Resource library
Practical teaching assets for interventional pulmonology educators, learners, and clinician-builders.
Found 680 images
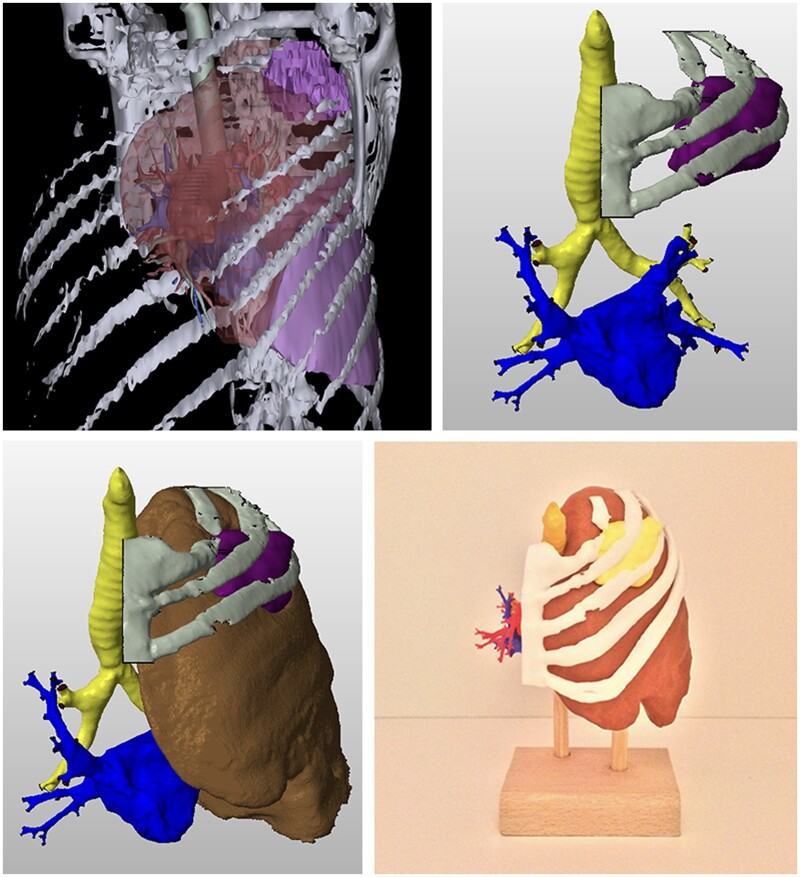
3D Printing – LUL tumor reconstruction (STL file processing)
3D Reconstruction – Bronchial tree timeline (LMB stenosis and stent placement)
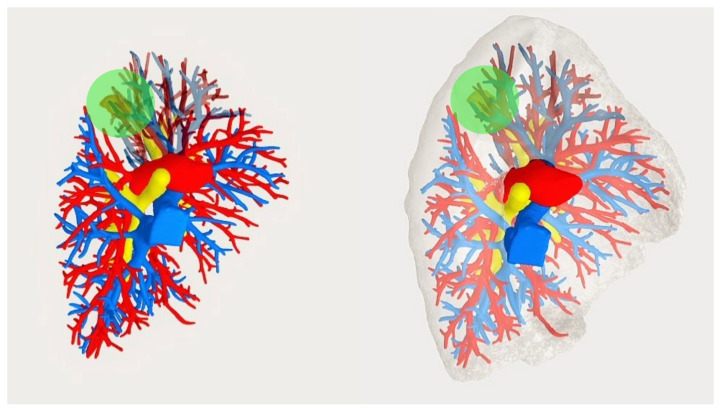
3D Reconstruction – Broncho-vascular anatomy (LUL S1+2 with nodule)
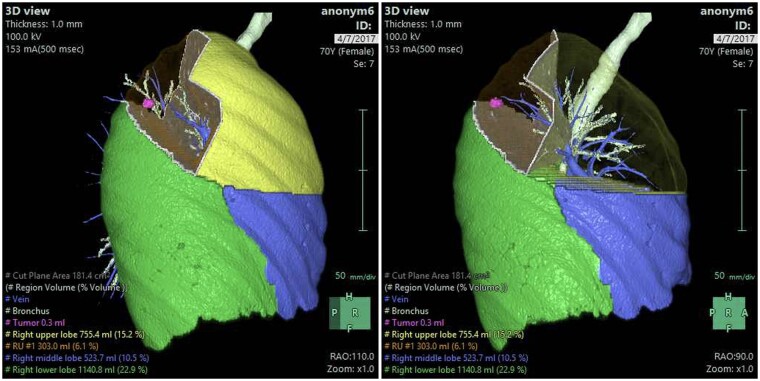
3D Reconstruction – Lung parenchyma segmentectomy simulation (S7+8 with nodule)
3D Reconstruction – Venous drainage (LUL surgical dissection vs virtual)
3D Reconstruction – Virtual bronchoscopy (CT-based bronchial model)
3D Reconstruction – Virtual segmentectomy
Augmented Reality – Virtual 3D model overlay (bronchoscope location display)
Radiation Protection – Operator shielding
Atelectasis Severity (ASSESS Scoring Schematic)
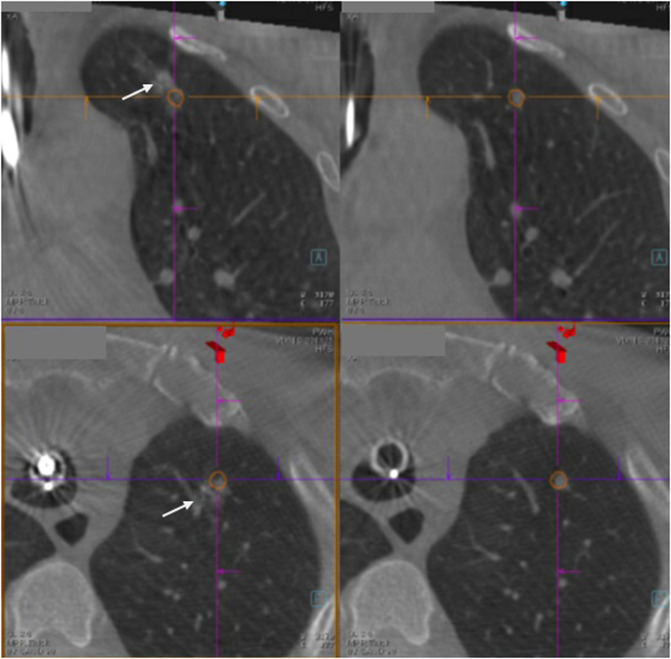
CBCT – Brush Catheter Adjacent to Pleura (Axial)
CBCT – Brush Catheter Adjacent to Pleura (Sagittal)
CT – Features Predicting SSN Growth
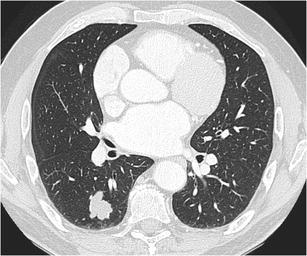
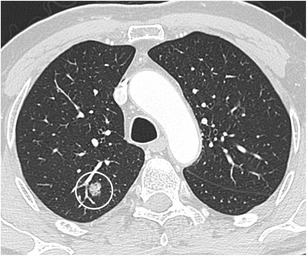
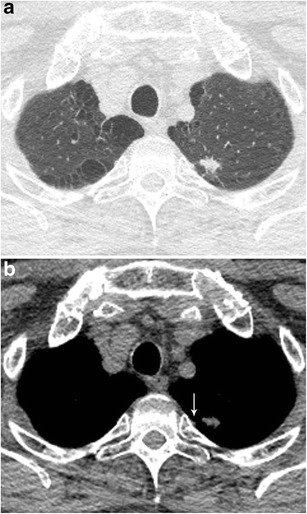
CT – Hamartoma with Popcorn Calcifications
CT – Hamartoma with Popcorn Calcifications
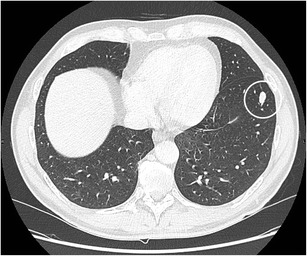
CT – Intrapulmonary Lymph Nodes (Triangular)
CT – Lobulated RLL Nodule (Adenocarcinoma)
CT – LUL Lobulated Nodule (Hamartoma)
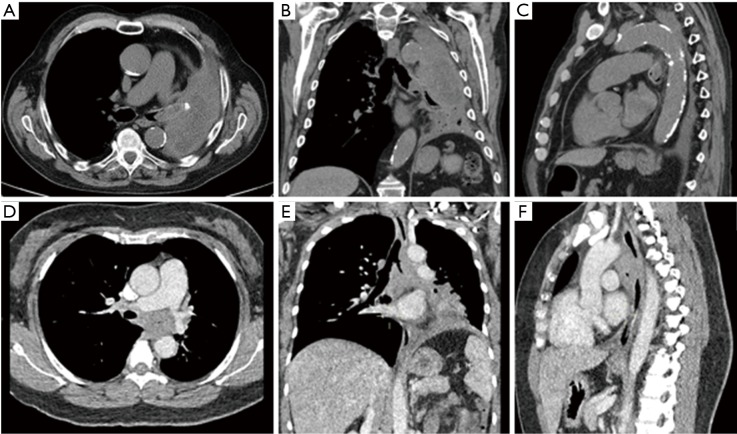
CT – LUL Mass (Contrast; Axial/Coronal/Sagittal)
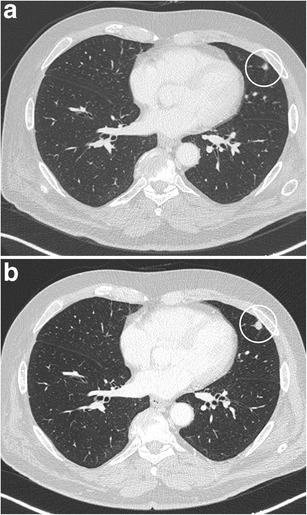
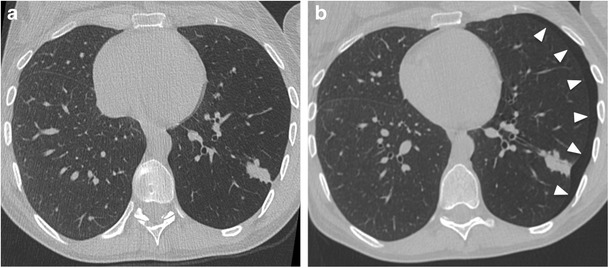
CT – Subpleural Lobulated Nodule (Adenocarcinoma)
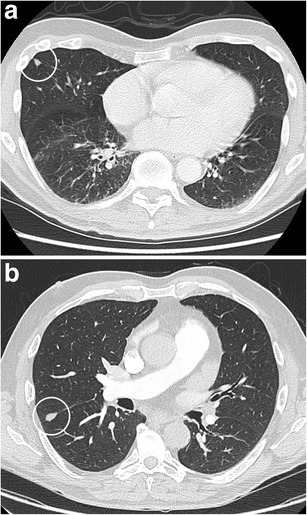
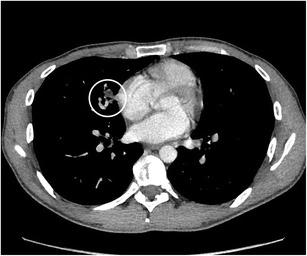
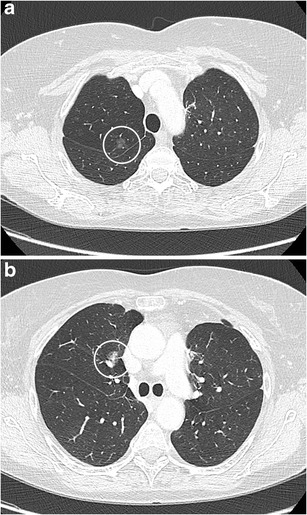
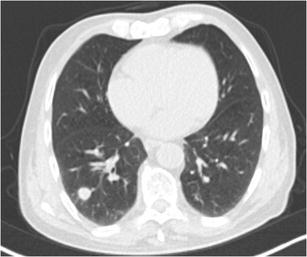
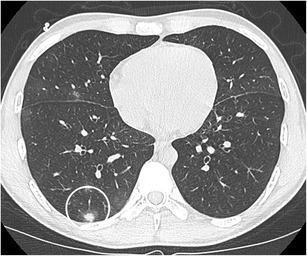
CT – Suspicious Pulmonary Nodule (Right Lung)
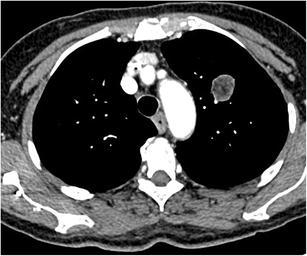
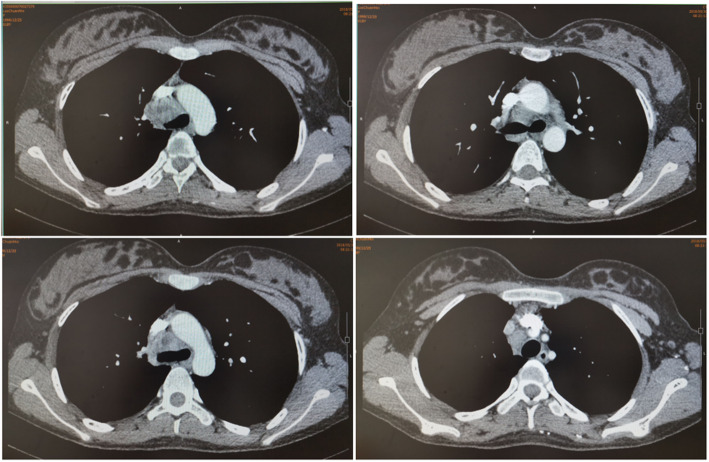
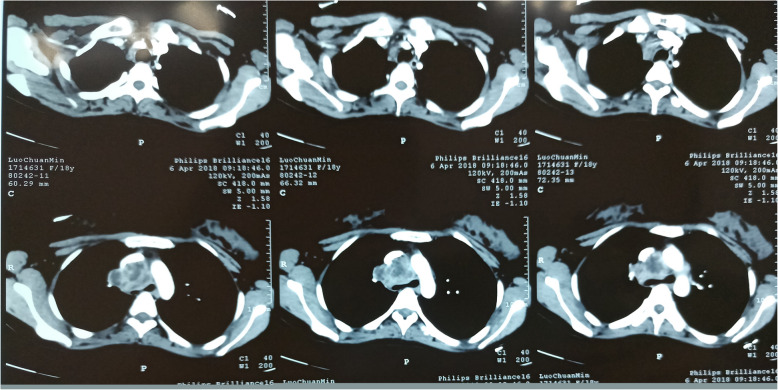
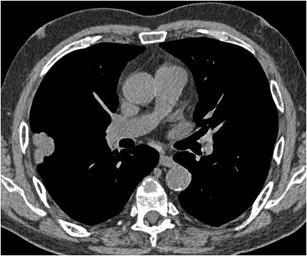
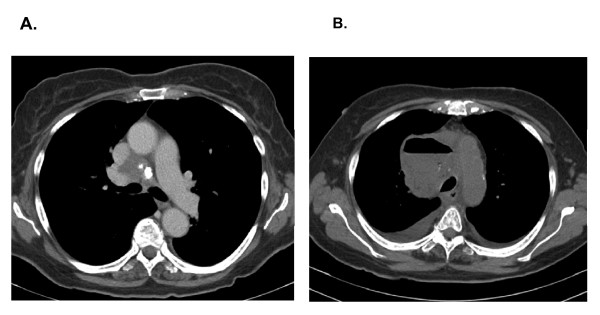
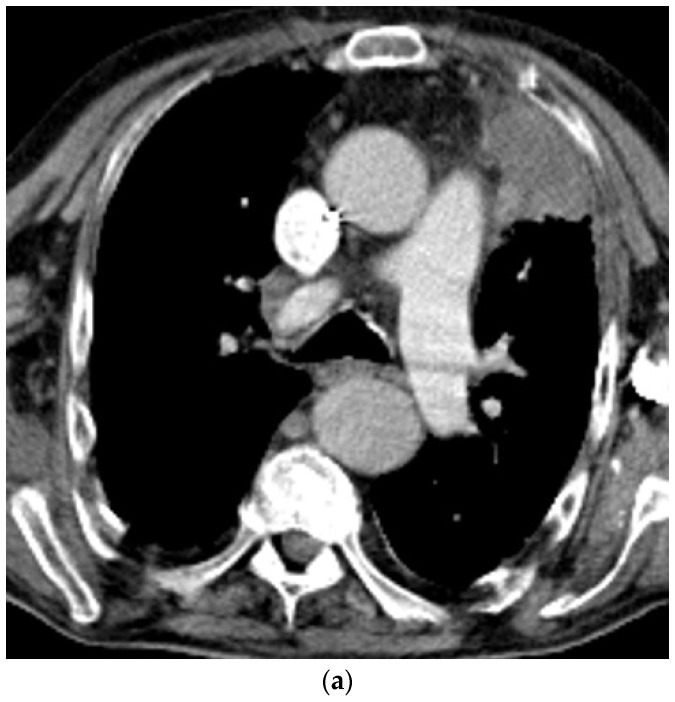
CT – SVC/PA Encasement (Middle Mediastinal Mass)
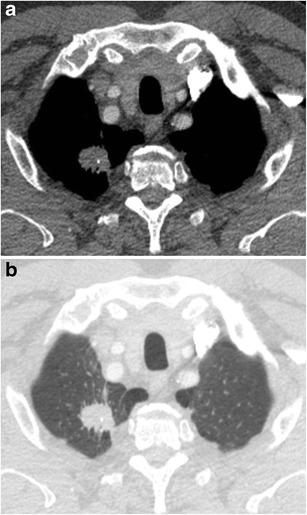
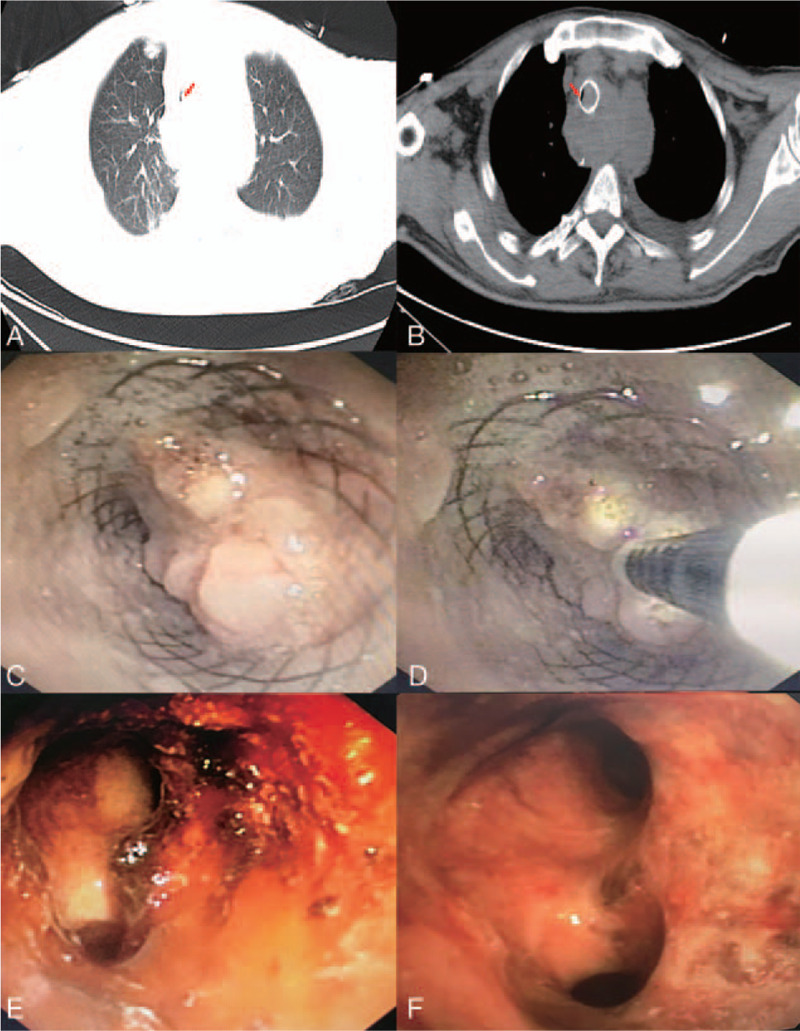
CT – Tracheal Lesion (At Presentation)
CXR/CT – Lobar Obstruction
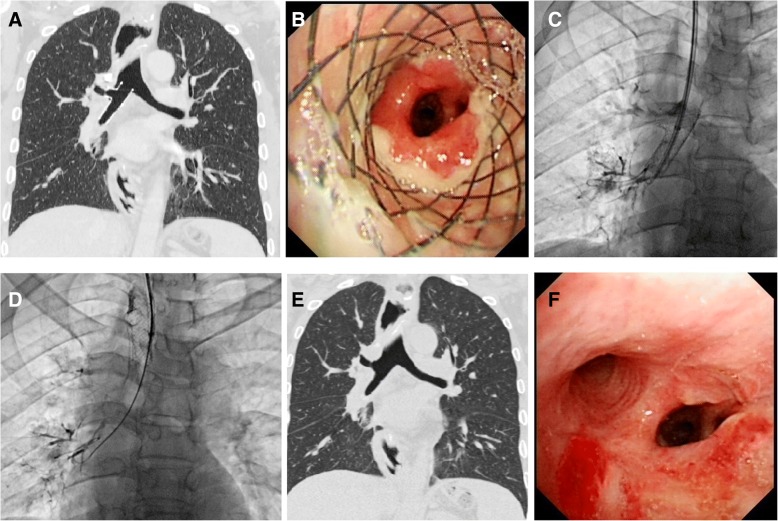
PET/CT/Clinical – Mediastinal mass with tracheal compression (Ultraflex stent deployment, post-CTA)
PET-CT – Abnormal cartilage metabolism (thyroid, tracheal, rib cartilage)
CT – Airway stent migration to stomach
CT – Atelectasis/ventilation change pre/post stent
CT – Bilateral SEMS (pre/post comparison, coronal views with patent stents)
CT – Bilateral SEMS cases (multiplanar reconstruction, five patients)
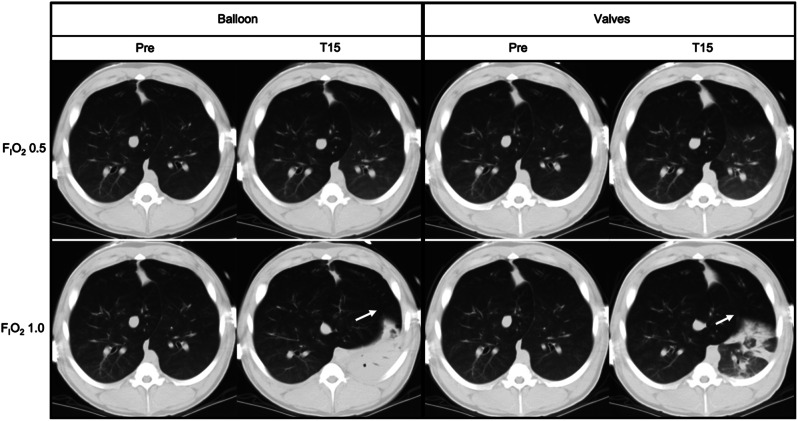
CT – BLVR occlusion methods (balloon vs valves, atelectasis patterns, accessory lobe expansion)
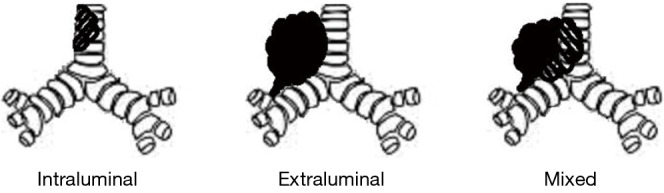
CT – Bronchus signs (truncation, passage, no bronchus)
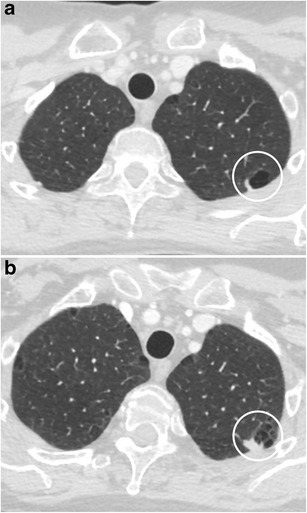
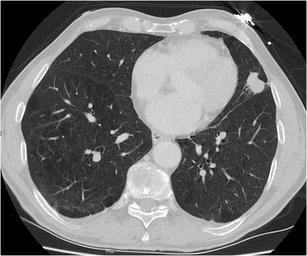
CT – Cavitary nodule (LLL squamous cell carcinoma)
CT – Cavitary nodule (RUL aspergilloma)
CT – Central tumor progression (vascular and bronchial compression)
CT – Complex nodule with bronchial interruption sign (LLL invasive adenocarcinoma, MIP vessel convergence)
CT – Complex nodule with bubble-like lucencies (RUL adenocarcinoma, mixed growth patterns)
CT – Cystic airspace with mural nodule (LUL adenocarcinoma)
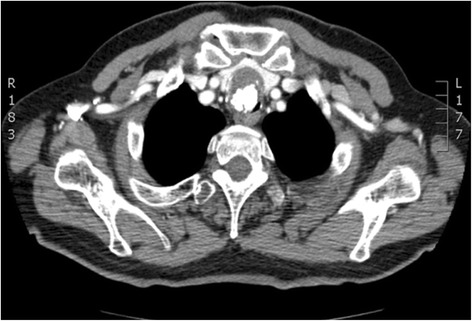
CT – Cystic lesion (right superior mediastinum, posterior SVC)
CT – Ground glass nodule evolution (stable, progressive, part-solid transformation)
CT – IASLC stations 4L/5/5
CT – Intrathoracic goiter (diffuse tracheal narrowing, severe obstruction)
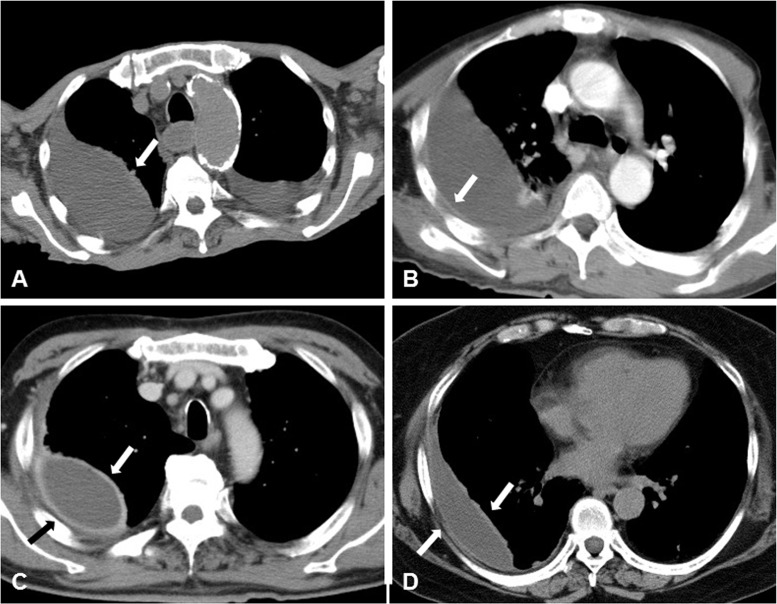
CT – Large left-sided pleural effusion
CT – Large tracheal lesion (95% obstruction, inferior third)
CT – Lipoid pneumonia (RML with fat component)
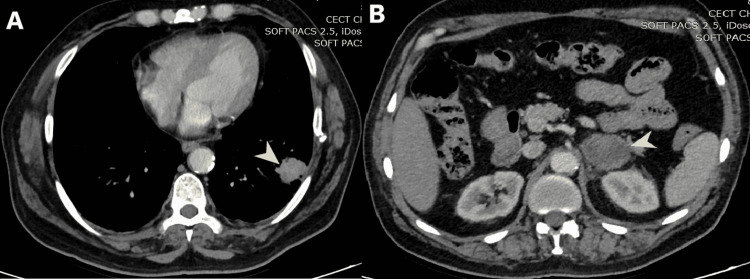
CT – LLL mass with left adrenal enlargement (heterogeneous enhancement)
CT – Loculated empyema
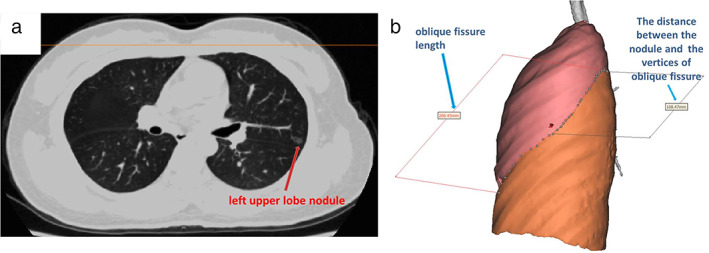
CT – LUL pulmonary nodule (oblique fissure measurement)
CT – Lung nodule with notch sign (lingula, large cell neuroendocrine carcinoma)
CT – Malignant CAO stenting (Dumon Y stent, post-laser and debulking, multiplanar views)
CT – Mediastinal abscess (post-EBUS TBNA complication)
CT – Mediastinal cyst wall enhancement (axial)
CT – Mediastinal mass (tracheal invasion, esophageal mass, chest wall and cervical involvement)
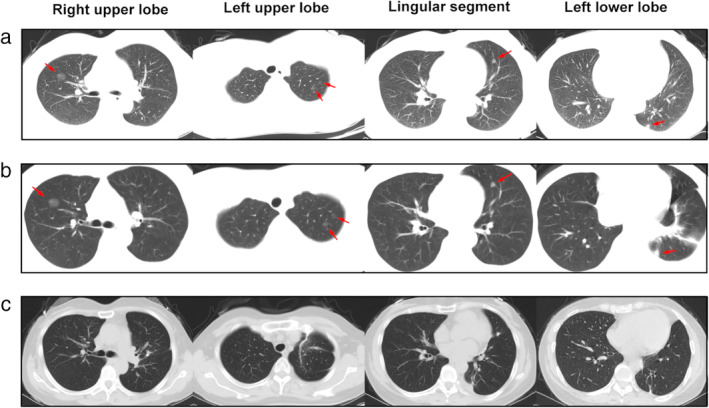
CT – Multiple ground glass nodules (post-trauma, follow-up, post-surgical changes)
CT – Multiple subsolid nodules (pure GGN vs part-solid, adenocarcinoma in situ vs minimally invasive)
