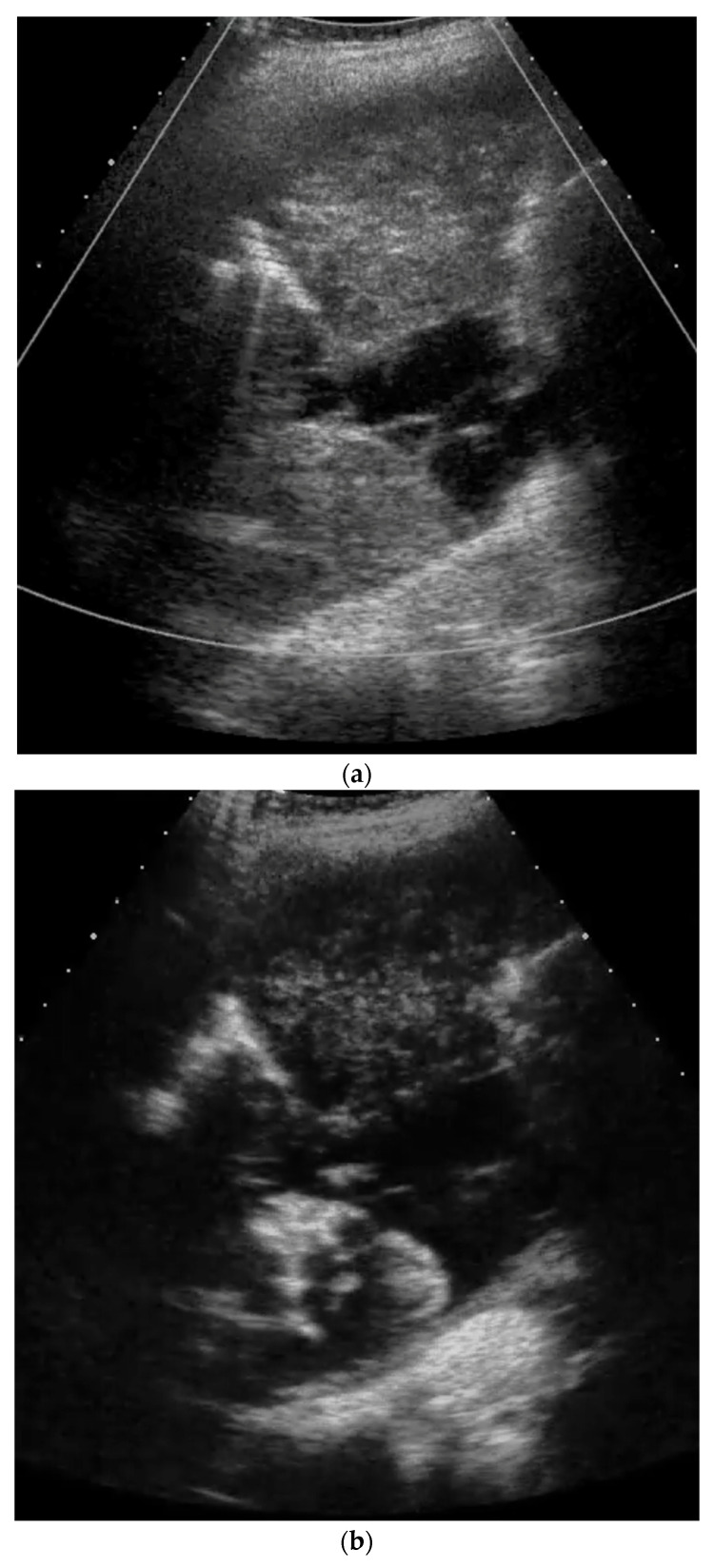
Ultrasound/CEUS – Primary lung sarcoma (pleural metastasis, enhancement patterns)

Ultrasound/CT Correlation – Pleural thickening (hypoecogenic lobular mass with circumferential pattern)