CT – Navigation planning (PlanPoint software, segmented views with target pathway)
CT – Nodule with bronchial interruption sign (RLL NSCLC with adrenal metastasis)
CT – Nodule with bubble-like lucencies (RUL adenocarcinoma with lepidic growth)
CT – Nodule with fissure retraction (adenocarcinoma)
CT – Nodule with irregular air bronchogram (RLL adenocarcinoma)
CT – Pleural effusion (contiguous to primary lesion)
CT – Pneumomediastinum and Subcutaneous Empysema
CT – Post‑EBUS timeline: cyst enlargement
CT – Post‑EBUS timeline: cyst smaller post‑TBNA
CT – Post‑EBUS timeline: pleural effusion
CT – Post‑op neck soft tissue: diffuse tracheal calcification
CT – Post-operative bronchial kinking (lower lobar bronchus)
CT – Post-SBRT (11-month follow-up, ground-glass appearance)
CT – Post-SBRT (2-month and 8-month follow-up)
CT – Post-stent removal (tracheal patency)
CT – Preoperative planning (RFID tag placement for S8a GGN, 3D reconstruction)
CT – RFA treatment (3D thermodynamic reconstruction maps, pre/post comparison)
CT – RFID tag deviation (target vs actual placement site, 20.8mm distance)
CT – RLL mass with pleural effusion (compressive atelectasis, mass-like opacity)
CT – RML orifice tumor with atelectasis
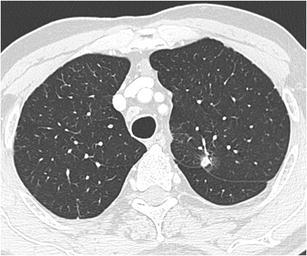
CT – Round well-delineated solid nodule (RLL squamous cell carcinoma)
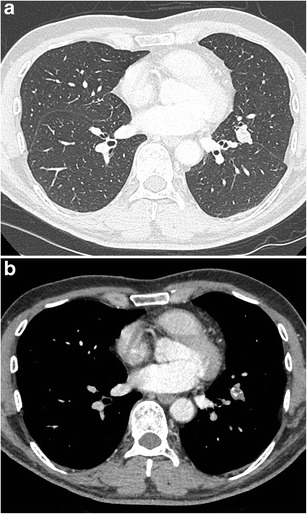
CT – RUL nodule with mediastinal adenopathy
CT – Septated pleural effusion & “bubble sign”
CT – Sharply delineated oval nodule (LLL typical carcinoid)
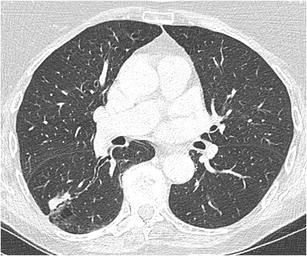
CT – Solid nodule with ground glass halo (RLL invasive aspergillosis)
CT – Solitary lung nodule (2D and 3D MSCT with distance measurement)
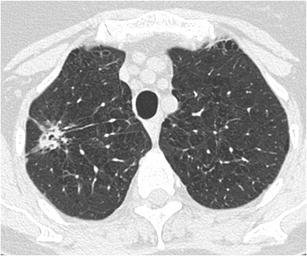
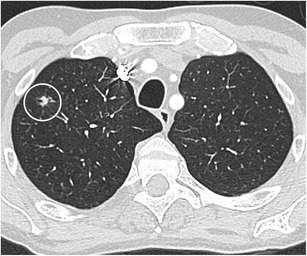
CT – Spiculated nodule (RLL squamous cell carcinoma)
CT – Spiculated nodule with calcifications (RUL apex, squamous cell carcinoma)
CT – Spiculated nodule with notch sign (RUL small cell lung cancer with lymphadenopathy)
CT – Spiculated nodule with pleural tags (LUL adenocarcinoma with pleural invasion)
CT – Spiculated subpleural nodule (RUL apex with paraseptal emphysema)
CT – Squamous cell lung cancer (extrinsic obstruction, alveolus stent placement)
CT – Station 4R adenopathy
CT – Subpleural reticulation & cysts (MIP selection)
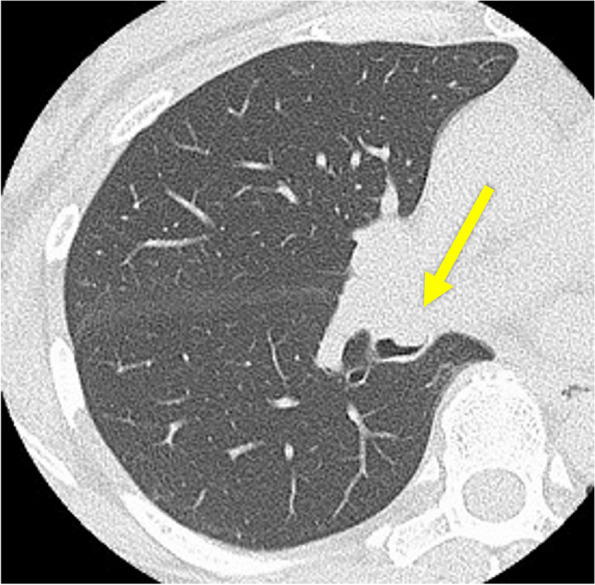
CT – Subpleural solid nodule (intrapulmonary lymph node, lingula)
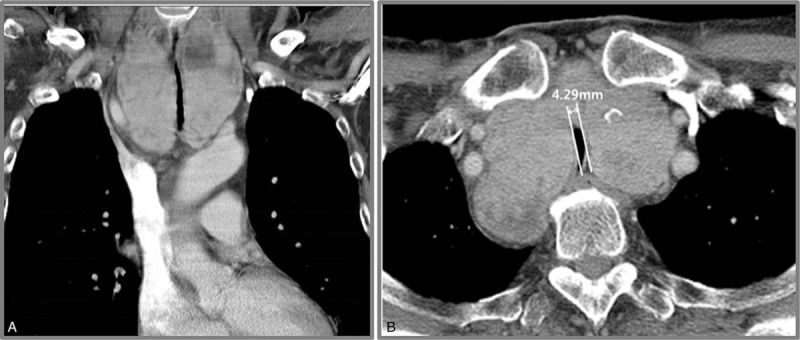
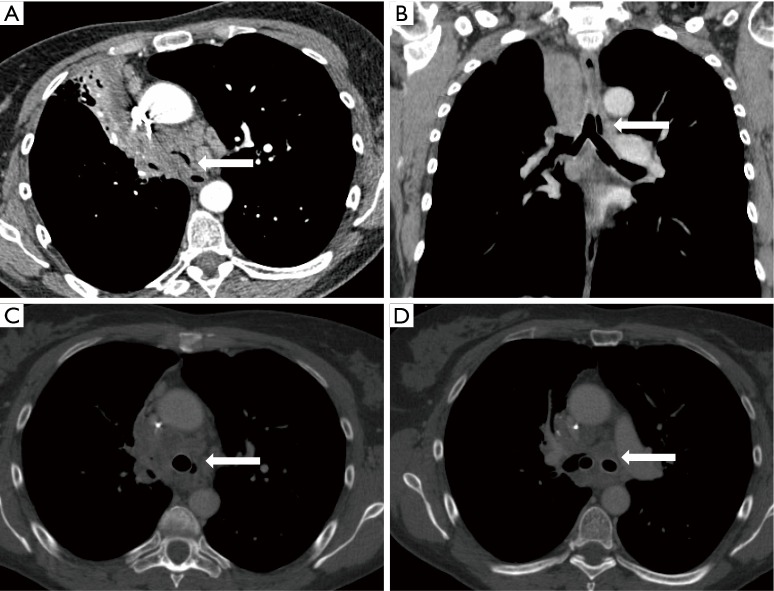
CT – SVC and right pulmonary artery compression (mediastinal mass)
CT – Temporal evolution of LMB obstruction & stenting
CT – Thyroid mass with tracheal deviation
CT – Tracheal and bilateral main bronchi stenosis (soft tissue thickening)
CT – Tracheal and bronchial wall thickening (left lung atelectasis and bronchiectasis)
CT – Tracheal patency (post-stent and chemotherapy, 5-year follow-up)
CT – Tracheal schwannoma causing obstruction
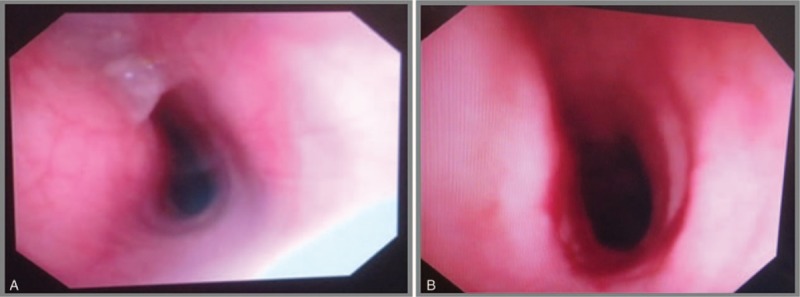
CT – Tracheal stenosis
CT – Triple dye injection (iodinated contrast, ICG, methylene blue near lung lesion)
CT – Tumor response after chemoradiation (tracheobronchial)
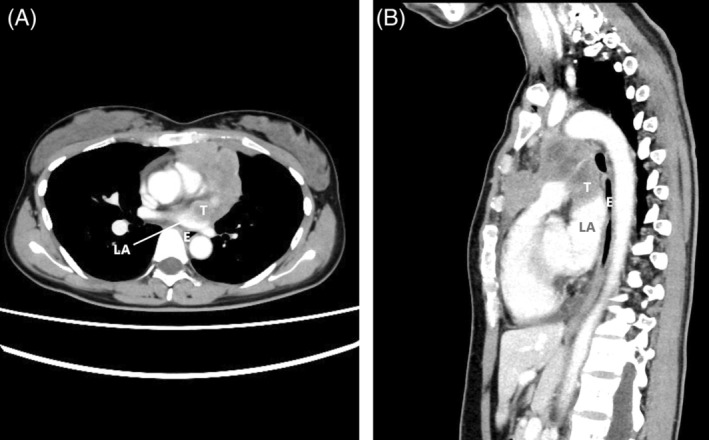
CT – Tumor with cardiac invasion (left atrial involvement)
CT – Upper tracheal stenosis (axial and coronal views)
CT Angio – Azygos vein ectasia
Chest X-ray – Postoperative Lobectom
Chest X-ray – Coil placement (post-interventional)
Chest X-ray – Edema/effusions resolving after diuresis
Chest X-ray – Intrathoracic goiter management (ECMO support, ETT positioning, post-extubation)
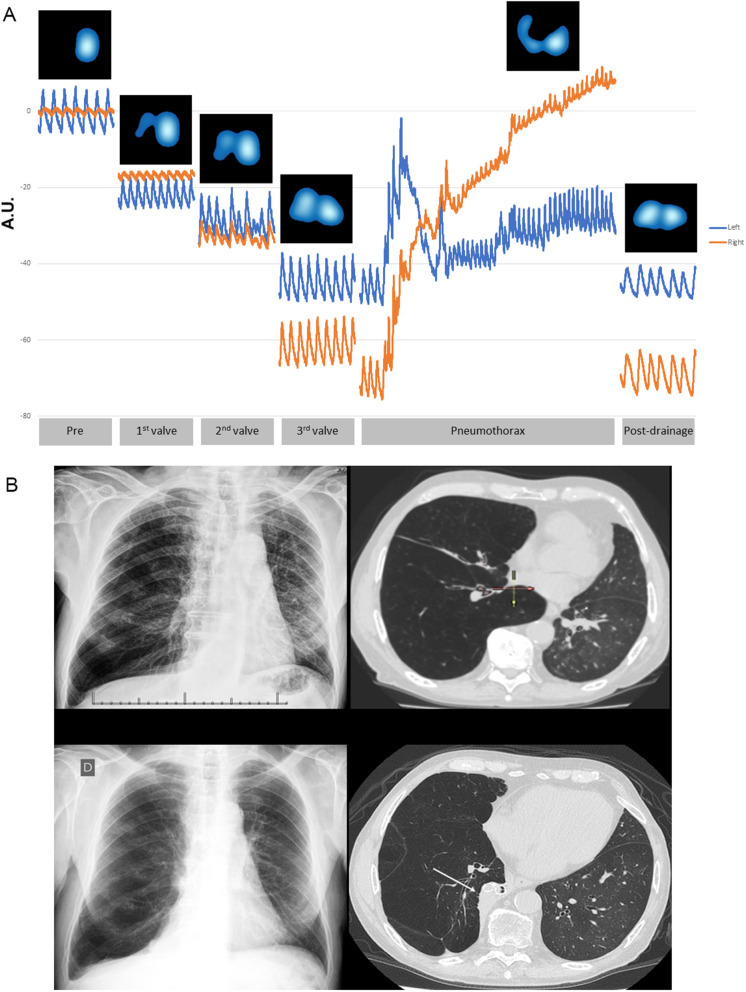
Chest X-ray – Large left pneumothorax (post-bronchial valve, mediastinal shift)
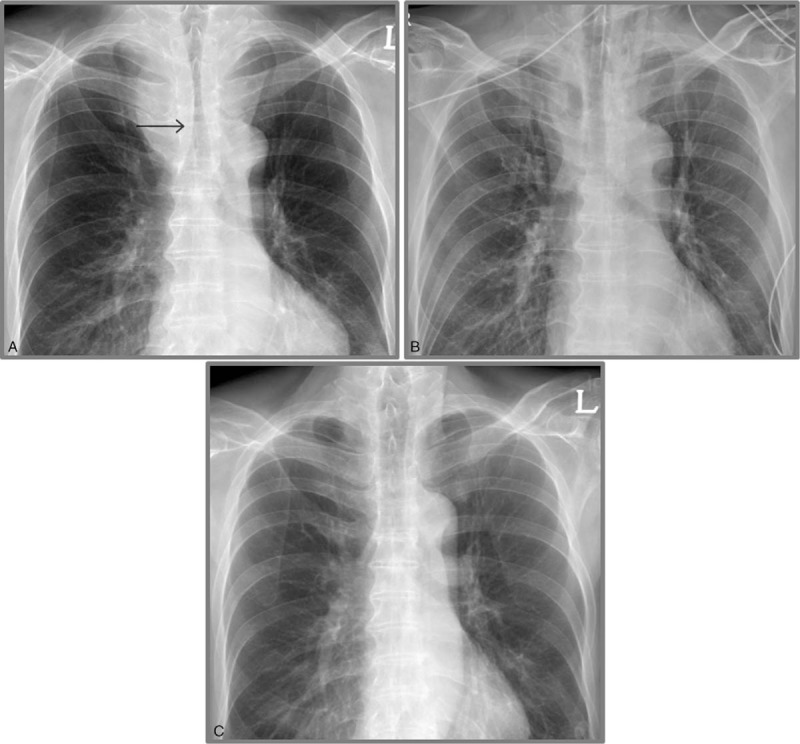
Chest X-ray – Left lung atelectasis (pre/post stent for LMB stenosis)
Chest X-ray – Post-chest tube placement (residual loculated pneumothorax)
Chest X-ray – Postoperative Lobectomy with atelectasis of residual parenchyma
Chest X-ray – Post-valve LUL volume loss (hemothorax, endobronchial valves)
Chest X-ray – Pre-procedure COPD (bronchial valve candidate)
Chest X-ray – RLL mass (initial and follow-up with pleural effusion)
Chest X-ray – Stent placement (LLL re-expansion)
Chest X-ray – Thoracoscopy pre/post comparison (loculated empyema resolution)
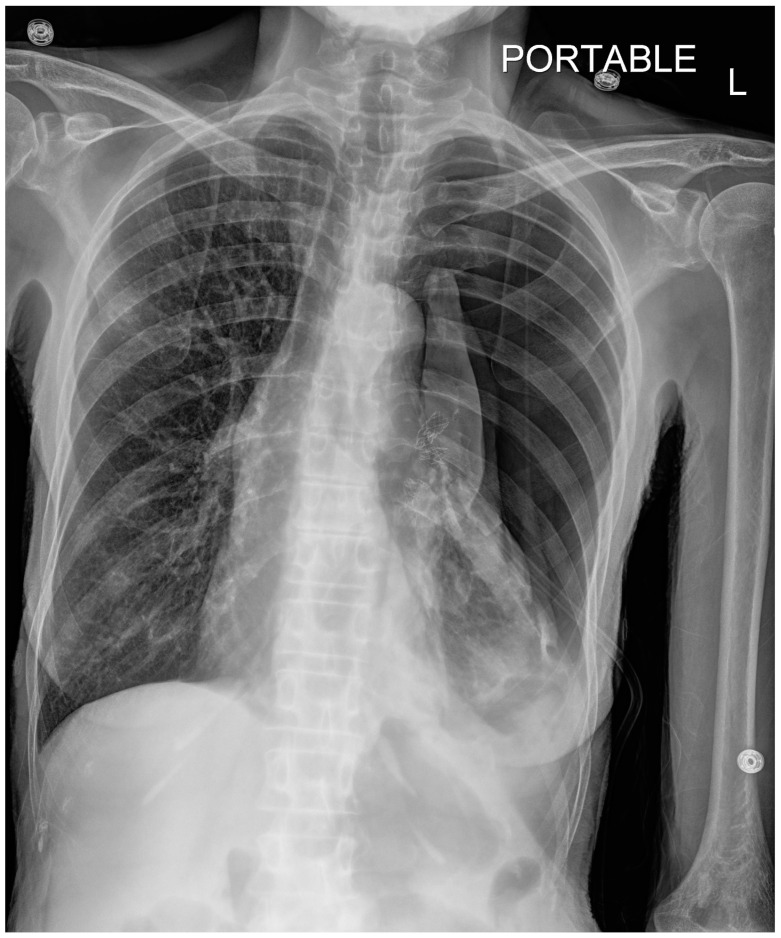
Chest X-ray – Tracheal deviation & mediastinal shift
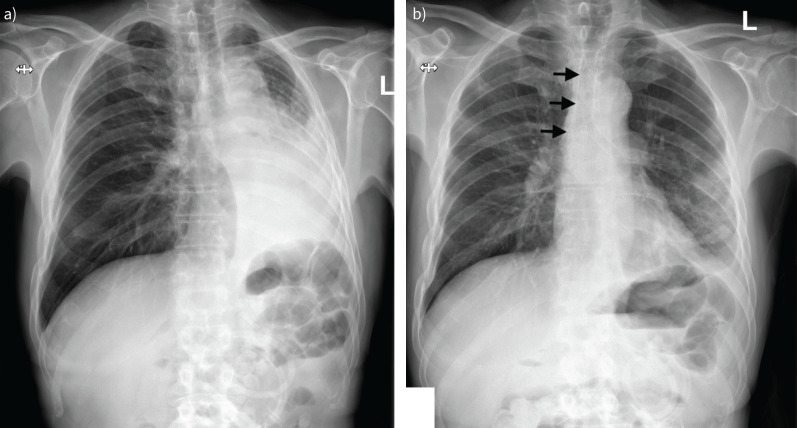
Chest X-ray – Tracheal shadow (bilateral pulmonary infiltrates)
Chest X-ray /CT – RMS endobronchial tumor
Chest X-ray/CT – LMB total occlusion (hilar mass with post-obstructive pneumonia)
Chest X-ray/CT Timeline – Pneumothorax management (drainage, stent placement, resolution)
Chest X-ray/CT – Left spontaneous pneumothorax (chest tube, air-fluid level, specimen)
Ultrasound – A lines (reverberation artifacts of pleuropulmonary interface)
Ultrasound – B lines (comet-tail artifacts, interlobular septa)
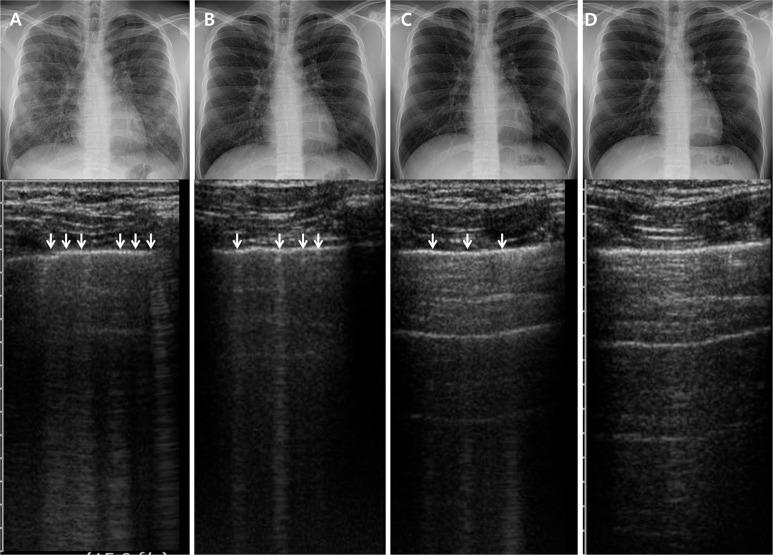
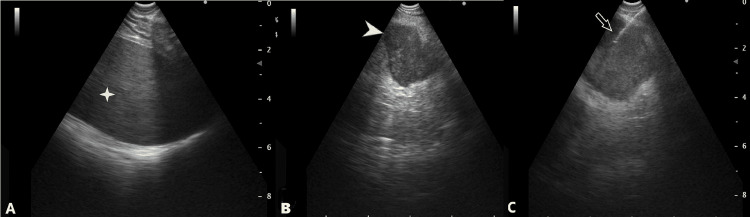
Ultrasound – B-lines timeline (days 1, 4, 7, 14)
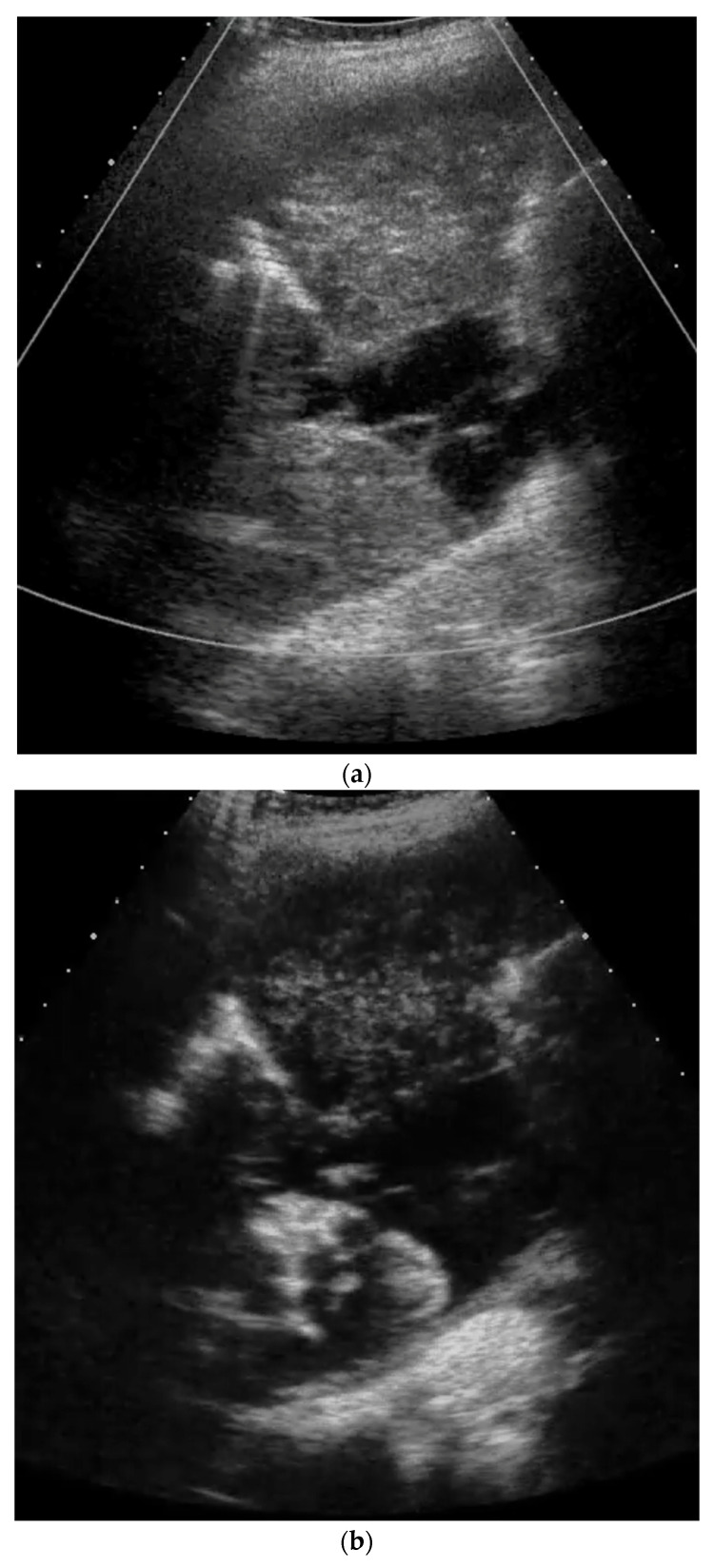
Ultrasound – Floating visceral pleura (atelectasis)
Ultrasound – Complex nonseptated pleural effusion (heterogeneous hyperechoic spots)
Ultrasound – Malignant pleural effusion (fibrinous septation)
Ultrasound – Mesothelioma (pleural effusion, tumor masses, diaphragm infiltration, rib fracture)
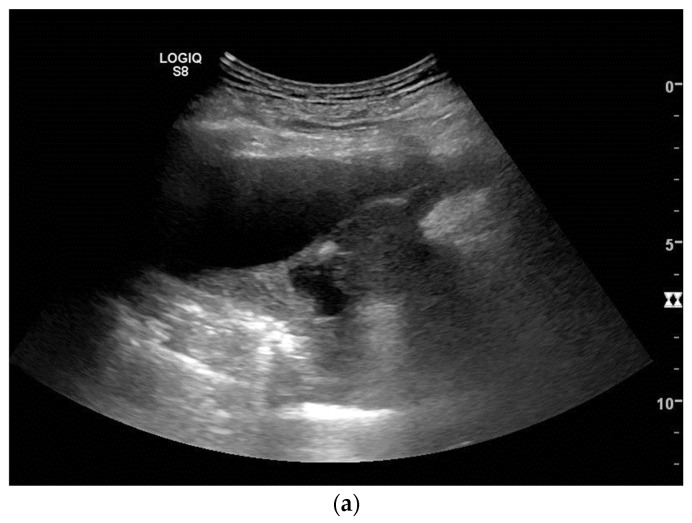
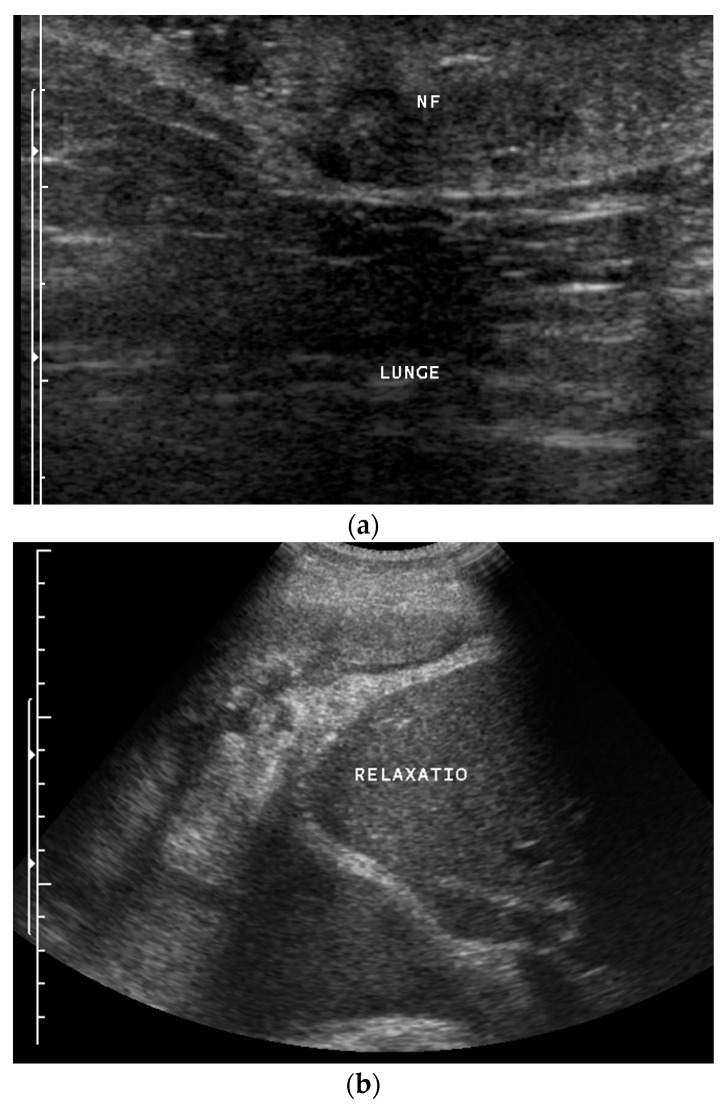
Ultrasound – Neurofibrosarcoma and neurofibroma (diaphragm paralysis, liver bulging)
Ultrasound – Pleural adhesions (diaphragmatic to collapsed lung)
Ultrasound – Pleural thickening (bat sign, oblique approach for rib shadow avoidance)
Ultrasound – Pleural thickening technique (transverse/longitudinal probe positioning)
Ultrasound – Pneumothorax (absent lung sliding at pleural line)
Ultrasound – Sonographic anatomy (chest wall layers, pleural line, probe comparison)
Spirometry/CT – Pre/post treatment comparison (tracheal tumor, flow-volume curves)
Post‑transplant – Stent for anastomotic dehiscence
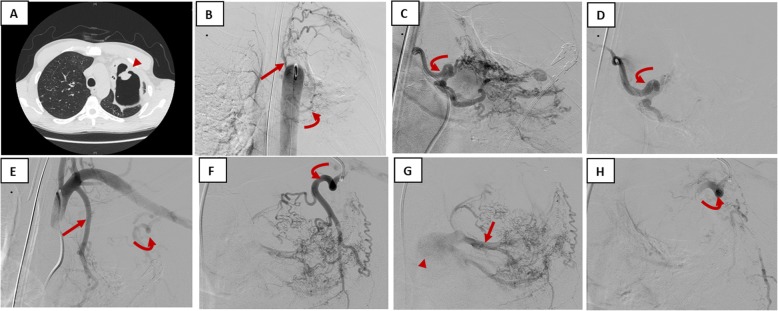
IR – Bronchial artery embolization for hemoptysis
Localization – CBCT‑assisted ENB marking
Localization – Lipiodol (CT‑guided)
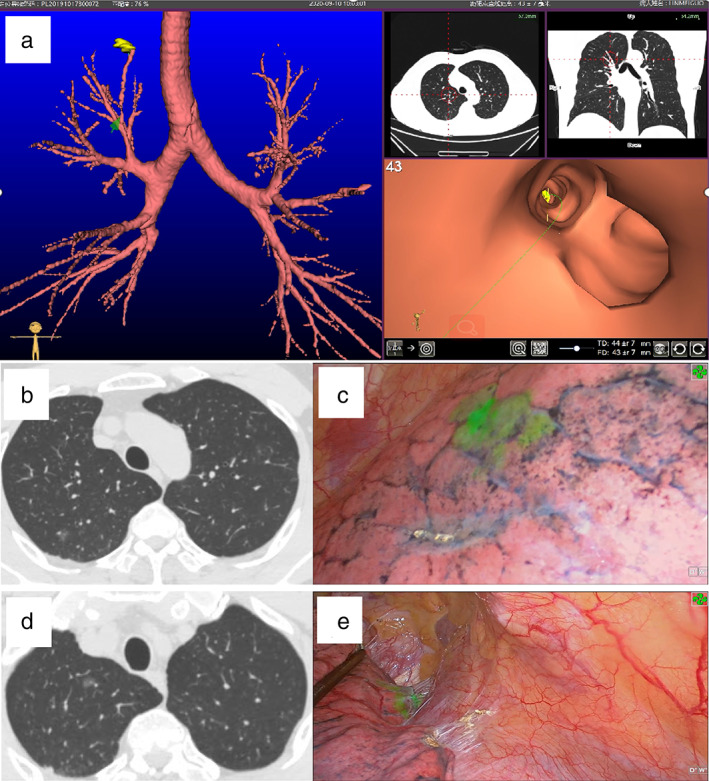
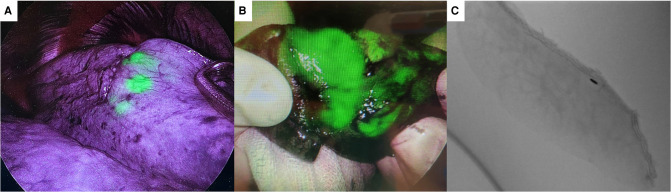
Localization – VNB‑guided ICG fluorescence
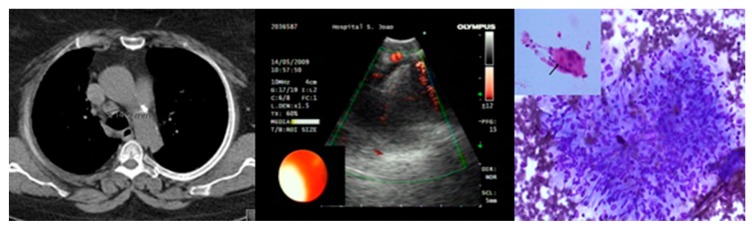
Ultrasound/CEUS – Primary lung sarcoma (pleural metastasis, enhancement patterns)
Ultrasound/CT Correlation – Pleural thickening (hypoecogenic lobular mass with circumferential pattern)
Ultrasound/CT Correlation – Pleural thickening localization (solid/cystic/complex characteristics)
Ultrasound/Pathology – Epithelioid mesothelioma (pleural effusion, solid tumor with biopsy)
CT/Chest X-ray – RMB and carina obstruction (Y-stent placement)
CT/Chest X-ray Correlation – Intratracheal tumor
CT/Fluoroscopy – Y‑stent implantation
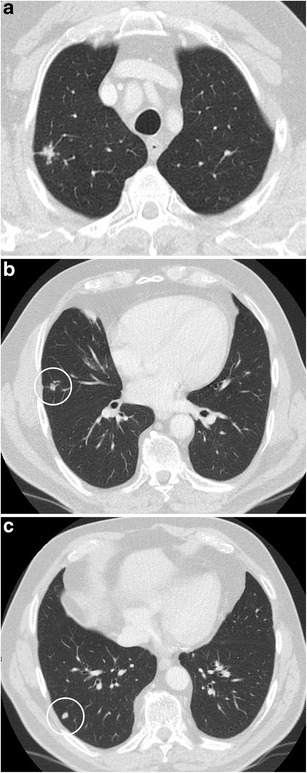
CT – Multiple nodules (carcinoid vs tuberculoma in oncology patient)
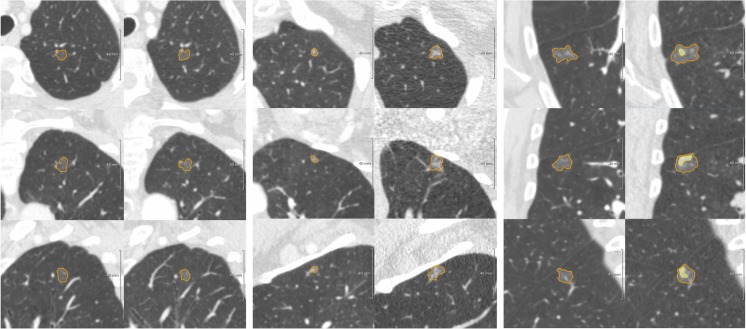
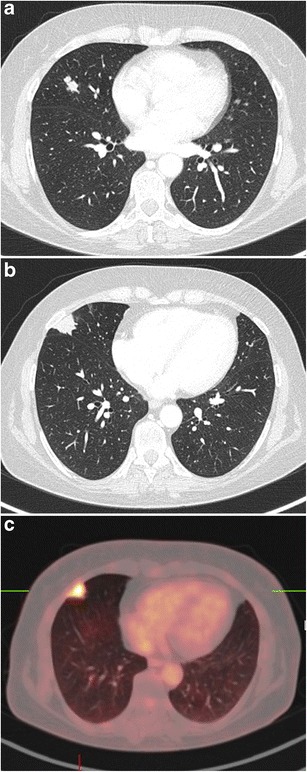
CT – Multiple pulmonary nodules (spiculated morphology, varied PET uptake)
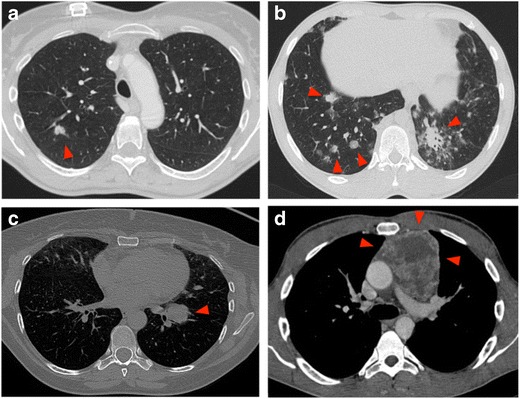
CT/PET-CT – Chest imaging (multiplanar correlation)
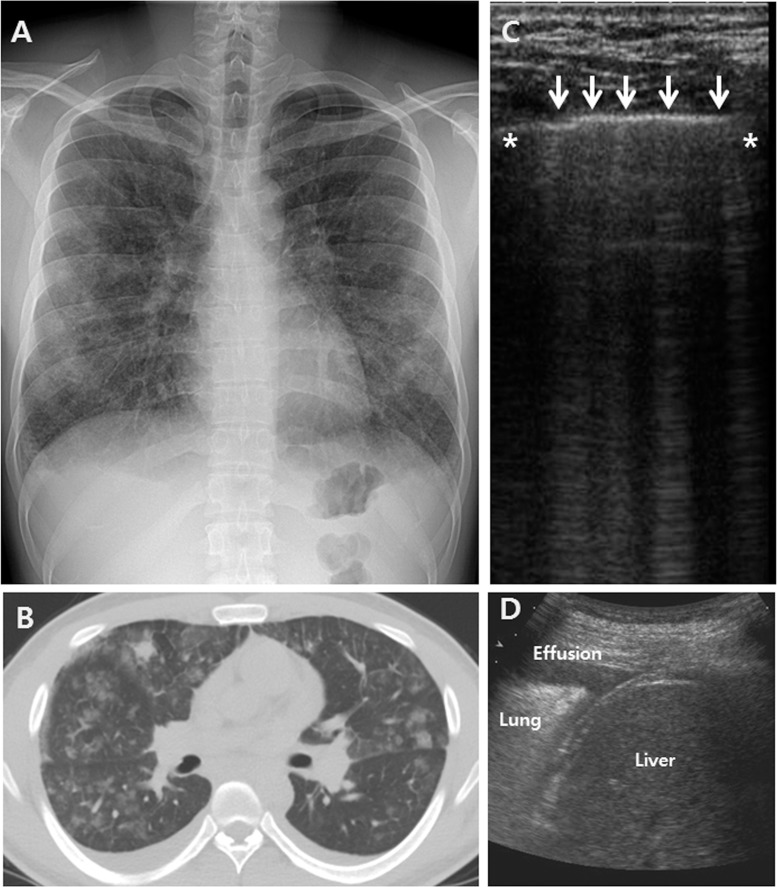
Chest X-ray/CT/Ultrasound – Bilateral GGO (interlobular septal thickening, B-lines, pleural effusion)
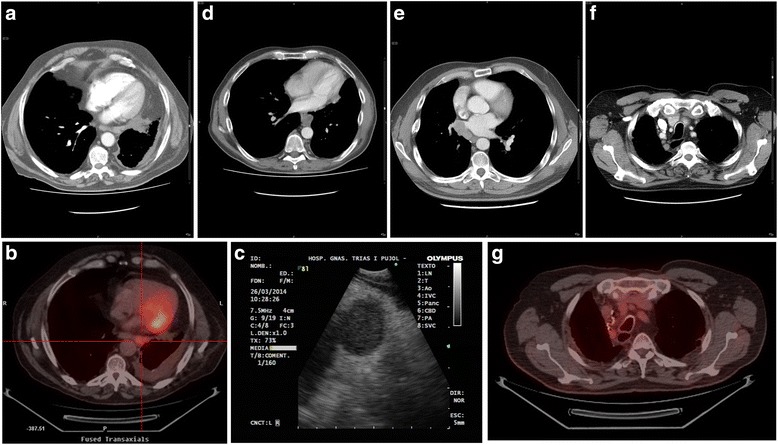
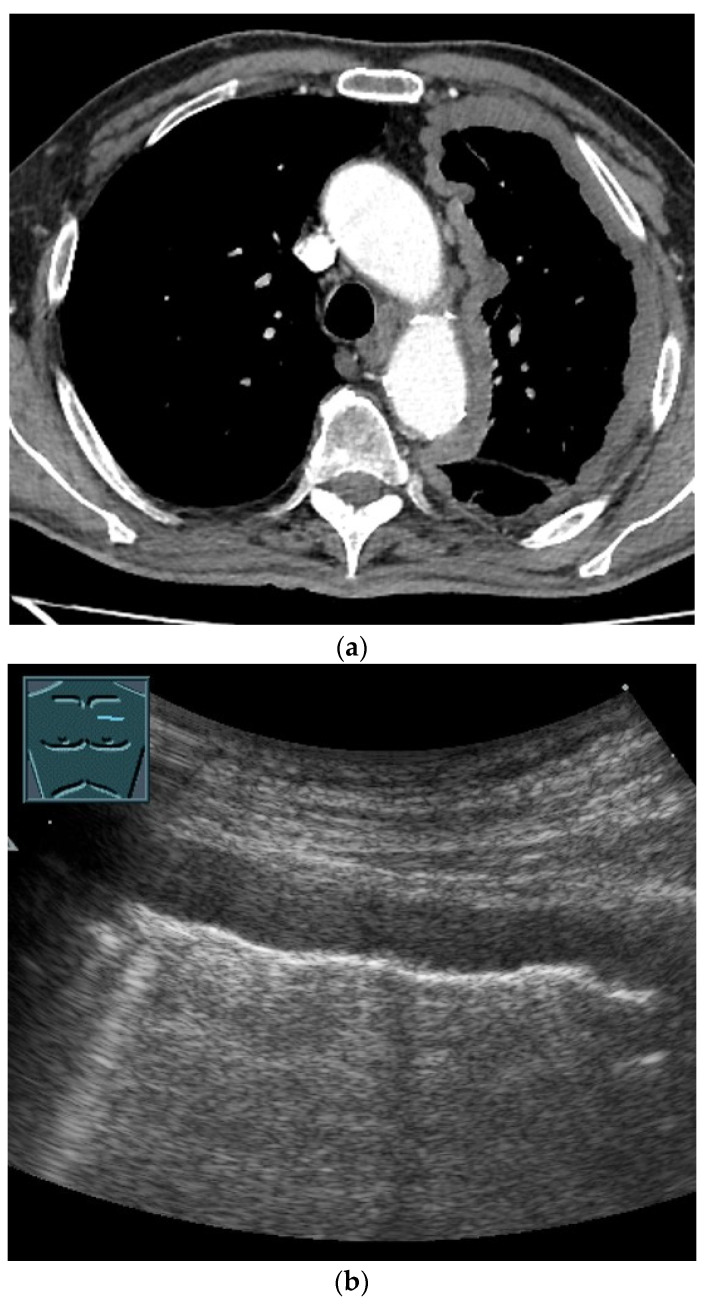
Chest X-ray/CT/Ultrasound – Mediastinal Hodgkin lymphoma (prevascular mass, airway compression, pleural effusion)
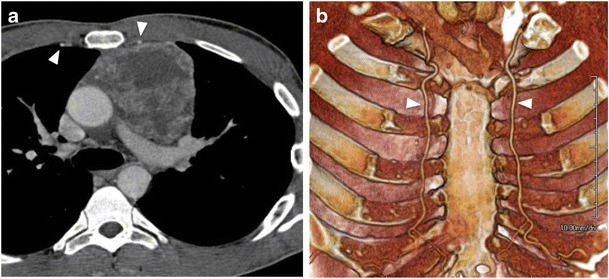
Anatomy – Internal mammary arteries on CT/3D
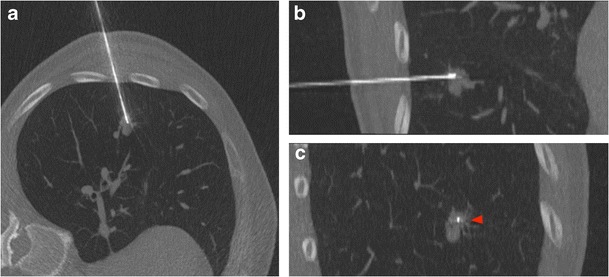
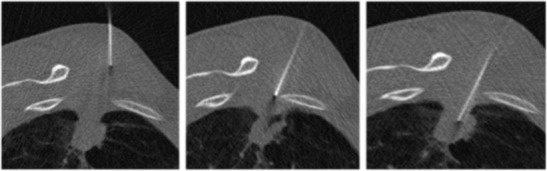
Biopsy – CT‑guided lung nodule (multi‑plane)
Biopsy – CT‑guided: hemorrhage complication
Biopsy – CT‑guided: indications
Biopsy – CT‑guided: pneumothorax complication
Biopsy – Fluoroscopy‑guided lung nodule
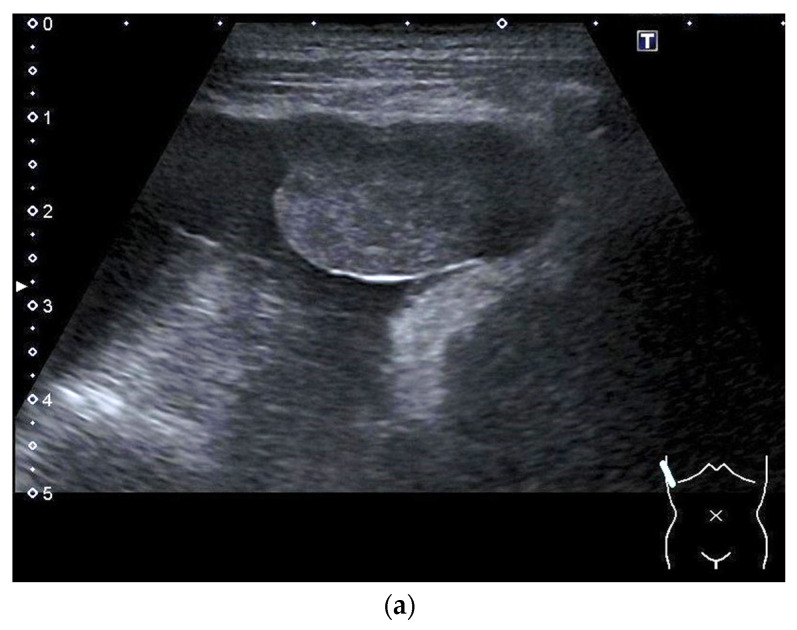
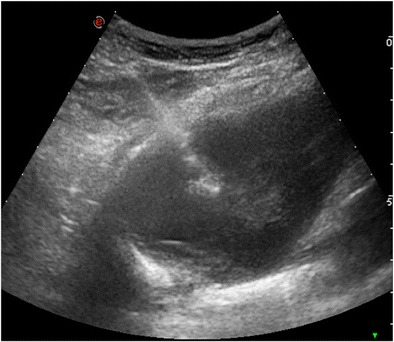
Biopsy – Ultrasound‑guided lung nodule
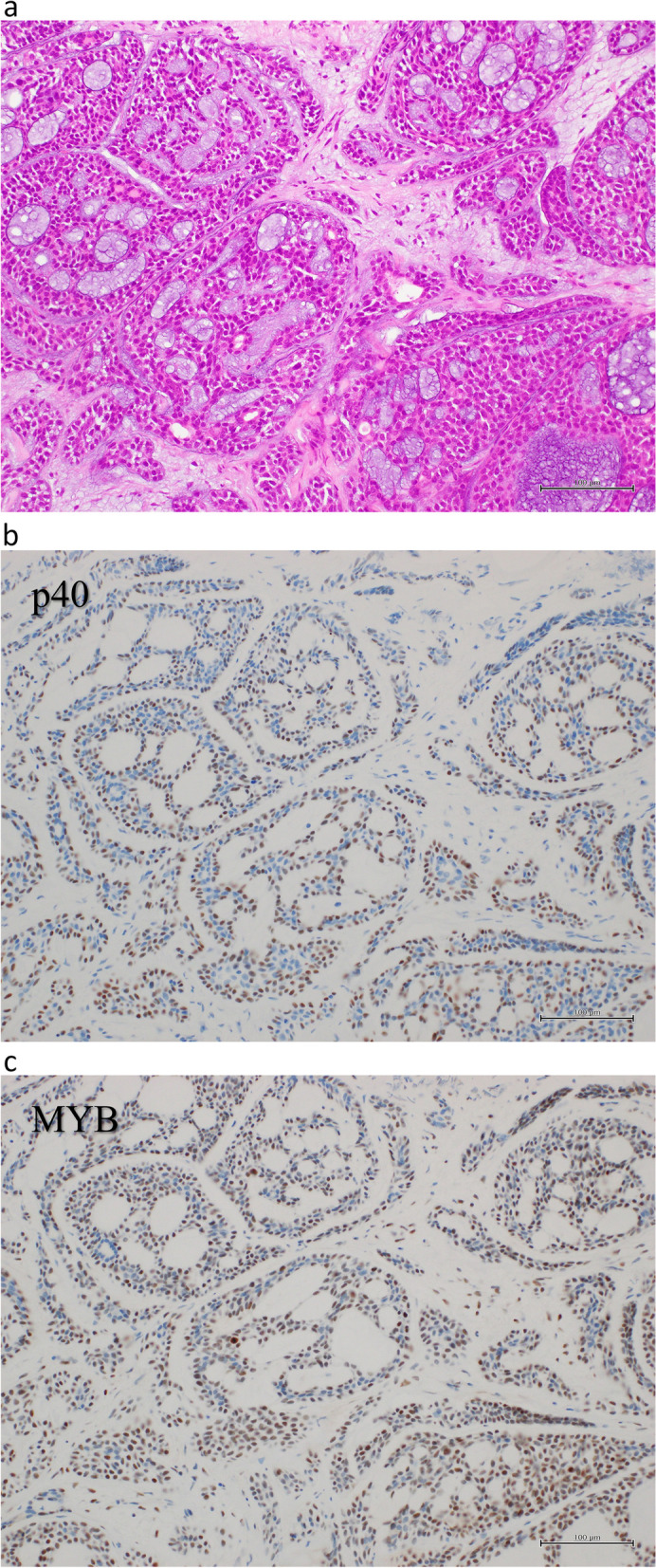
Adenoid cystic carcinoma (cribriform pattern, p40 and MYB IHC)
Adenoid Cystic Carcinoma (Cribriform Subtype)
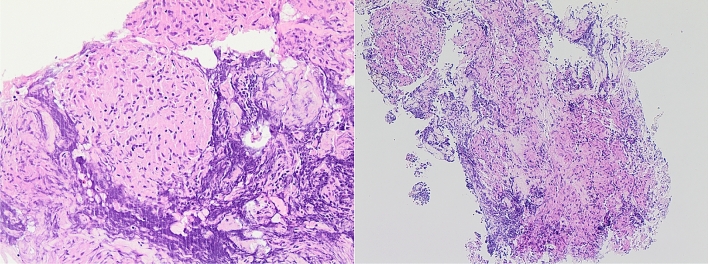
Cribriform tumor structure (H&E 40× and 200×)
Cytokeratin immunohistochemistry (negative)
EBUS thyroid aspiration (poorly differentiated adenocarcinoma, TTF1/CEA/CK7 IHC)
EBUS-FNA squamous cell carcinoma (H&E, p40 and CK14 IHC)
Endobronchial lipoma (mature adipose tissue with mucoid changes, H&E)
Endobronchial tumor (polypoid lesion, H&E with myxoid stroma)
Endobronchial tumor (pre- and post-ablation biopsy comparison, H&E)
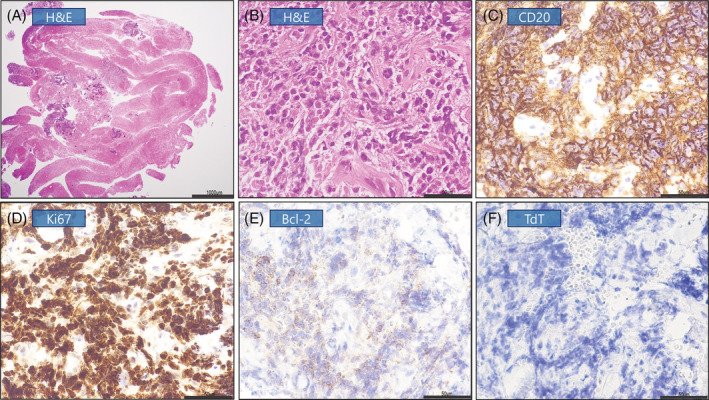
Immunohistochemistry panel (CD20, Ki67, Bcl-2, TdT)
Kaposi Sarcoma (Forceps vs Cryobiopsy vs FNA)
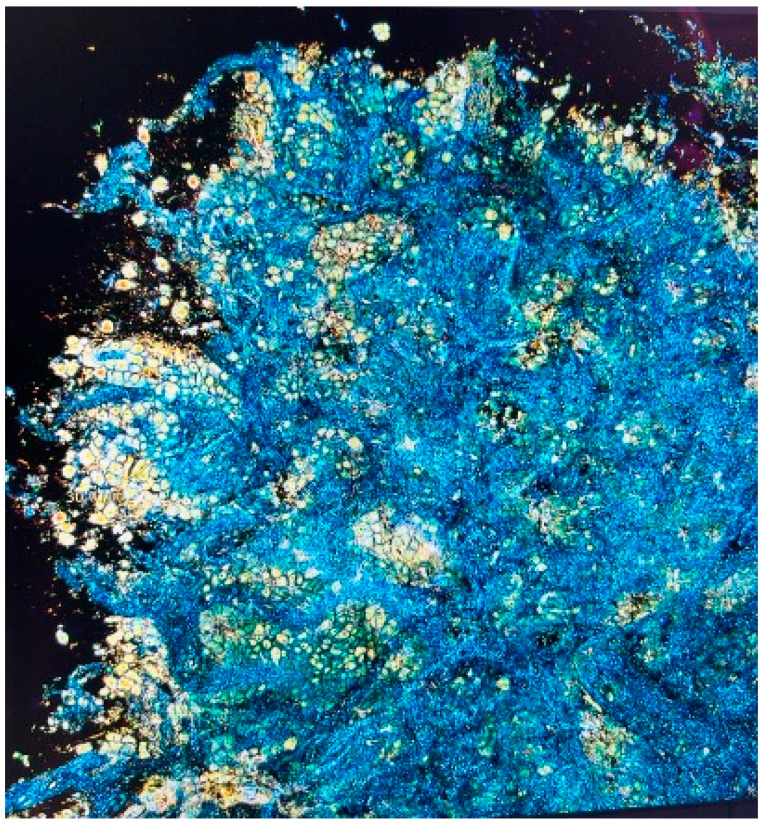
Lung cryobiopsy (H&E and ex-vivo confocal microscopy)
Lymph node squamous cell carcinoma (H&E low magnification)
Malignant mesothelioma (epithelioid and sarcomatoid, WT1 and calretinin IHC)
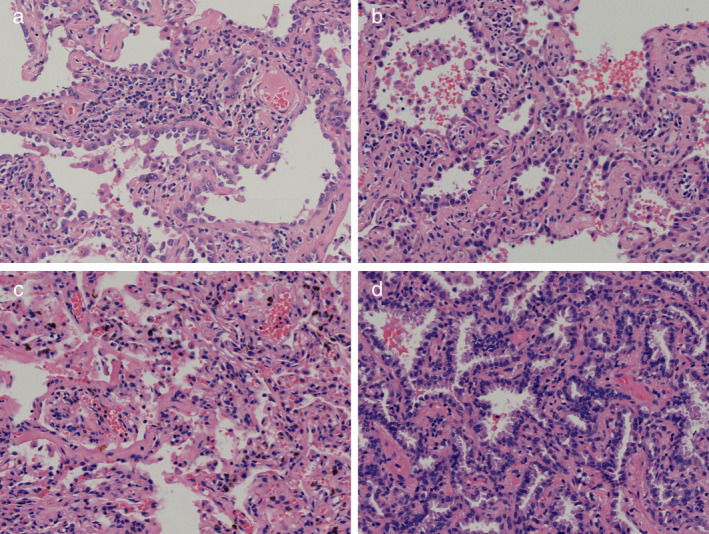
Multiple lung nodules (AIS, MIA, chronic inflammation, H&E)
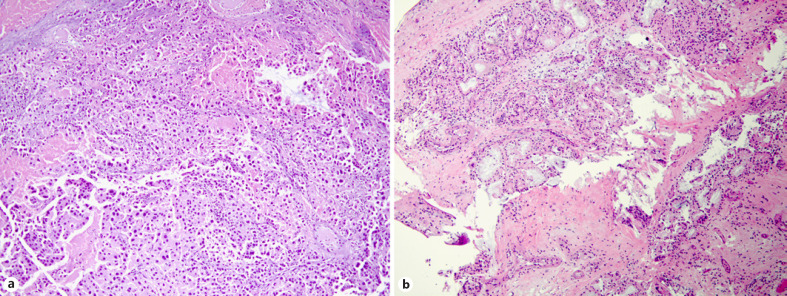
PLCH vs HP (fibromyxoid foci and interstitial fibrosis)
Pleural Endometriosis with Stromal Invasion
Pleuropulmonary blastoma (chondrosarcoma, glandular and blastemal components, H&E)
S-100 immunohistochemistry (positive)
Sarcoidosis granuloma (cytoblock with Crown Cut needle)
Tissue core and blood contamination evaluation (H&E slides)
Tracheal schwannoma (H&E with Antoni A/B areas, nuclear palisading)