Ultrasound/CT Correlation – Pleural thickening localization (solid/cystic/complex characteristics)
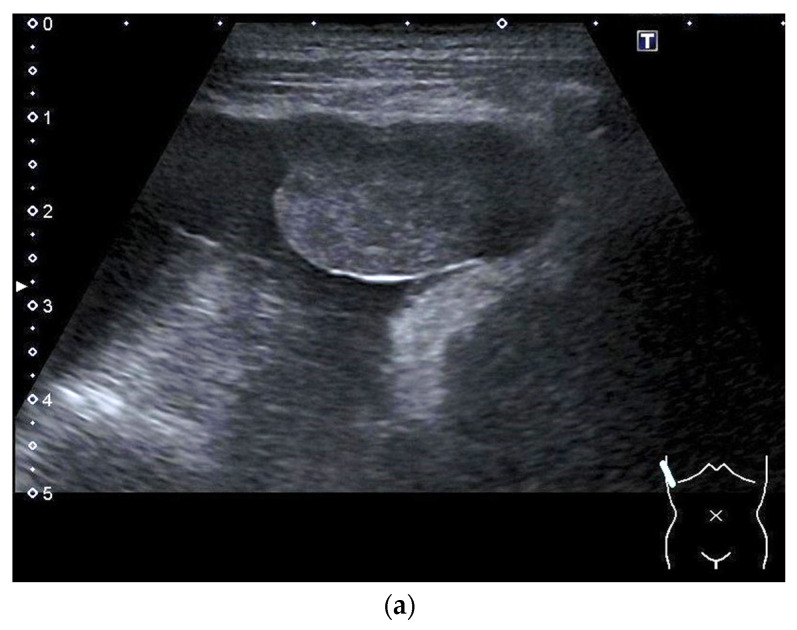
Ultrasound/Pathology – Epithelioid mesothelioma (pleural effusion, solid tumor with biopsy)

CT/Chest X-ray – RMB and carina obstruction (Y-stent placement)

CT/Chest X-ray Correlation – Intratracheal tumor

CT/Fluoroscopy – Y‑stent implantation
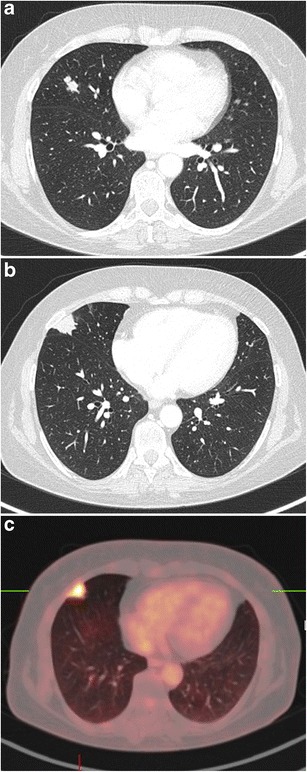
CT – Multiple nodules (carcinoid vs tuberculoma in oncology patient)
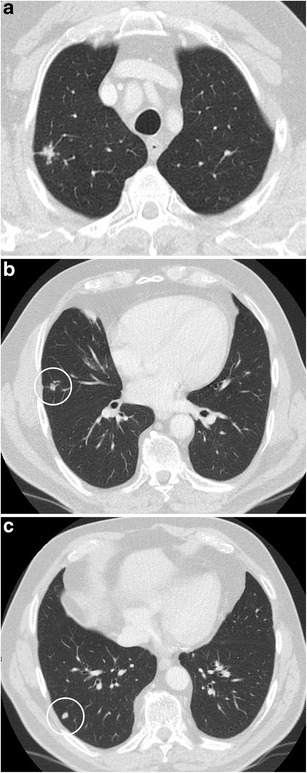
CT – Multiple pulmonary nodules (spiculated morphology, varied PET uptake)

CT/PET-CT – Chest imaging (multiplanar correlation)
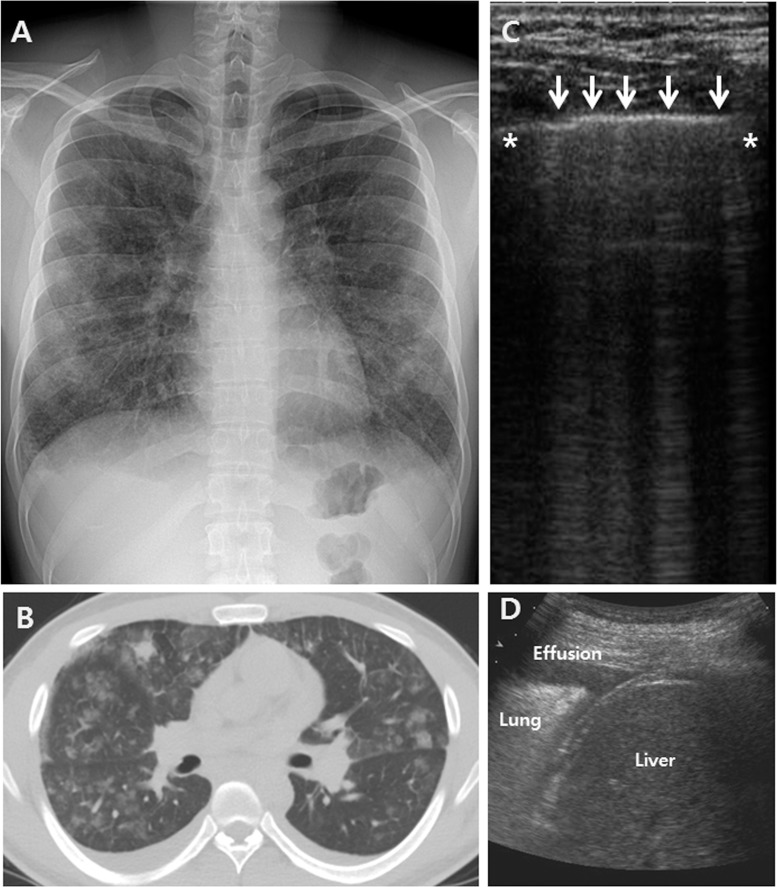
Chest X-ray/CT/Ultrasound – Bilateral GGO (interlobular septal thickening, B-lines, pleural effusion)