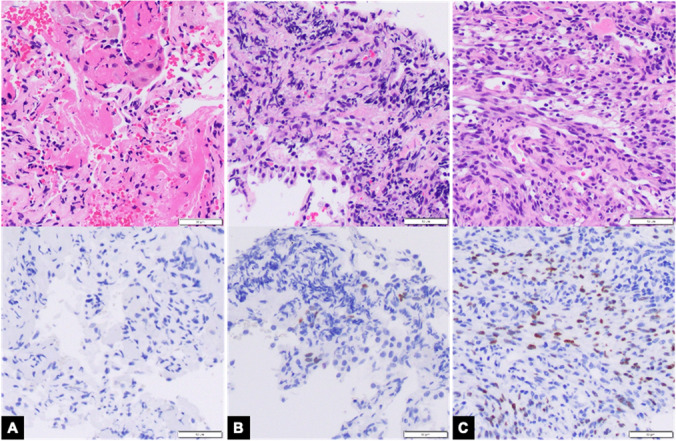
Tracheal Schwannoma (S100 Positive)
Transbronchial biopsy adenocarcinoma (RUL with ROSE, H&E)
Cytology – Adenocarcinoma cells (high N/C ratio, TTF1 IHC)
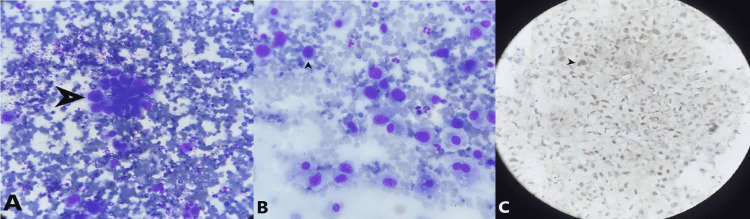
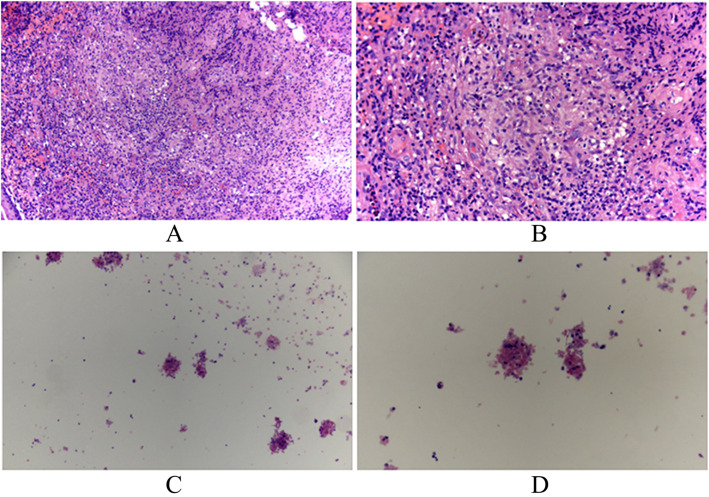
Cytology – Aspirated pus (epithelioid cells, lymphocytes, granuloma formation)
Cytology – EBUS-FNA cell block vs smear (subcarinal metastatic adenocarcinoma)
Cytology – Lymphocytes in aspirated material (H&E)
Cytology – ROSE classification (Class 3 vs Class 4 cluster density)
Cytology – ROSE from EBUS-FNA (22G Mediglobe needle)
ROSE/Pathology Comparison – Forceps vs cryobiopsy (metastatic urothelial carcinoma and adenocarcinoma)
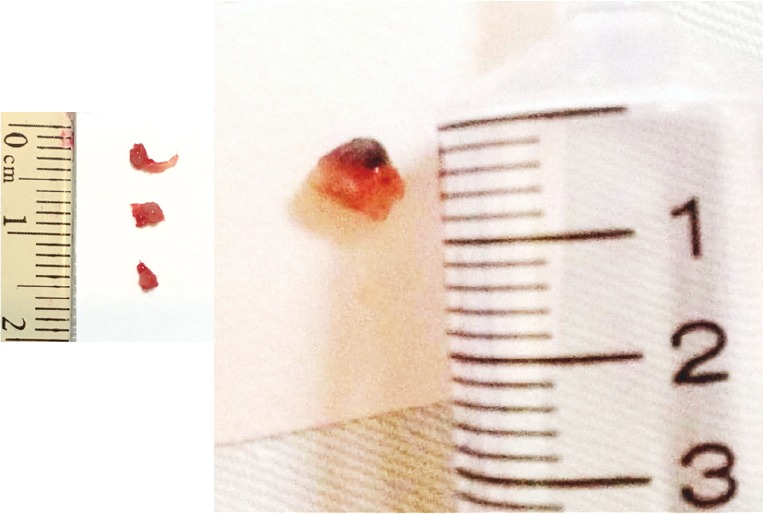
Specimen – Resected lung mass (RLL and RML)
Specimen Comparison – Forceps biopsy vs cryobiopsy
FFOCT-DCI – Technique description (high-resolution 3D biopsy imaging)
Digital Pathology – Quantitative analysis workflow (calibration and threshold measurement)
CT/Cytology – Mediastinal lymphadenopathy (small cell lung carcinoma, H&E)
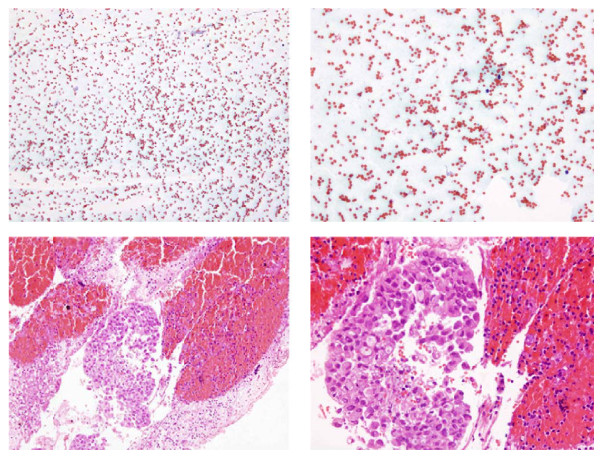
CT/Cytology – Mediastinal mass with necrosis (EBUS-TBNA adenocarcinoma)
CT/Pathology – Discordant histology (LUL mass, SCC vs adenosquamous carcinoma)
Confocal Laser Endomicroscopy – Squamous cell carcinoma vs adenocarcinoma (with cytology)
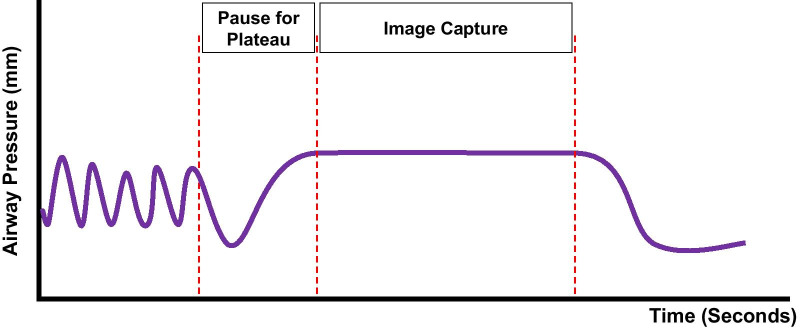
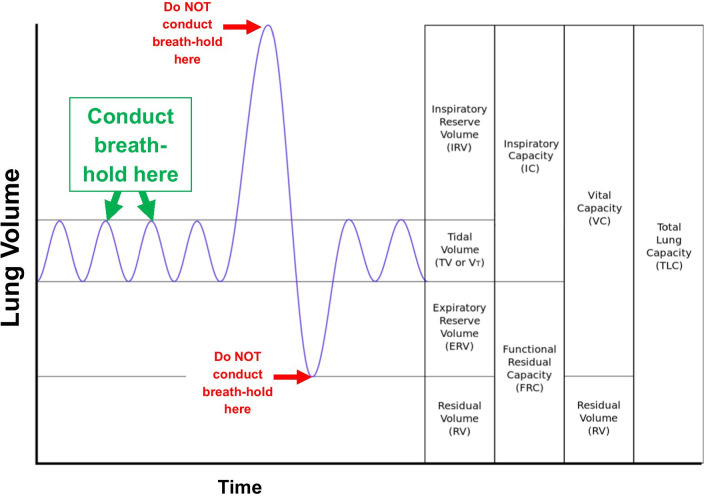
Protocol – Breath‑Hold Timing & Hemodynamics
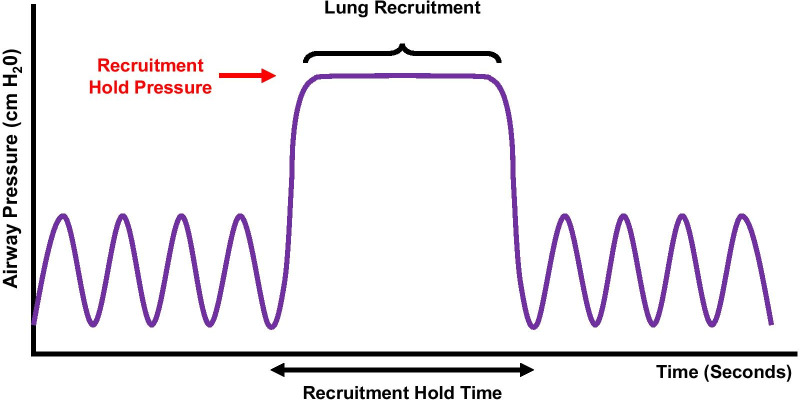
Protocol – Ventilation (Recruitment / PEEP / “40 for 40” Note)
Procedure – Sheath-free Amplatzer device deployment method (guide wire technique)
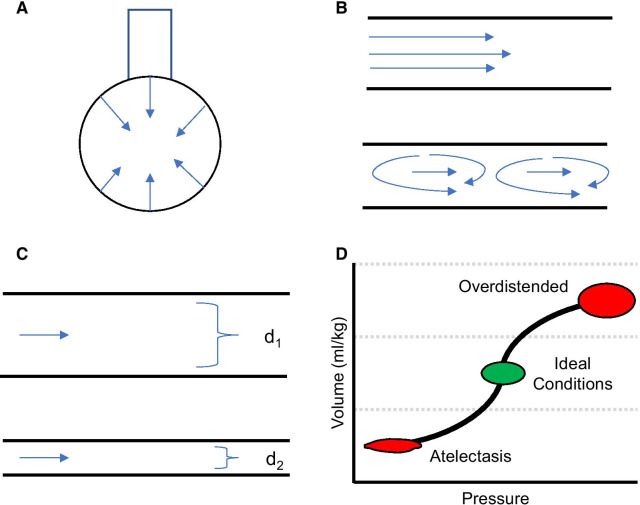
Physiology – Mechanisms of Atelectasis & Resistance (Diagram)
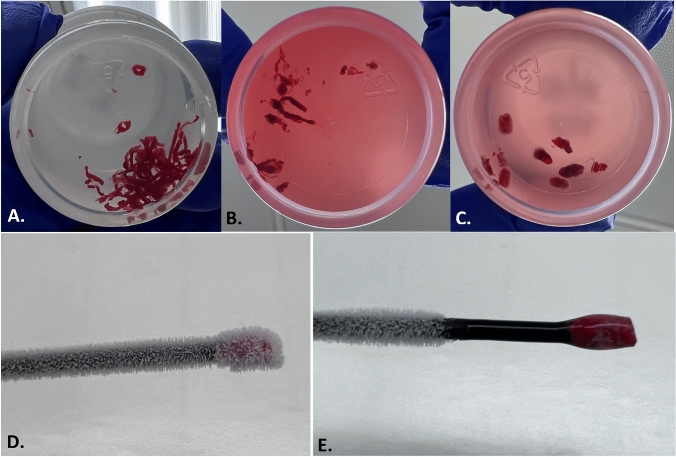
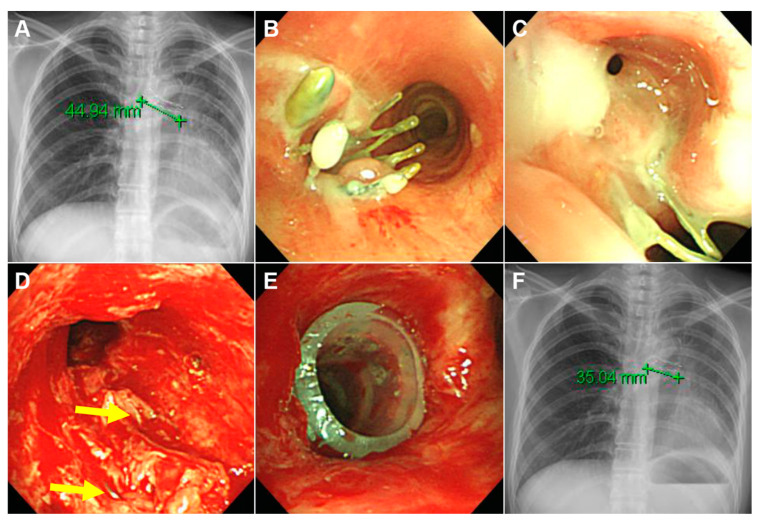
Foreign Bodies – Tracheobronchial specimens (dental device, nail, coin, grape)
Schematic – Flow‑Volume Loop Comparisons
Diagram – Breath-hold technique (peak inspiration for intraprocedural imaging)
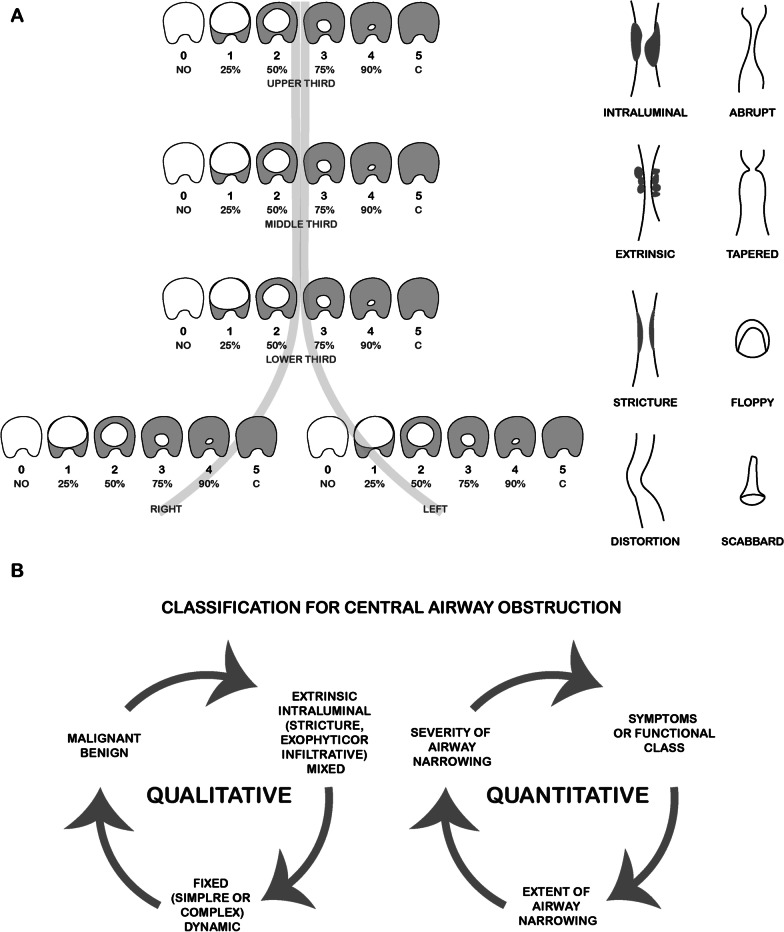
Diagram – Central airway obstruction types
Diagram – iSGS treatment approaches (dilation, resection, open surgery)
Diagram – Lung nodule localization (spatial relationship to pleural surface)
Diagram – Mediastinal lymph node stations (EUS, EBUS, combination coverage)
Diagram – MWA characteristics (ablation zones, oven effect, thermal sink effect)
Diagram – Normal vs iSGS trachea (anatomical comparison)
Diagram – SSN natural history (seven progression types, growth rate classification)
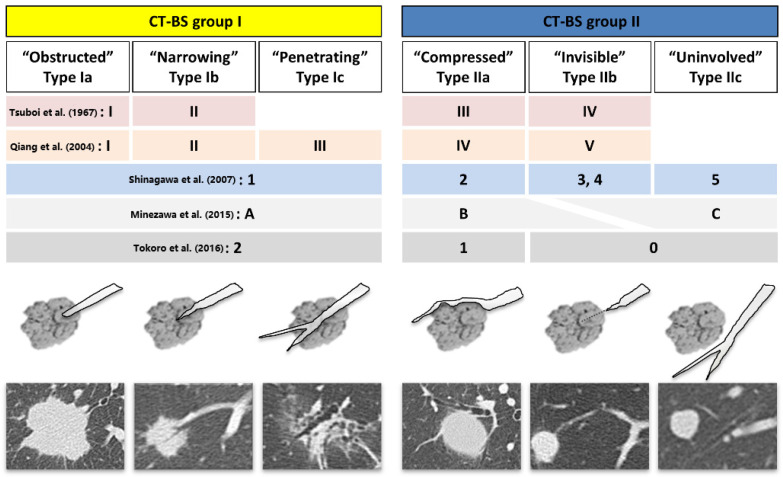
Classification – Bronchus sign types (CT-BS integrated schematic)
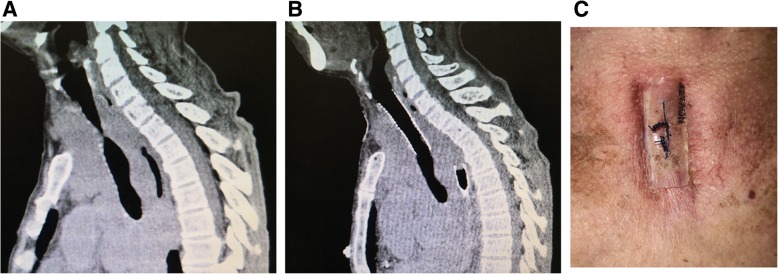
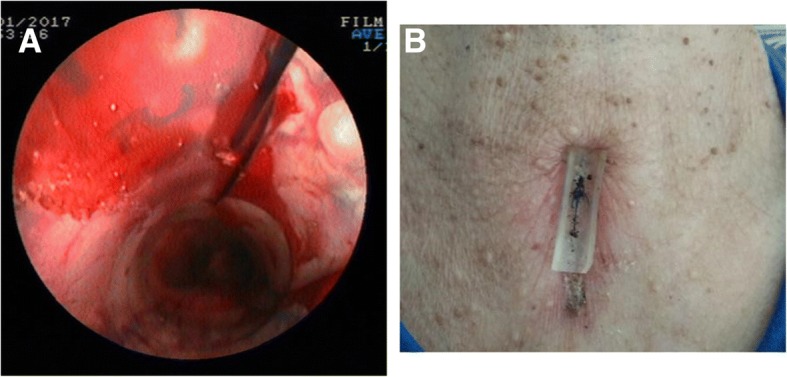
Clinical Images – Post-operative T-tube insertion
Airway Management – Endobronchial Blockers (Schematic)
Airway Management – Endobronchial Blockers (Types/Parts)
Airway Stenosis – Post‑intubation (CT & bronchoscopy)
Algorithm – Endobronchial-transbronchial ablation zones (anatomical guidance)
Algorithm – SSN 3D measurement index (CT histogram and texture features)
Anatomy – Secondary lobule diagram (artery lobularis and pulmonary artery branch)
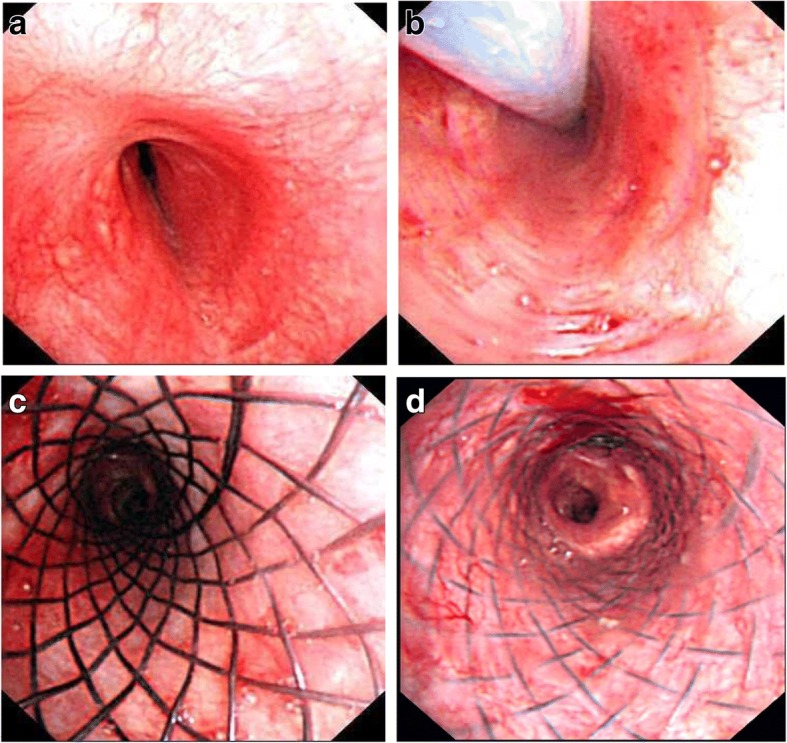
Bronchoscopic Images – Cobblestoning
CBCT‑Derived AF (Forceps/Cryobiopsy/Percutaneous)
ENB – CBCT Assistance (ICG Marking; Hybrid OR)
ENB – Edge Catheter (EWC SD180EWCTE‑FT)
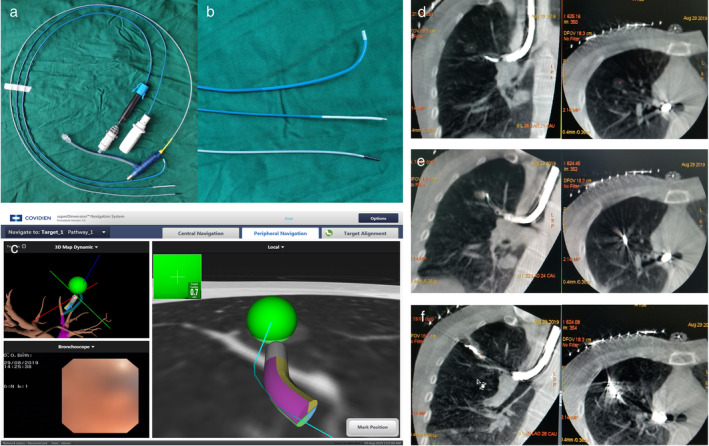
ENB – Equipment (Therapeutic Scope + EWC + Cryoprobe)
ENB – GGO Dye Marking (3D Recon + ENB Screen)
ENB – Illumisite (Fluoroscopic Navigation Set)
ENB – Pleural Dye Marking (Workflow)
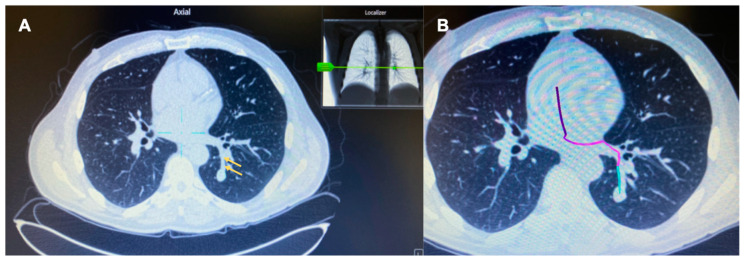
ENB – SuperDimension (Case 1 Mapping)
ENB – SuperDimension (Case 2 Mapping)
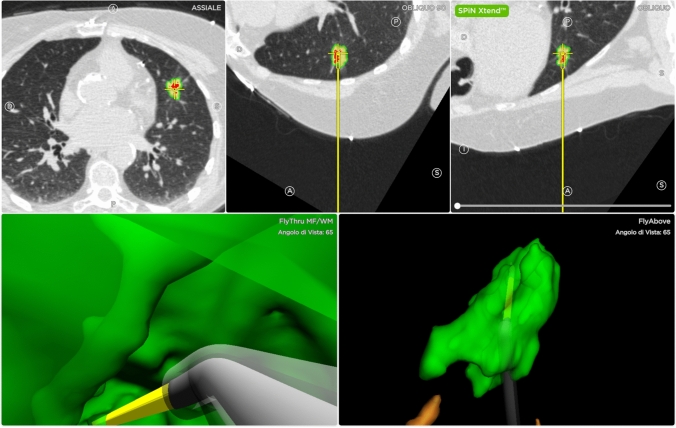
ENB – SuperDimension (Virtual Proximity at Target)
ENB (4D) – Multiplanar CT + Real‑Time Sampling
Hybrid OR – CBCT System (Ceiling‑Mounted)
Illumisite (Fluoro Navigation + Tomosynthesis)
Manual vs automated pathways (RB8 nodule with REBUS confirmation)
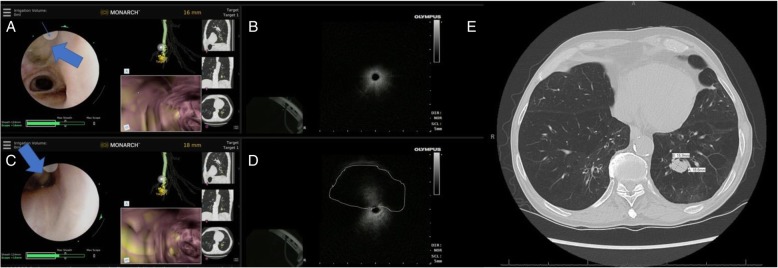
Monarch system interface (conventional and virtual bronchoscopic pathways)
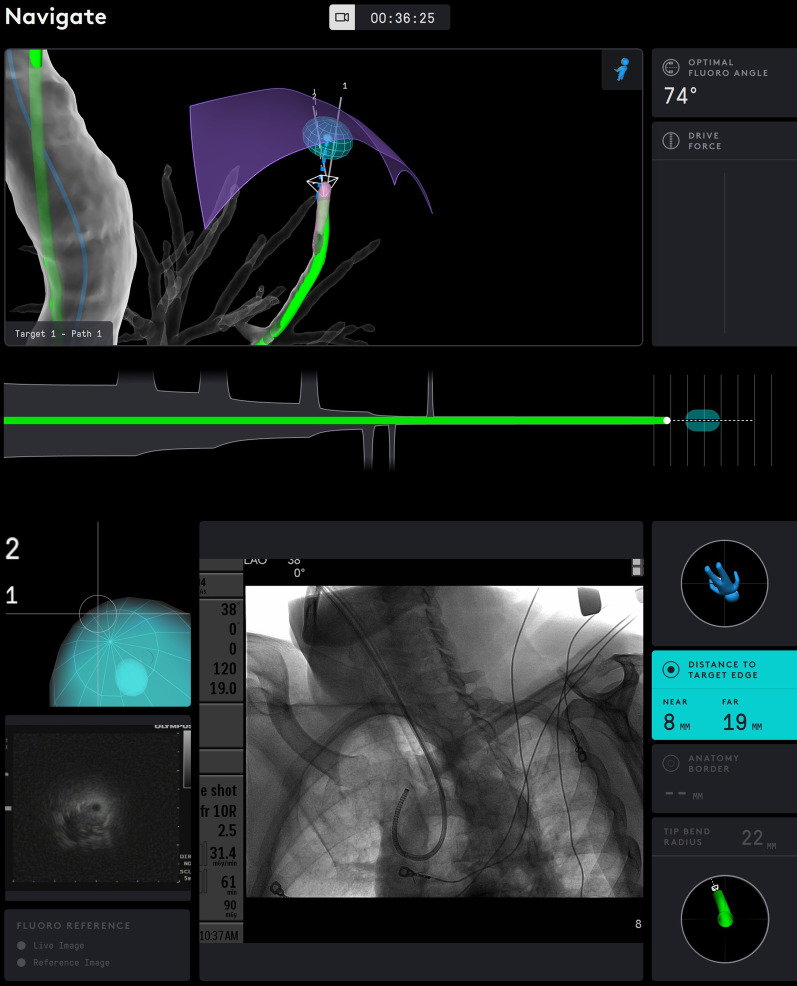
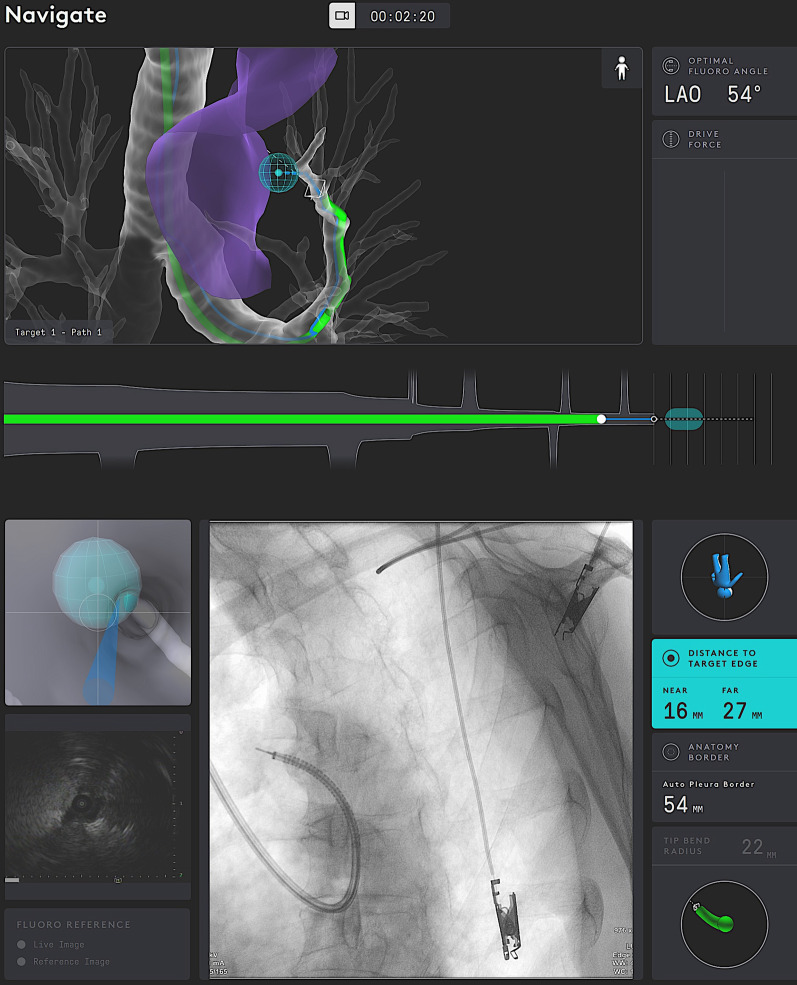
Robotic – Catheter Display with Distance Metrics
Robotic – CBCT Collision Awareness (Alignment)
Robotic – Controller Interfaces (Ion/Monarch/Galaxy)
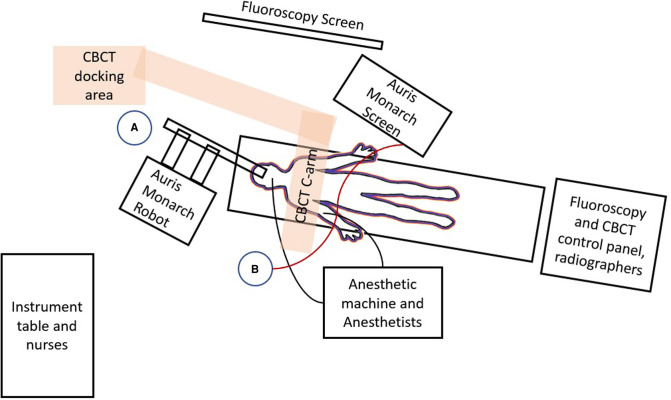
Robotic – Floor Plan (Hybrid OR Layout)
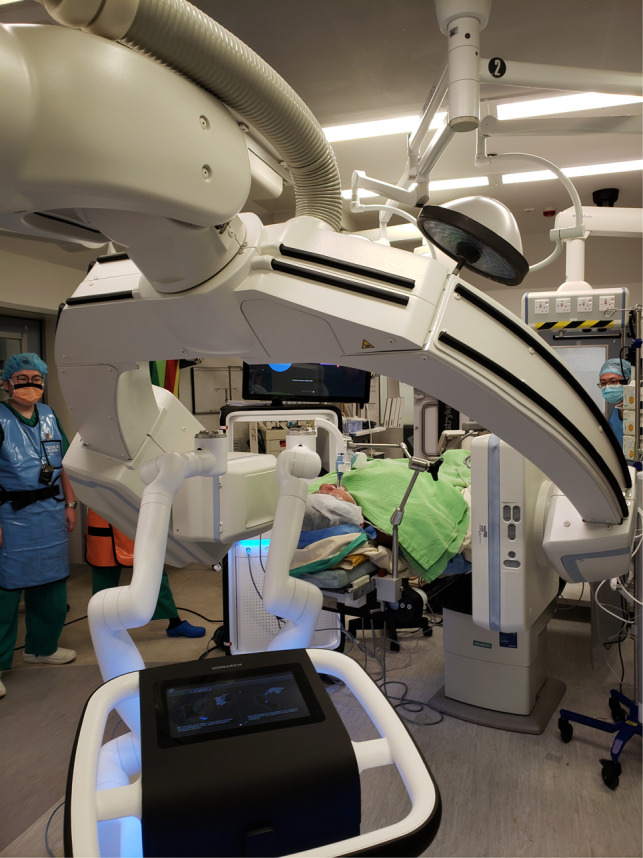
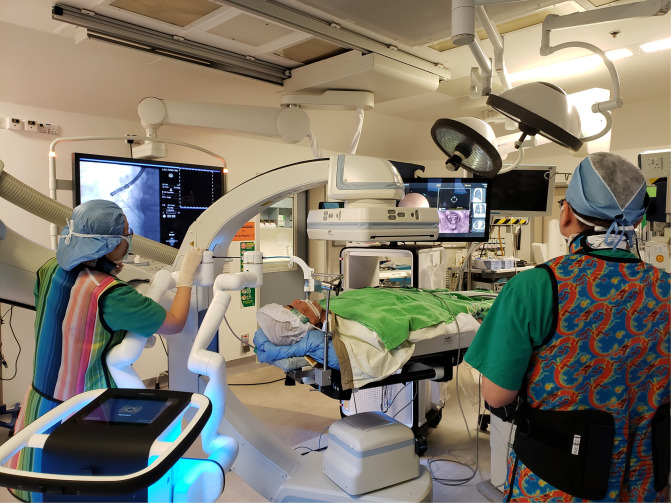
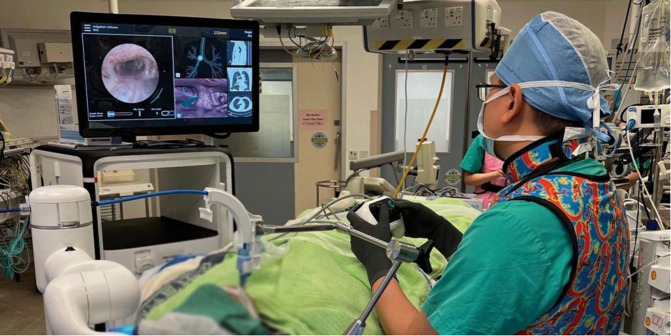
Robotic – Hybrid OR Workflow (Team & Screens)
Robotic – Ion + CBCT (Multiplanar Tool‑in‑Lesion)
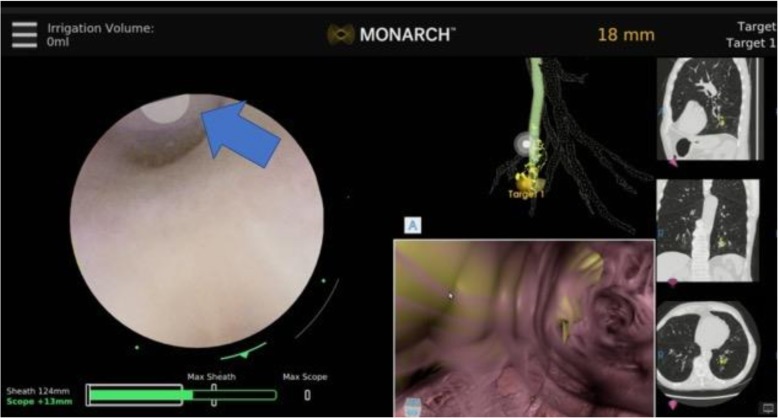
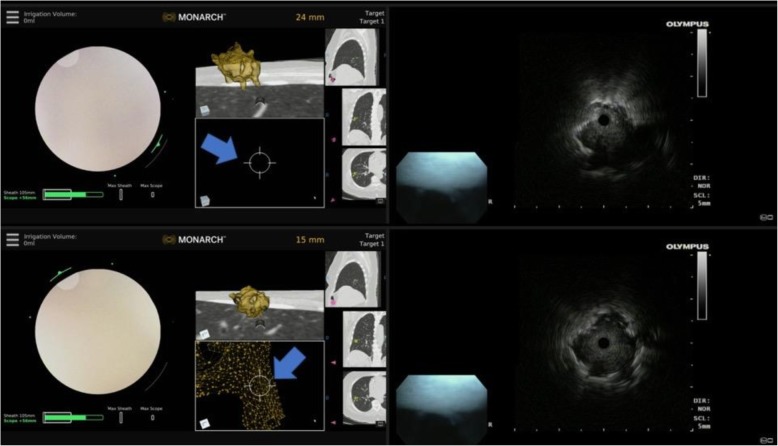
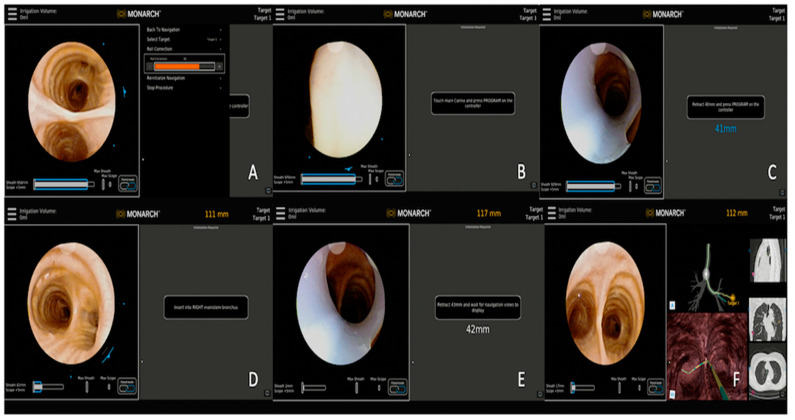
Robotic – Monarch (Multiscreen Panels)
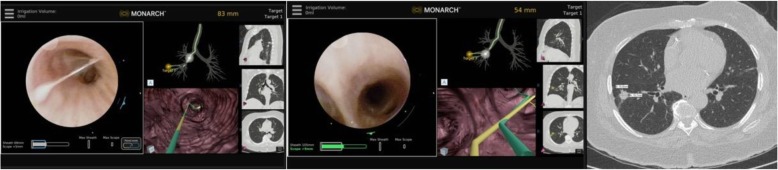
Robotic – Monarch + CBCT in Hybrid OR
Robotic – Multisource Display (Fluoro/EBUS/CT)
Robotic – Needle Aspiration (Tool Exit Orientation)
Robotic – REBUS Patterns (Eccentric → Concentric)
Robotic – REBUS Target Relationship (Probe Orientation)
Robotic – Registration Steps (Ion Example)
Robotic – Setup with Artis Zeego CBCT
Robotic – System Comparison (Yield & Tech)
Robotic – System Gallery (Monarch/Ion/Galaxy)
Robotic – Unicorn RAB System (China)
Robotic bronchoscopy interface (real-time and virtual bronchoscopic views)
Robotic system interface (real-time scope view, RUL nodule pathway)
Room Setup (Fixed C‑Arm; Bronchoscopy Positioning)
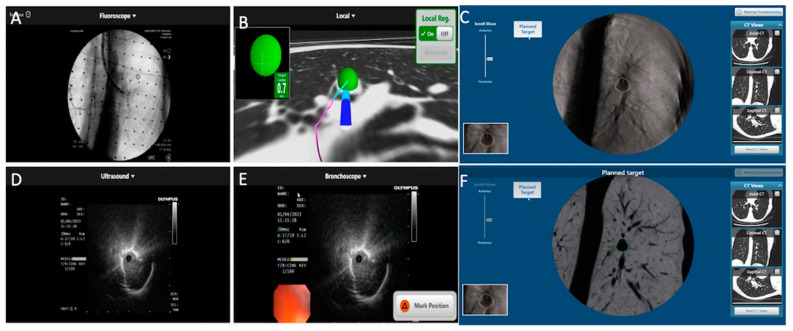
VBN + CBCT (Tip‑in‑Target Confirmation)
Virtual Bronchoscopy – Path Planning (Fly‑Through)
Virtual Bronchoscopy – Planning (Multiplanar Views)
Virtual Bronchoscopy – RFID Tag Placement (CT Correlation)
Virtual Bronchoscopy – Route/Target Overlay
ENB – Virtual-assisted lung mapping (LG catheter, indigo carmine injection sequence)
CT/CBCT – DTS reconstruction (ART vs prior-aided, registered views)
CT/CBCT – Lung abscess drainage (rEBUS localization, needle placement, follow-up resolution)
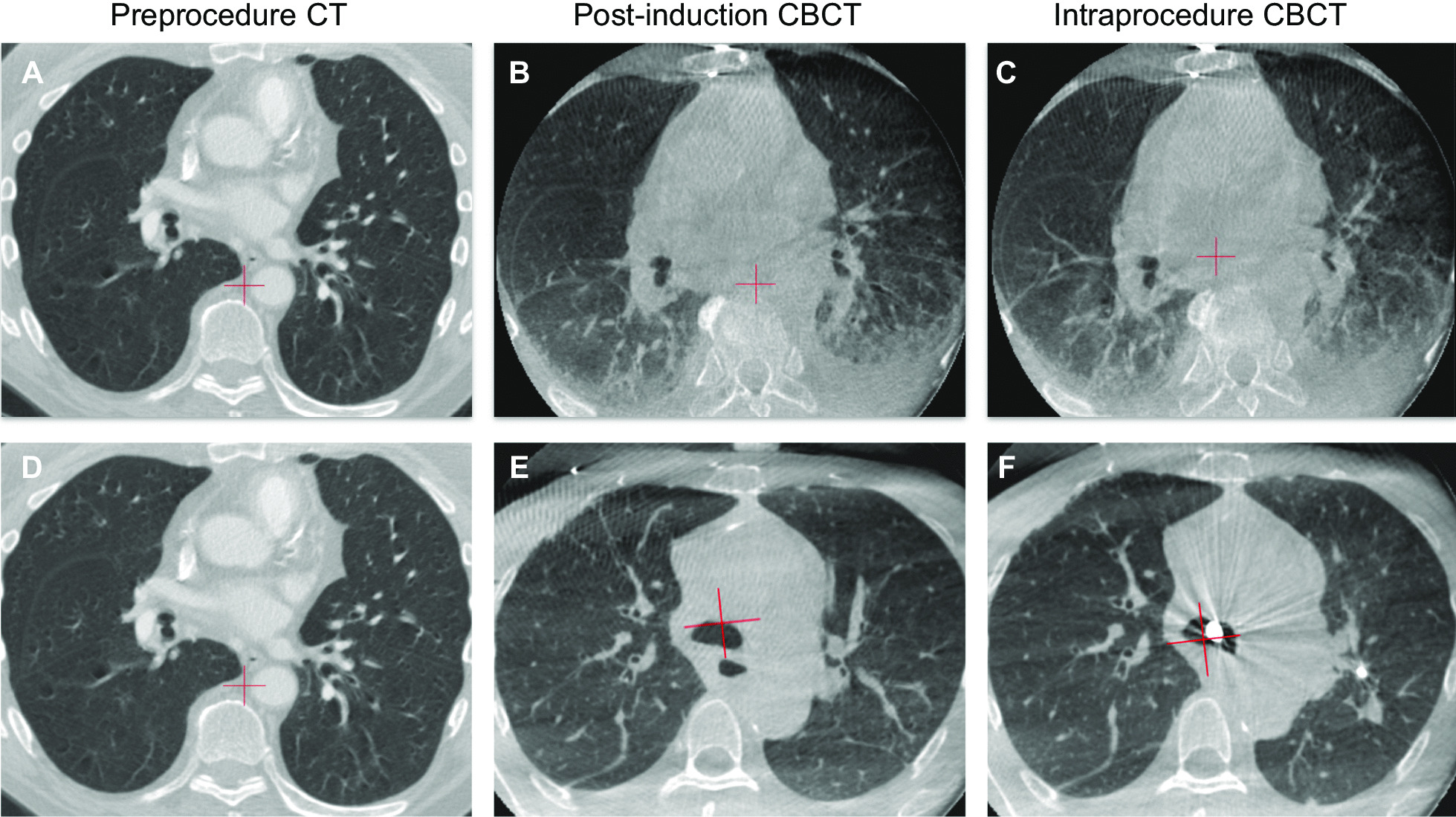
CT/CBCT Comparison – Atelectasis artifact (with and without ventilation protocol)
CT/CBCT/EBUS – LLL nodule (CBCT-AF with EBUS-TBB, adenocarcinoma diagnosis)
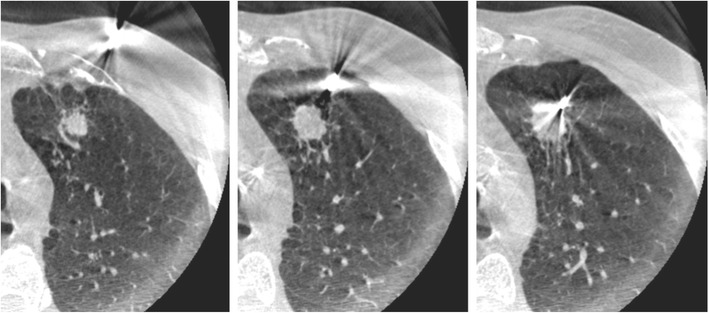
CBCT – Lung nodule (center strike, multiplanar views)
CBCT – Percutaneous nodule marking guidance
CBCT–DTS – Patient (CT vs intra‑op CBCT)
CBCT–DTS – Patient reconstruction (PL DTS)
CBCT–DTS – Phantom (CT vs intra‑op CBCT)
CBCT–DTS – Phantom reconstruction (PL DTS)
CBCT–DTS – Phantom reconstruction (SE DTS)
Bronchoscopic Images/Pathology – ENB-guided methylene blue injection (S2a subsegmental, adenocarcinoma)
Bronchoscopic Ablation – Microwave (CBCT verification)
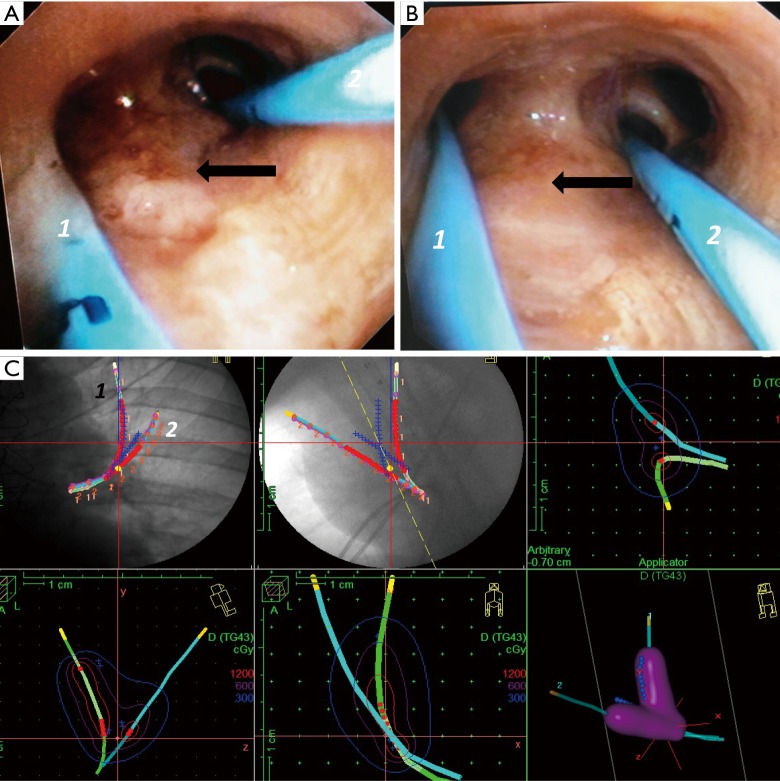
Brachytherapy – Endobronchial infiltration (LUL catheter placement and dose planning)
Bronchopleural Fistula – AD implantation (post-RML/RLL lobectomy)
Bronchopleural Fistula – AD implantation with CT/bronchoscopy correlation (post-LUL lobectomy)
Bronchoscopic Ablation – Argon plasma debulking
Augmented Fluoroscopy – Bronchoscopic localization
Augmented Fluoroscopy – Coil deployment view
Ablation – Fluoroscopy-guided cryoprobe with EBUS (1.1mm)
RAB – Integrated multimodal monitors
RAB – Microwave ablation platforms
RAB – Navigation alignment (no rEBUS)
Robotic Bronchoscopy – Navigation platforms (Monarch, Ion, Galaxy with TILT technology)
Ultrathin Bronchoscopy – rEBUS views & sampling
Fluoroscopy/CBCT – Multimodal navigation (RAB tool-in-lesion confirmation)
Fluoroscopy/Chest X-ray – Visicoil fiducial markers (triangulated pattern, augmented fluoroscopy)
Fluoroscopy – Transbronchial biopsy techniques (ultrathin vs thin bronchoscope with guide sheath)
Hybrid OR – CBCT‑guided bronchoscopy setup
Hybrid OR – Mobile CBCT (Cios Spin) setup
Image Processing – Registration algorithm comparison (MSE, MoMSE, improved MoMSE)
Diagram – DTS scan orbits (SE and PL trajectories)
Diagram – Robotic bronchoscopy room setup (Monarch, Ion, Galaxy platforms)
Biopsy – CBCT‑guided lung nodule
Biopsy – Specimen comparison (needle, forceps, cryobiopsy gross and frozen)
Biopsy – Transbronchial cryobiopsy procedure (RLL, ILD, fluoroscopy-guided)
RATS – Azygos vein exposure
RATS – Post‑azygos division
Conventional VAL-MAP technique (step-by-step)
CT-guided cyanoacrylate localization
CT-guided indocyanine green localization
CT-guided memory alloy coil localization
Lungpro-assisted metallic marker localization
RFID marker placement (wedge resection steps)
VAL-MAP 2.0 technique (step-by-step)
Intraoperative Imaging – ICG dye localization (VATS with fiducial marker)
Intraoperative Imaging – NIR fluorescence with ICG (Firefly mode vs white-light)
Fluoroscopy/Pathology – Lung nodule resection confirmation (ICG-coil marker, specimen)
Forensics – Tracheal ring injuries (autopsy)
Magnetic Navigation – Pulmonary nodule localization (RUL, methylene blue, thoracoscopic verification)
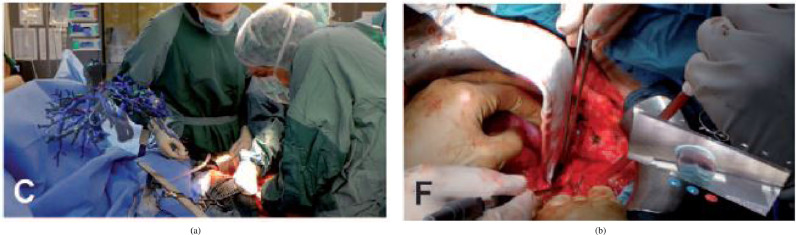
Telemedicine – Intra‑op 3D anatomy & consult
Ultrasound – Intraoperative pulmonary nodule localization
VAL-MAP – Dual dye technique (indigo carmine and ICG with NIR thoracoscopy)
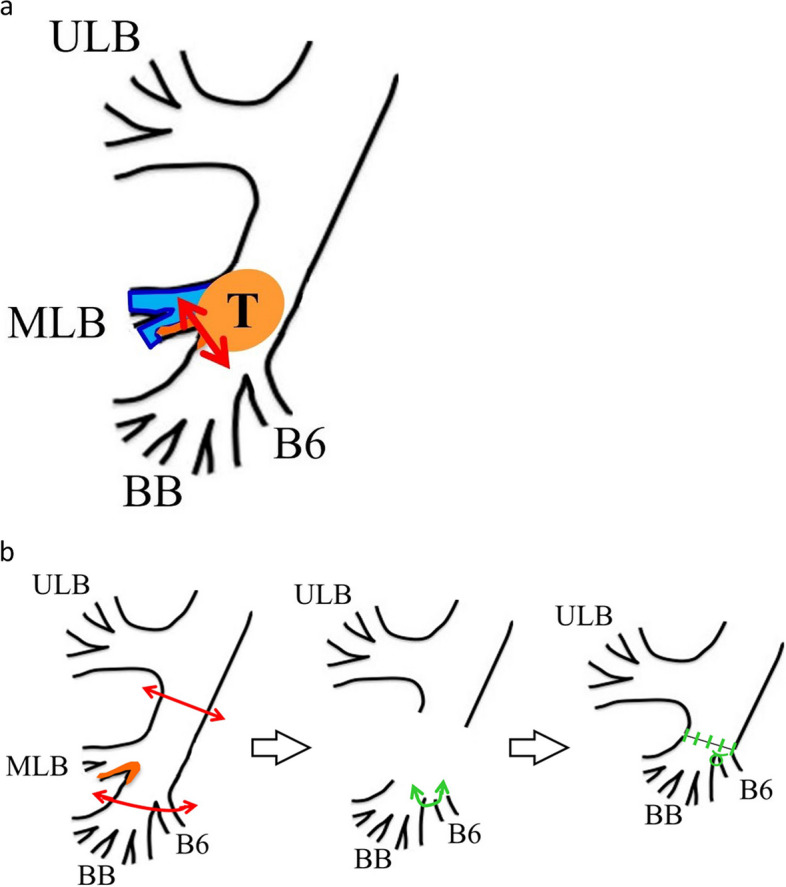
Diagram – Endobronchial tumor resection (electrocautery snare and RML sleeve lobectomy)
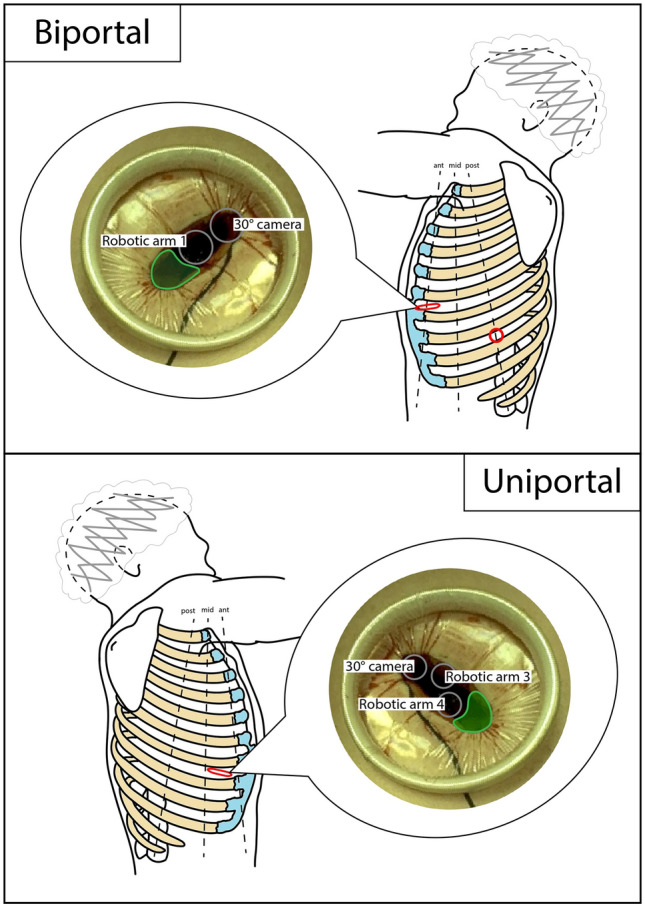
Diagram – RATS biportal and uniportal access positioning (schematic)
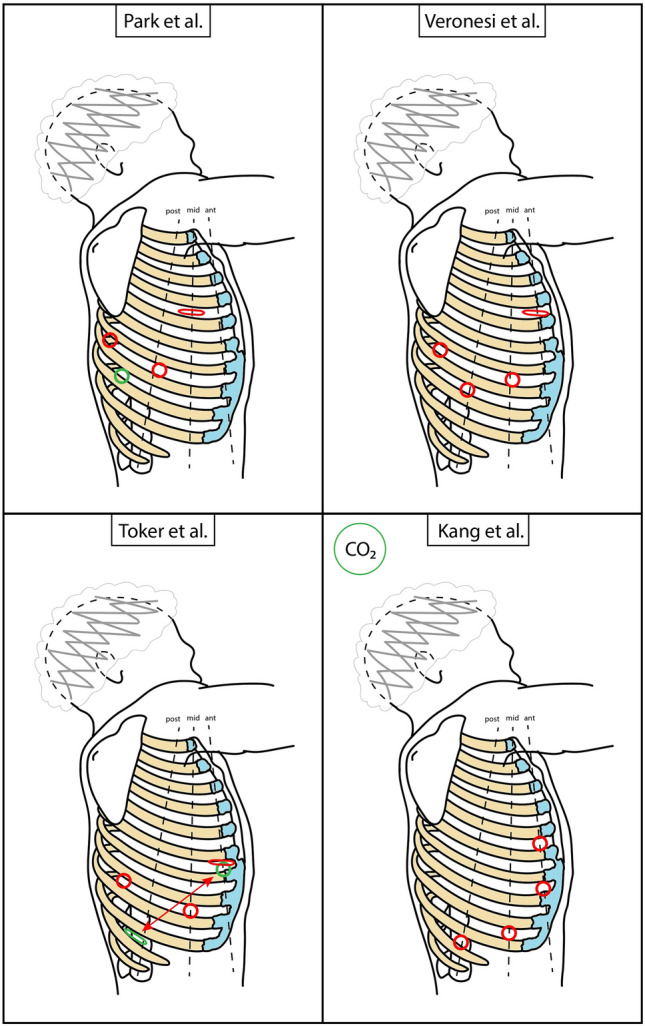
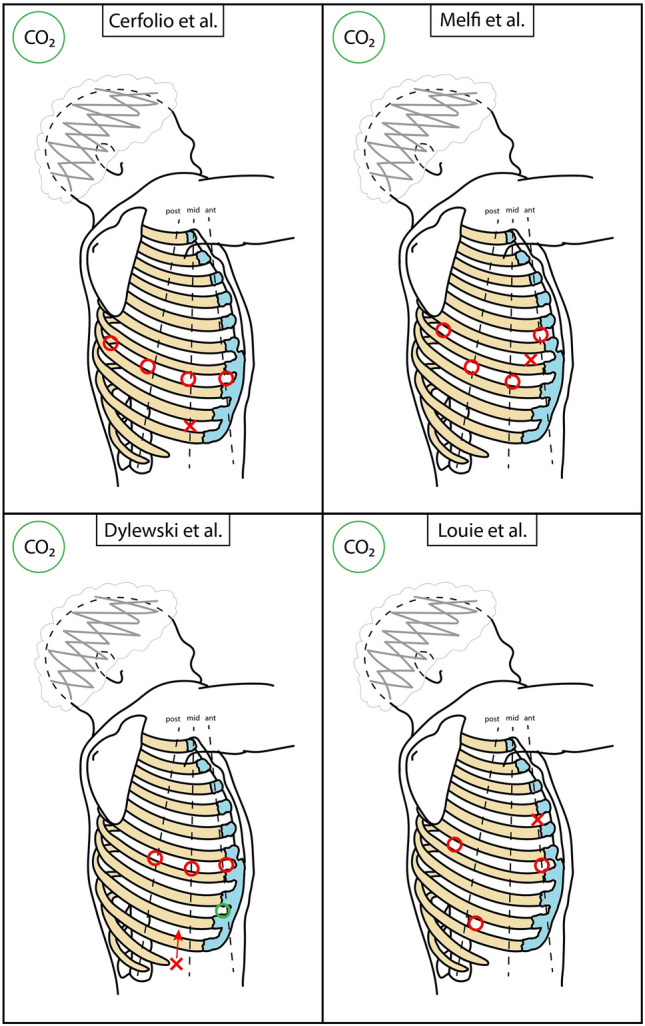
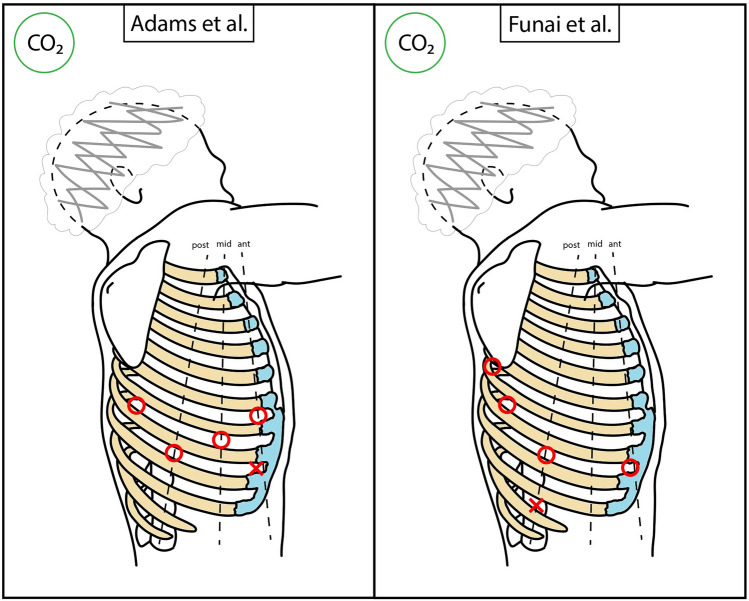
Diagram – RATS main access positioning (schematic with mini-thoracotomy)