Chest X-ray/CT/Ultrasound – Mediastinal Hodgkin lymphoma (prevascular mass, airway compression, pleural effusion)
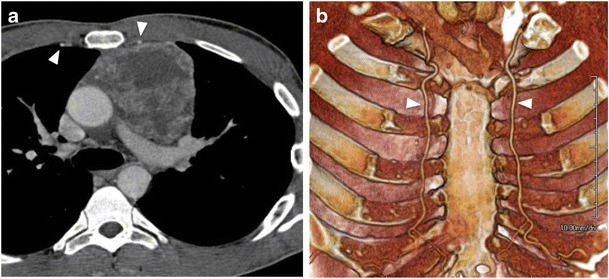
Anatomy – Internal mammary arteries on CT/3D
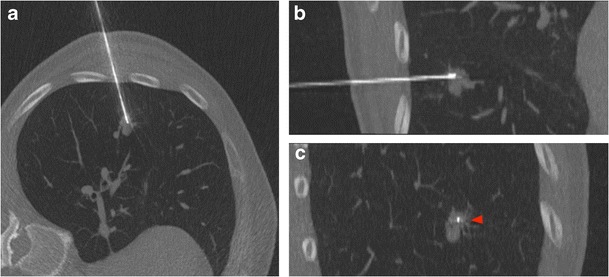
Biopsy – CT‑guided lung nodule (multi‑plane)

Biopsy – CT‑guided: hemorrhage complication
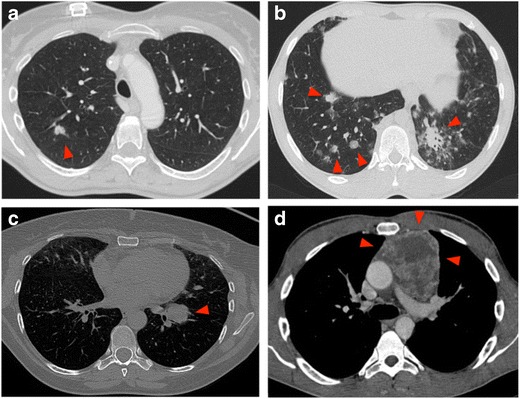
Biopsy – CT‑guided: indications
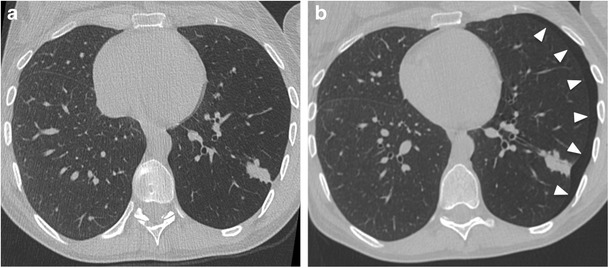
Biopsy – CT‑guided: pneumothorax complication
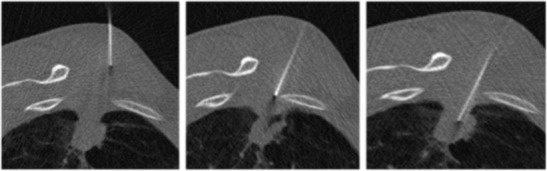
Biopsy – Fluoroscopy‑guided lung nodule
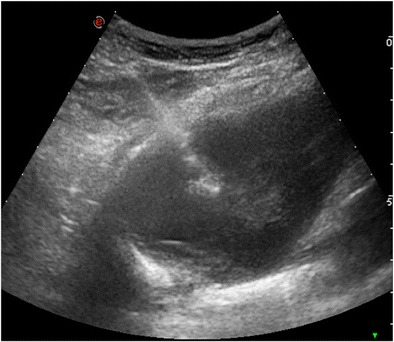
Biopsy – Ultrasound‑guided lung nodule