Diagram – RATS main access positioning (schematic with tunneling)
Diagram – RATS main access positioning (schematic)
Diagram – VAL-MAP 2.0 workflow (microcoil placement, 3D reconstruction, fluoroscopy-guided resection)
CT/PET – Pulmonary lesion (surgical port mapping)
CT/Bronchoscopy – Tracheal esophageal tumor (stent obstruction, APC recanalization)
CT/Bronchoscopy – Tracheal polypoid metastasis (rigid bronchoscopy coring, APC)
CT/Bronchoscopy – Tracheoesophageal fistula (SEMS placement and removal, stenosis management)
CT/Bronchoscopy Correlation – Tracheal mass with near-complete obstruction
CT/Bronchoscopy Correlation – Tracheoesophageal fistula (esophageal tumor, stent placement with barium swallow)
CT/Bronchoscopy/Chest X-ray – LMB compression (thoracic aortic aneurysm, stent placement timeline)
CT/Bronchoscopy/Chest X-ray – Mediastinal mass (LMB occlusion, stent placement)
Silicon stent follow-up (6-month, removal with persistent stenosis)
Single‑Use Bronchoscope (Airway Burn/Cryotherapy)
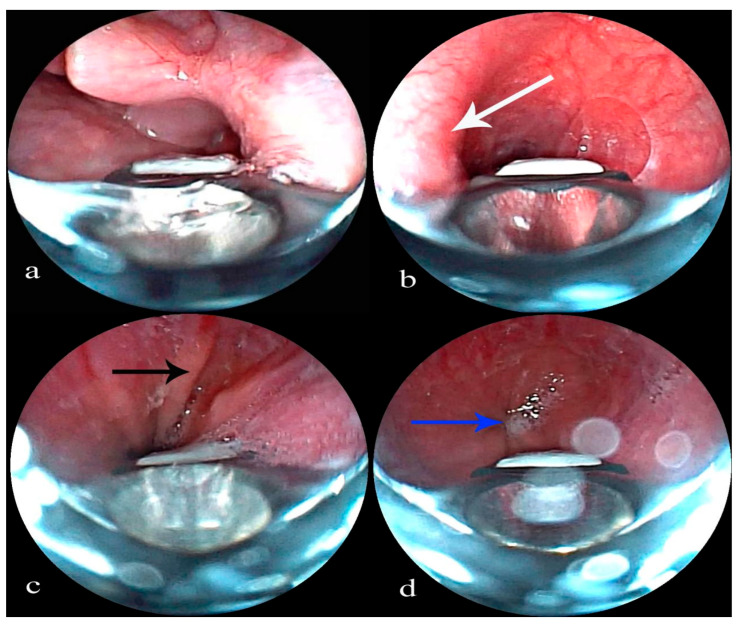
Subglottic stenosis (balloon dilation, Kenalog injection, follow-up)
Subglottic stenosis (IT knife palliation)
Subglottic stenosis (needle knife incisions, Kenalog injection)
Tracheal adenoid cystic carcinoma (pre/post resection, follow-up)
Tracheal and LMB obstruction (stent placement, proximal and distal views)
Tracheal compression (rigid bronchoscopy dilation, Dumon Y stent at carina)
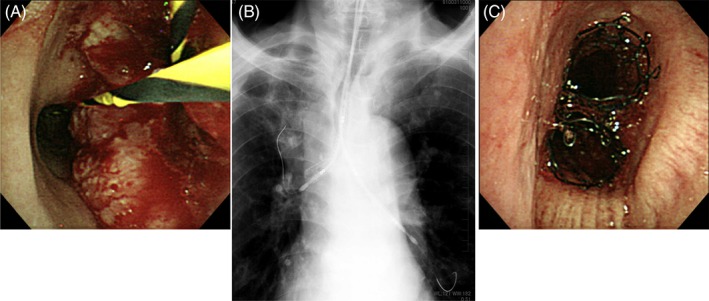
Tracheal invasion and perforation (silicon Y-stent placement for fistula)
Tracheal lobulated mass (pre/post removal, 12-month follow-up)
Tracheal MAO (malignant melanoma, Polyflex stent)
Tracheal papilloma (pre/post endobronchial treatment)
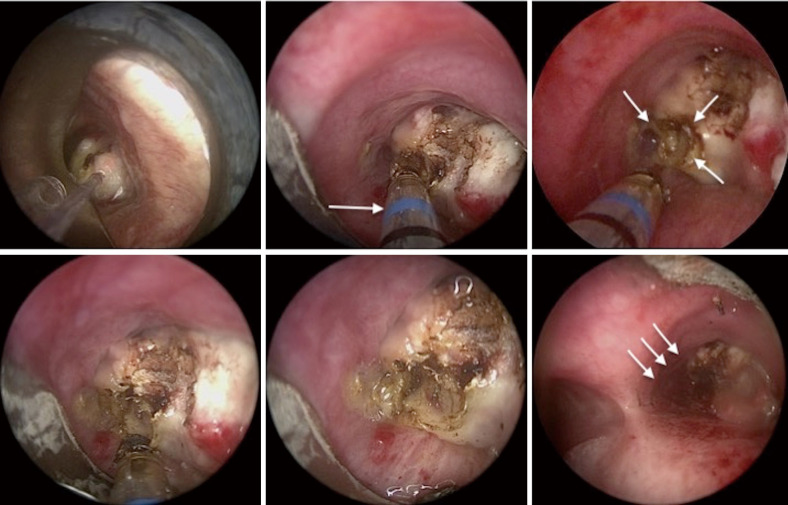
Tracheal polypoid tumor (APC, cryoablation, snare resection sequence)
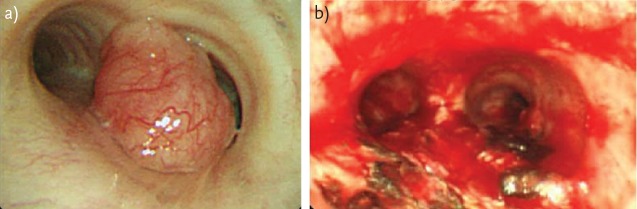
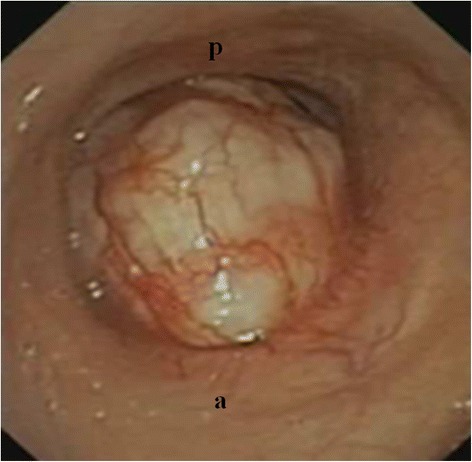
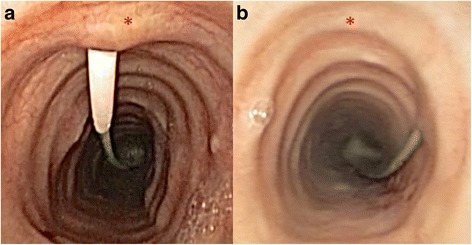
Tracheal Schwannoma (White Pedunculated Lesion)
Tracheal squamous cell carcinoma (diode laser coagulation, scabbard trachea)
Tracheal stenosis (covered Ultraflex for malignant lymphoma)
Tracheoesophageal fistula (covered Ultraflex with migration)
Tracheoesophageal fistula suturing (rigid bronchoscopy technique)
Tumor clearance (mechanical removal via rigid bronchoscope)
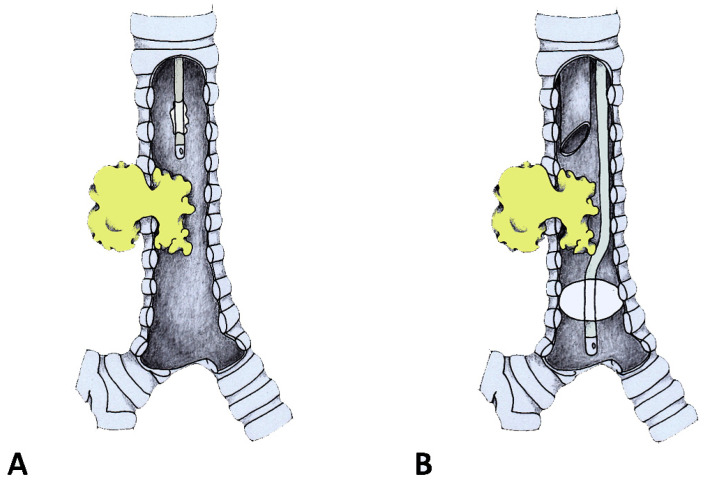
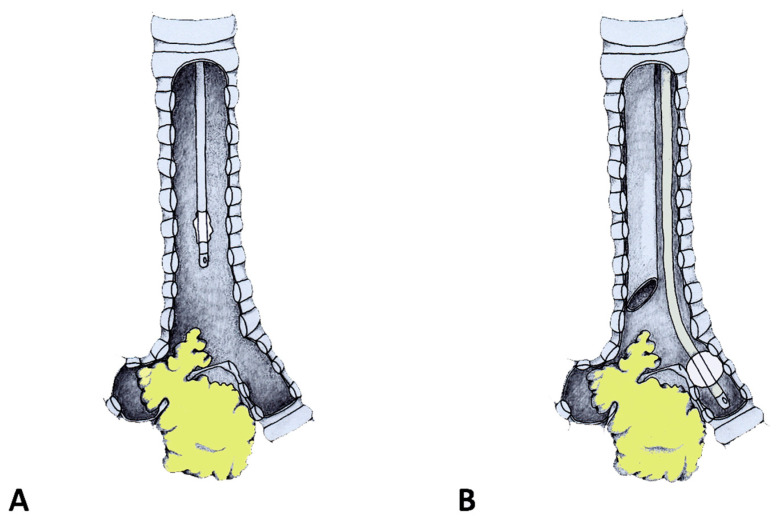
Types of Malignant Airway Obstruction (Examples)
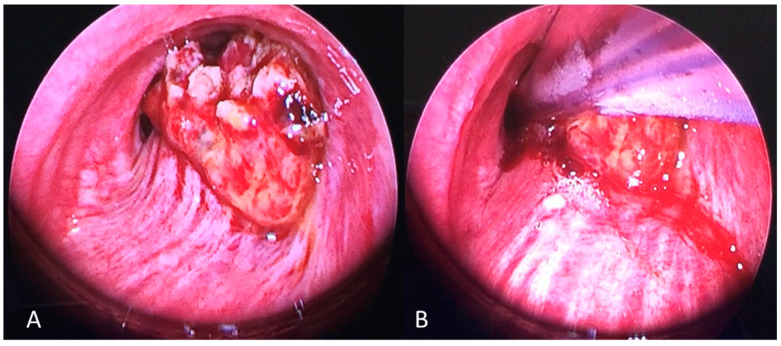
Typical Carcinoid (Pre/Post Laser Resection)
Y-shaped stent removal (failed expansion, hook retrieval)
Bronchoscopic Images/CT – Dumon Oki stent (RMB extrinsic compression, post-stenting)
Bronchoscopic Images/CT – RML fistula stent management (placement, restenosis, removal timeline)
Bronchoscopic Images/CT – Tracheal stenosis (covered Ultraflex for lymphoma, R-CHOP therapy, 6-year survival)
Bronchoscopic Images/CT – Tracheal stenosis (spiral Z stent for thymic cancer, 6-year survival)
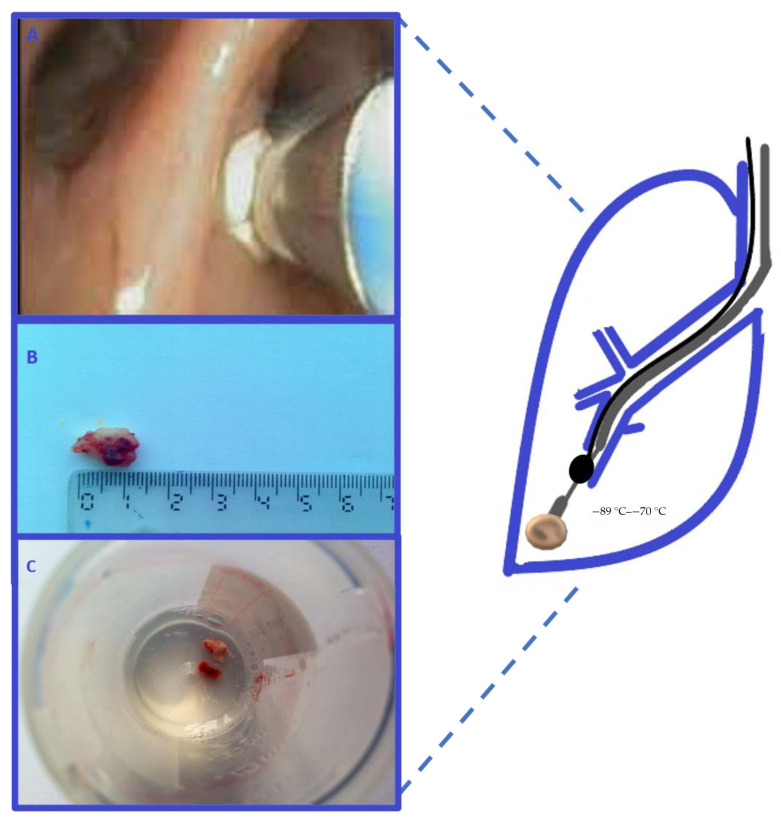
Cryo-debulking (endoluminal tumor)
Cryotherapy (silicone stent-induced granulation)
Dynamic stenosis and stent complications (Y-silicone stent, metallic stent, granulation)
Early Endobronchial Lesion (Silver Hue)
Early squamous cell carcinoma (central airways)
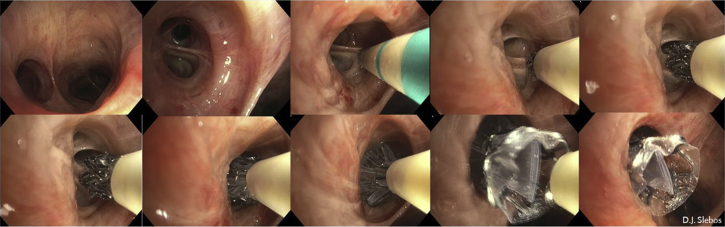
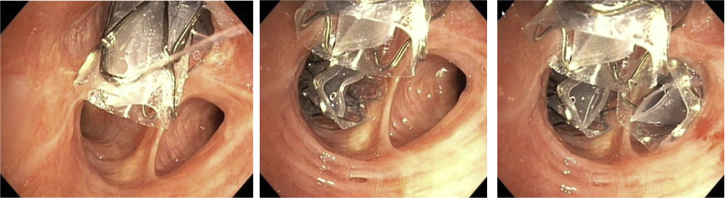
Endobronchial hamartoma (core-out and cryotherapy sequence)
Endobronchial leiomyoma (LMB obstruction, EC snare/cryo debulking)
Endobronchial lipoma (cryorecanalization sequence)
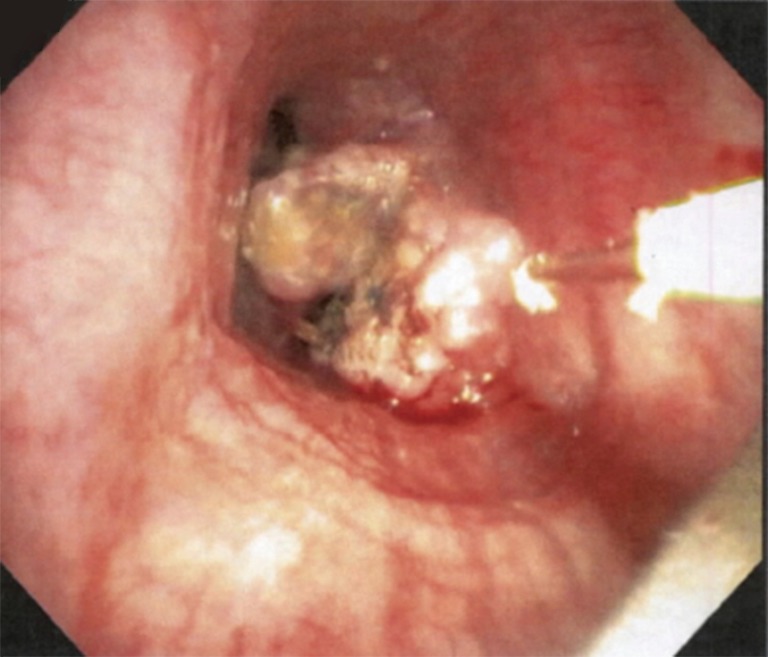
Endobronchial Mass (Tracheal Lesion at Presentation)
Endobronchial mucous adenoma (treatment timeline with histology)
Endobronchial tumor (middle lobe, pre/post resection)
Endoluminal Carcinoid (Resection Correlation)
Extrinsic CAO (silicone Y-stent for airway recanalization)
Fibroepithelial tumor (LUL superior segment, pre/post treatment)
Fibrotic Stenosis (Left Main Bronchus)
Fogarty Balloon (Hemoptysis Control)
Foreign body removal (intermediate bronchus, granulation cautery, basket/forceps techniques)
FOT placement above stenosis (rigid scope insertion with cuff)
FOT placement for carinal obstruction (cuff inflation technique)
iSGS proximal stenosis progression (cross-sectional evolution stages)
LMB occlusion management (microdebrider debulking, APC, stent placement)
LMB stenosis (nitinol stent, 7-year follow-up)
MAO bilateral main bronchi (pre/post therapy, Y-stent)
Mediastinitis with Tracheal Fistula Drainage
Microwave Ablation (LMS Tumor)
Mixed CAO (cryo-debulking and stent placement)
Mixed CAO Resected (Airway Restored)
Modified silicone Y stent removal (post-tuberculous destroyed lung)
Modified Y stent placement (bronchiectasis, occluded LUL branch)
Montgomery T-tube placement (subglottic stenosis, pre/post)
Multimodal CAO management (carinal SCC, laser, Y stent, radiation)
Multimodal MCAO management (bilateral stent placement with spray cryotherapy)
Neoplasia in airway stent (endoscopic resection sequence)
Paratracheal tumor excision (covered stent with balloon dilation)
Polypoid lesion (RMB vascularized tumor)
Postoperative timeline (pre-op to 3.5 years)
Post‑Transplant Airway Complication Types
Recanalization Post‑Procedure (Trachea)
Rigid bronchoscope and suction catheter (carina level)
SEMS for tracheoesophageal fistula (mechanical ventilation, no fluoroscopy)
SEMS removal (embedded stent, laser vaporization, Y-shape SEMS, PTTS)
Silicon stent follow-up (1-month, granulation formation)
Silicon stent follow-up (4-month, increased granulation)
3D printed stent (customized silicone for complex stenosis)
Airway metastasis (LMB, hepatocellular carcinoma, laser/mechanical debulking)
APC and diode laser (endobronchial treatment sequence)
Balloon Dilation (Incisions → Rigid Scope)
Balloon Dilation (Timeline Sep–Oct 2021)
Balloon Dilation and Stent (Timeline Oct–Nov 2021)
BAO complex tracheal stenosis (mechanical dilation, silicone stent)
BAO from pulmonary amyloidoma (carina, 5-month follow-up)
BD stent (3-month follow-up, mucosal hyperplasia)
BD stent (immediate post-implantation)
Biodegradable stent degradation (3-month follow-up)
Bronchial stenosis (post-dilation and silicon stent placement)
Chest X-ray/Bronchoscopy – SEMS removal with silicone stent replacement (tracheal stenosis, Grade III)
Chest X-ray/CT/Bronchoscopy – SEMS removal failure (LMB, embedded stent, Natural stent insertion)
Rigid Bronchoscopy – Laser/Device Positioning
Rigid Bronchoscopy – Mechanical Debulking (Tip of Scope)
Rigid Bronchoscopy – Microdebrider (Rotating Tip)
Rigid Bronchoscopy – Radial Incisions (Blade; 4/8/12 o’clock)
Rigid Bronchoscopy – Subglottic Stenosis (Severe; Pre‑Treatment)
Rigid Bronchoscopy – Ventilation via Side Port
Schematic – Types of Central Airway Obstruction (Freitag/Murgu)
Specimen – Biodegradable stent fibers (coughed fragments)
Stenting – Metallic Y stent for bronchopleural fistula (LLL)
Stenting – Metallic Y stent for bronchopleural fistula (RML deployment sequence)
Stenting – Metallic Y stent for bronchopleural fistula (RML migration and successful reimplantation)
Stenting – Metallic Y stent removal (hook technique with radiography/CT confirmation)
Stenting –Distal Granulation at Endobronchial Stent
Stenting –Dumon Arm with Cut‑Out + Micro‑Tech “Stent‑in‑Stent”
Stenting –GINA Silicone Stent (Design/Anti‑Migration)
Stenting –GINA vs Dumon (Bench Tests: Anti‑Migration/Force/Flex)
Stenting –GINA vs Dumon (Porcine Stenosis Models; 21 Days)
Stenting –Hook‑Sheath Technique (Tracheal Stent Removal)
Stenting –Micro‑Tech Straight FC‑SEMS
Stenting –Neo‑epithelialization (Metal Stents; 4 Patients)
Stenting –Polydioxanone Tracheal Stent (Radiopaque Markers)
Stenting –Post‑Placement Confirmation (Bronchoscopy)
Stenting –SEMS Deploying System (Aero; Merit Endotek)
Stenting –Silicone Stent Deploying System (Polyflex)
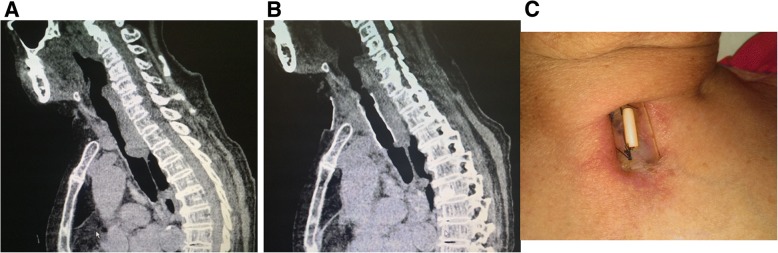
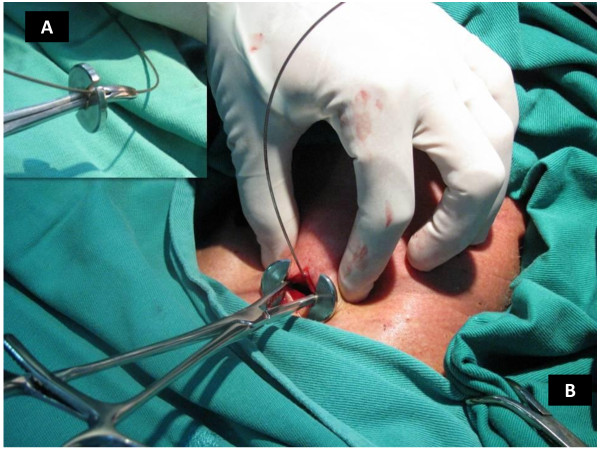
Stenting –Suture Fixation (Case #1; Sagittal CT & Neck View)
Stenting –Suture Fixation (Case #9; Sagittal CT & Neck View)
Stenting –Suture Fixation (Percutaneous Pad; Post‑Op CT)
Stenting –Through‑the‑Scope (TTS) vs Over‑the‑Wire (OTW) Design
Stenting –Y Silicone in Stomach (Migration Case)
Combined Airway/Esophageal Stents (TEF; Fluoro‑Guided)
Esophageal Stent Migration (Relocation Under Fluoro)
MWA Inside Silicone Stent (Ball‑Valve Tumor)
PDT (Early Lung Cancer; Fiber Alongside Lesion)
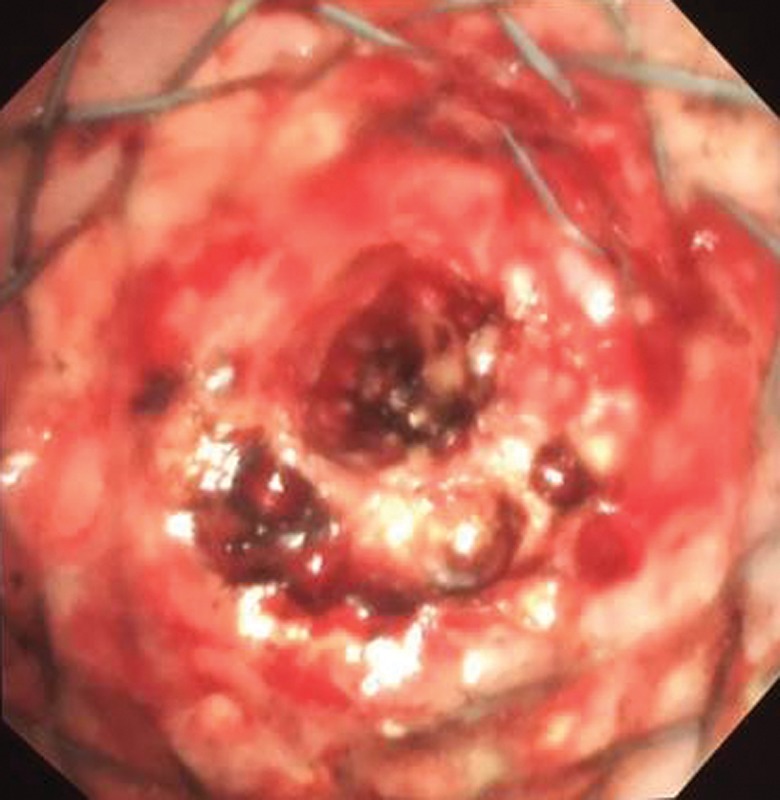
Post‑PDT Debris (Bronchoscopic View)
TEF Coverage with Self‑Expanding Y SEMS (CT/Bronch)
TPO (Carina/Main Bronchi)
TPO (Tracheobronchopathia Osteochondroplastica; Trachea)
Y‑SEMS for Severe Bilateral MAO (Recovery)
Stent – Through‑the‑scope (TTS) outcomes
Bronchoscopic Images – Laser Photocoagulation (YAP/Nd:YAG)
Fluoroscopy – Bilateral SEMS placement (side-by-side method, step-by-step)
Instrumentation – CoreCath 2.7S (Multimodal Debulking)
Direct Laryngoscopy – Subglottic stenosis (0-degree endoscope view)
CT/Spirometry – CAO pre/post stent (flow-volume loops, chemoradiotherapy response)
Airway Stenosis – Montgomery T-tube placement procedure
Algorithm/Procedure – iSGS treatment approaches (endoscopic laryngotracheoplasty techniques)
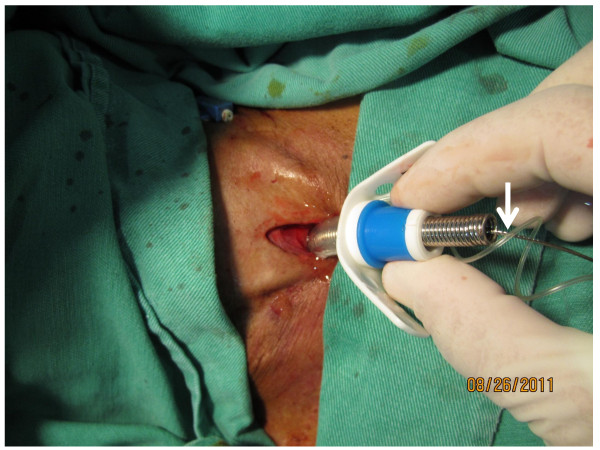
Mini‑Open (Marks and Final Appearance)
Percutaneous Dilatational Technique (Ciaglia)
Single‑Use Flexible Bronchoscope (SUFB)‑Guided PDT
Transillumination Landmarks (PoCUS Correlate)
Ultrasound – Trachea longitudinal view (cricoid and tracheal rings, 8 MHz probe)
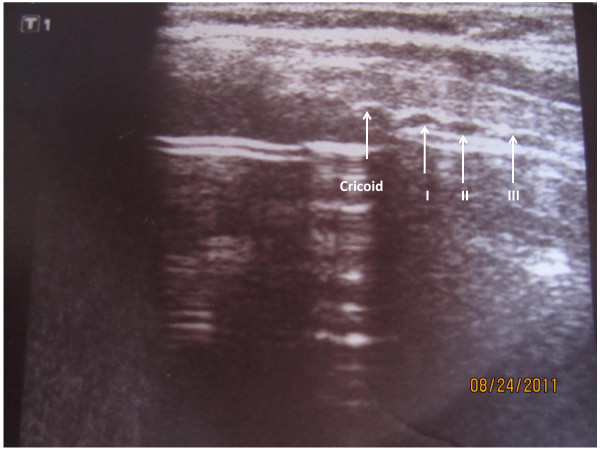
Ultrasound – Trachea sagittal view (cricoid cartilage and five tracheal rings)
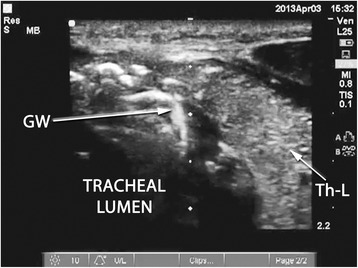
Ultrasound – Trachea sagittal view (guidewire entry point identification)
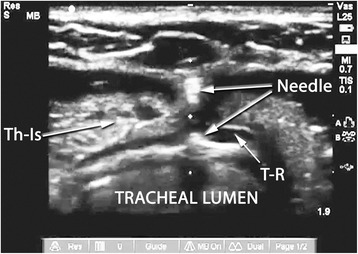
Ultrasound – Tracheal puncture (axial view with needle at anterior wall)
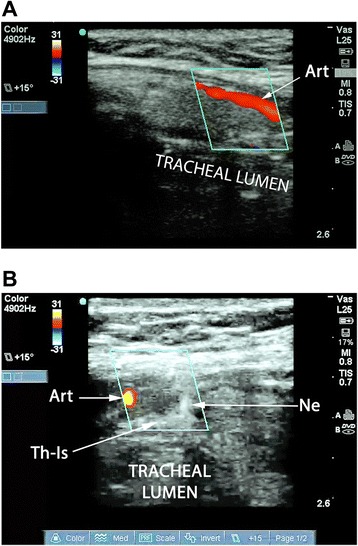
Ultrasound – Tracheal vascular anatomy (duplex imaging, paramedian artery avoidance during puncture)
Ultrasound – Centralized tracheal puncture guidance
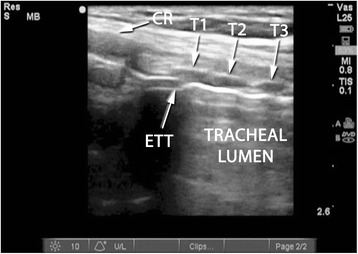
Ultrasound – ETT positioning (tracheal longitudinal view with cricoid and tracheal rings)
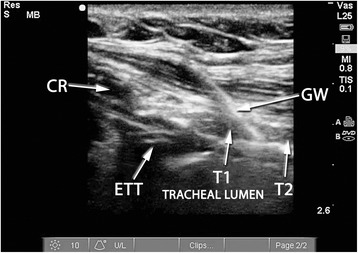
Ultrasound – Guidewire confirmation (axial view, right of midline)
Ultrasound – Guidewire confirmation (longitudinal view, tracheal rings)
Procedure – Tracheostomy anatomical landmarks (fiberoptic guidance, depth marking, puncture angle)
Procedure – Tracheostomy Ciaglia method (dilation and cannula insertion)
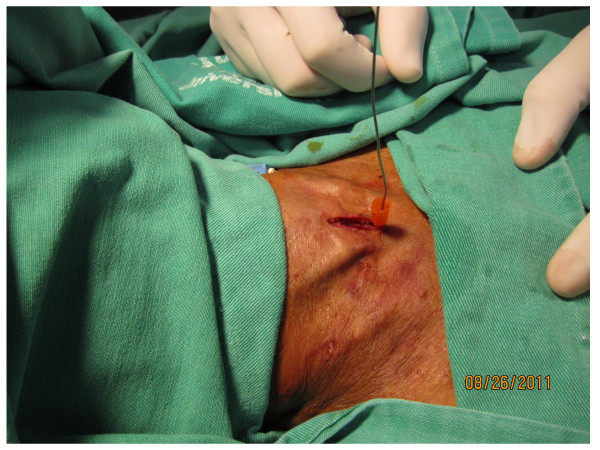
Procedure – Guidewire positioning (14G IV catheter insertion)
Ultrasound/Clinical – Tracheal transillumination with PoCUS guidance (cricothyroid membrane and puncture point)
Diagram – Tracheal ring injuries (classification)
Diagram – Tracheal ring injuries (classification)
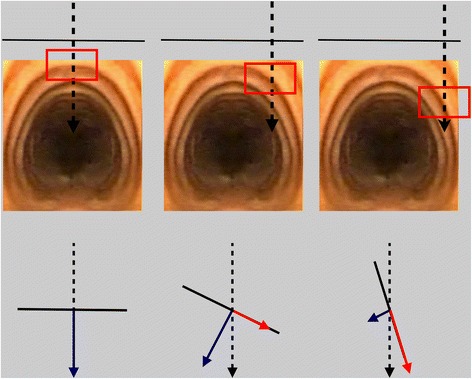
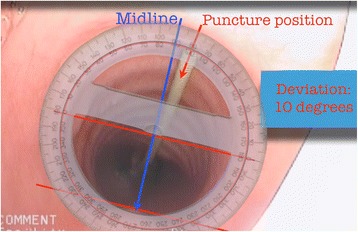
Diagram – Tracheostomy puncture deviation measurement (protractor technique)
Clinical Images – Tracheostomy stomal ulcer (vertical incision, pre/post healing)
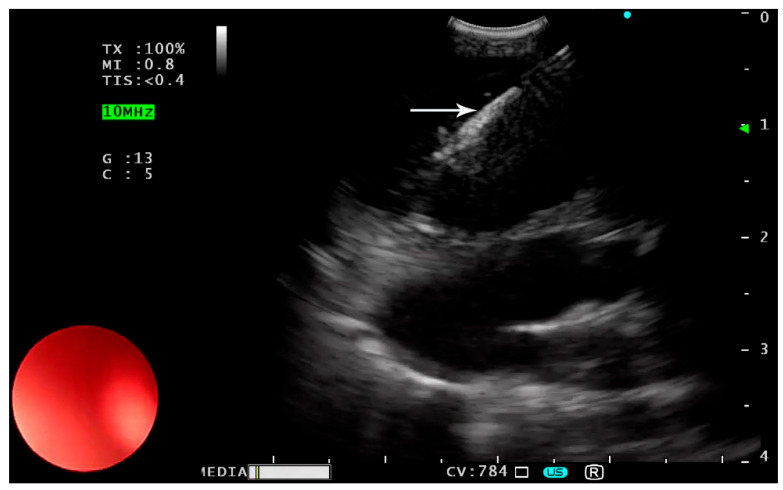
CP‑EBUS (Well‑Circumscribed Water‑Density Lesion)
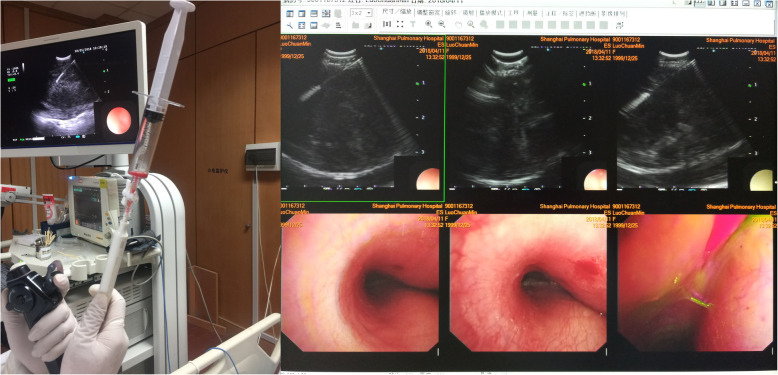
CP-EBUS real-time TBNA (mediastinal lymph node with dual video/US display)
CT/Path Correlation (Right Paratracheal)
CT/Path Correlation (Sarcoid Granuloma)
CT/PET Correlation (Post‑Surgery Recurrence Cases)
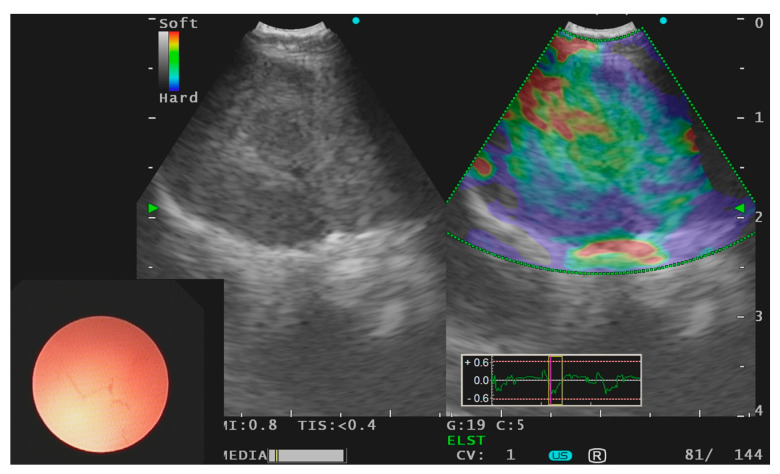
Elastography (subcarinal lymph node with lung adenocarcinoma)
Elastography Types (inflammation vs small cell carcinoma with ROSE correlation)
Lymph Node Aspiration (Cytology/Granulomas)
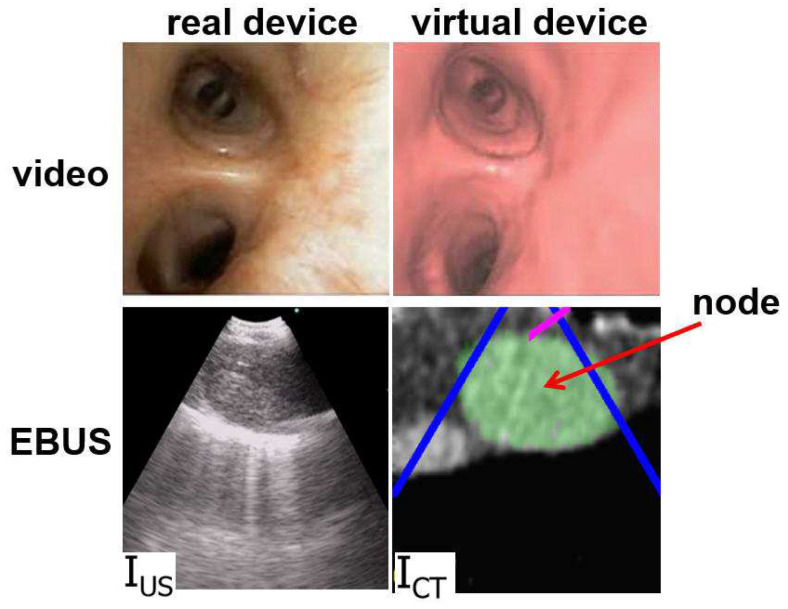
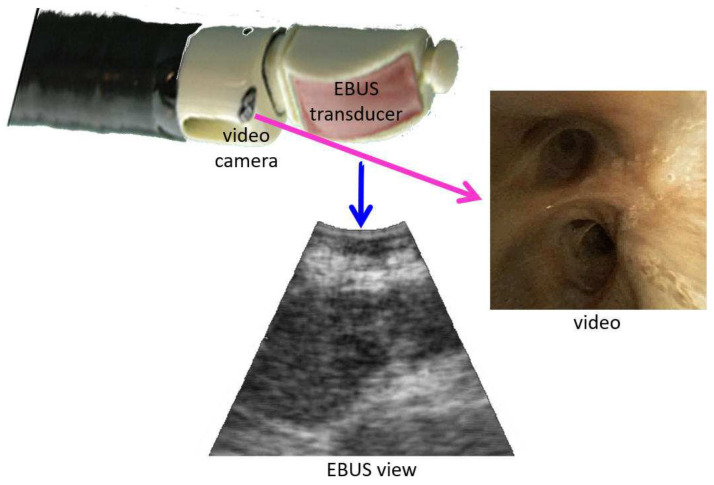
Multimodal bronchoscope views (real vs virtual EBUS/video diagram)
Needle Insertion into Target Mass
Path Correlation (Malignant Mass Adjacent to Aorta)
Simulator (OR Setup & Interface)
Vascular wall–adjacent lesion
Integrated bronchoscope (video camera and 2D transducer, axes diagram)
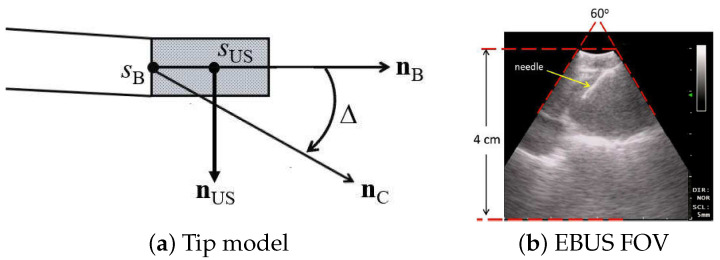
Probe model (device tip and 2D fan-shaped view diagram)
Prototype CP-EBUS with electromagnetic sensor
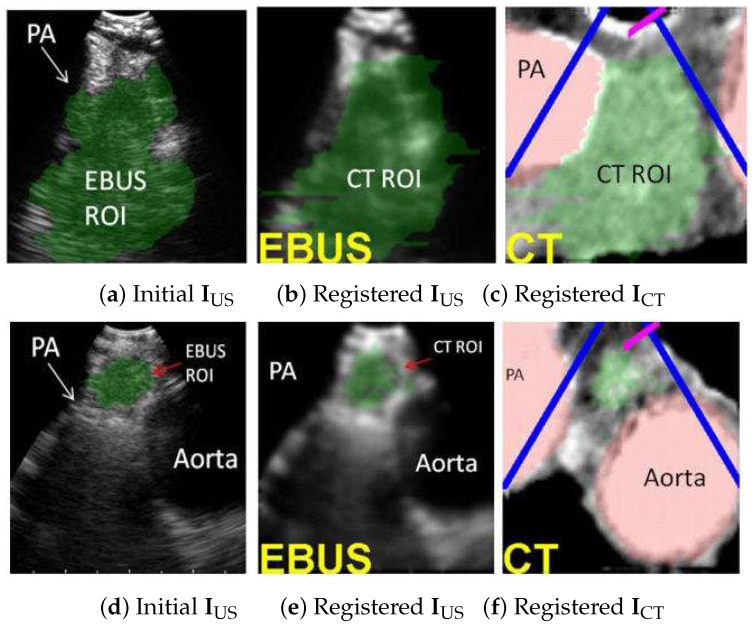
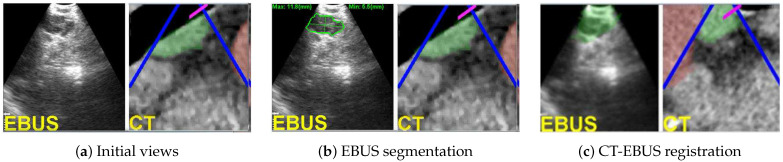
EBUS/CT Registration – Station 4L nodes (segmented ROI, virtual EBUS views)
EBUS/CT Registration – Station-10 lymph node (segmentation and ROI correlation)
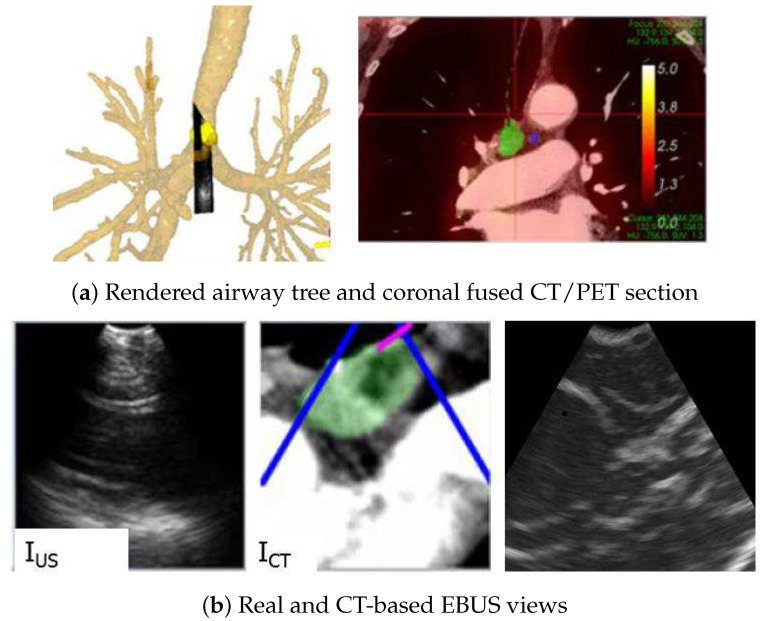
EBUS/CT/PET Correlation – Image-guided navigation (4R lymph node with 3D rendering)
EBUS/CT/PET Correlation – Transvascular EBUS-TBNA (interlobar lymph node and RUL nodule)
EBUS/EUS – Combined station access map
EBUS/EUS‑B – CT/PET/Path Correlation (Adenocarcinoma)
EBUS/PET/CT Correlation – Image-guided navigation (4R lymph node, registered views)
EBUS‑TBNA – Peripheral nodules (left lung)
EBUS‑TBNA – Peripheral nodules (right lung)
EBUS-TBNA – Subcarinal lymph node (sarcoidosis granuloma, color Doppler, ROSE correlation)
Schematic – IASLC Mediastinal Landmarks (mPA/SVC/Esophagus)
Schematic – Mediastinal LN Stations (EUS vs EBUS vs Combined)
Schematic – Stations Map (IASLC ↔ Wang Correlation: 4L)
Schematic – Stations Map (IASLC ↔ Wang Correlation: 4R)
Schematic – Stations Map (IASLC ↔ Wang Correlation: 7)
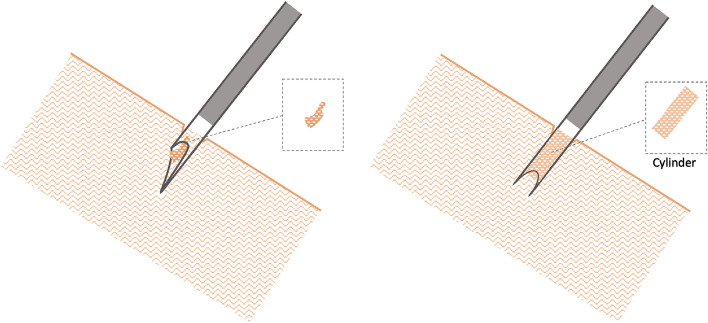
Schematic – TBNA Needle vs Crown‑Cut (Tissue Acquisition)
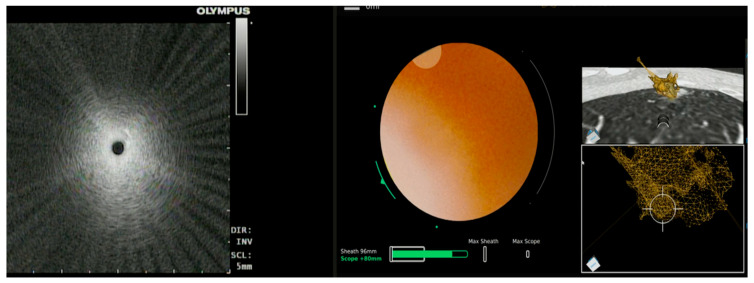
rEBUS – Eccentric lung nodule (detailed procedure)
rEBUS – Views classification (concentric, eccentric, blizzard, no view)
EBUS – Mini‑Forceps (Mediastinal Biopsy)
Diagram – EBUS and EUS (complementary mediastinal lymph node staging)
CT/PET/EUS – Superior mediastinal mass (hypermetabolic, endo-oesophageal puncture)
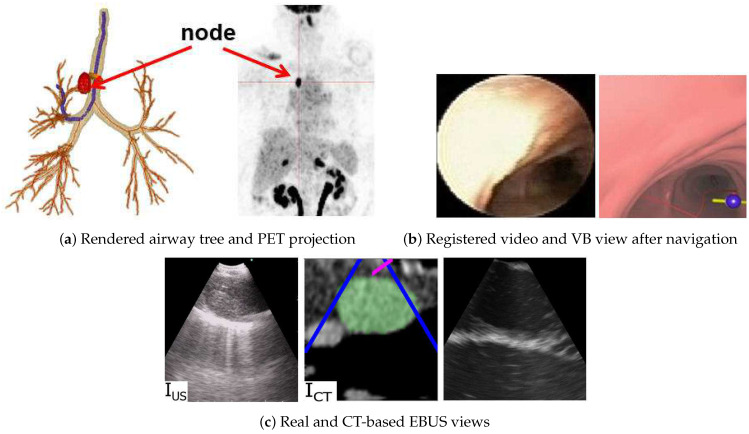
Algorithm – Navigated CP-EBUS workflow (mediastinal lymph node diagnosis, 6-step schematic)
EUS – Aortopulmonary Window (Landmark View)
EUS – Elastography (lung cancer evaluation)
EUS – Left adrenal mass (sliding view, needle placement)
EUS – Lymph Nodes (Benign vs Malignant Patterns)
EUS – Mediastinal Lymph Node (Breast Cancer Metastasis)
EUS – Mediastinal Lymph Node (Sarcoidosis)
EUS – Subcarinal Lymph Node (Diameter 21.4 mm)
EUS – Thoracic Aorta (Mirror Image Artifact)
EUS/CT – Pulmonary embolism (right main pulmonary artery)
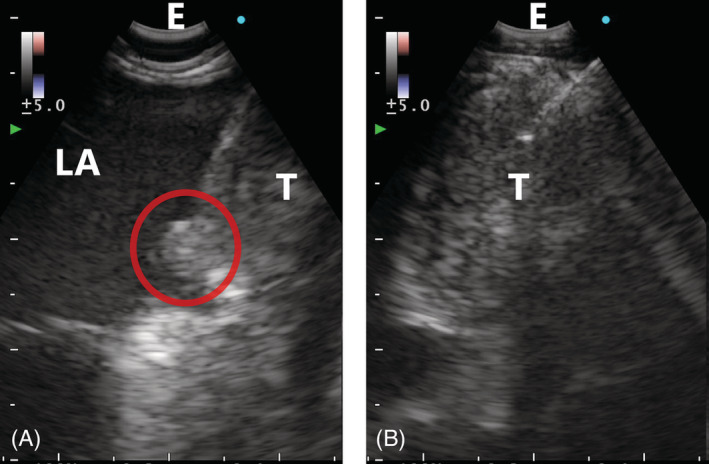
EUS‑B – FNA Findings (Left Atrium Invasion)
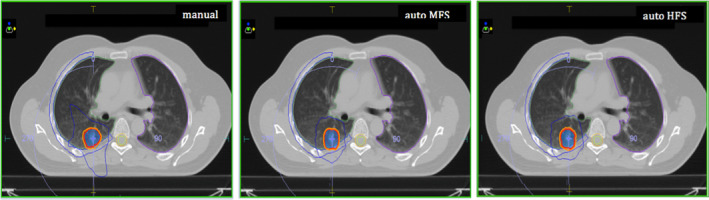
Auto‑planning vs manual (MFS/HFS)
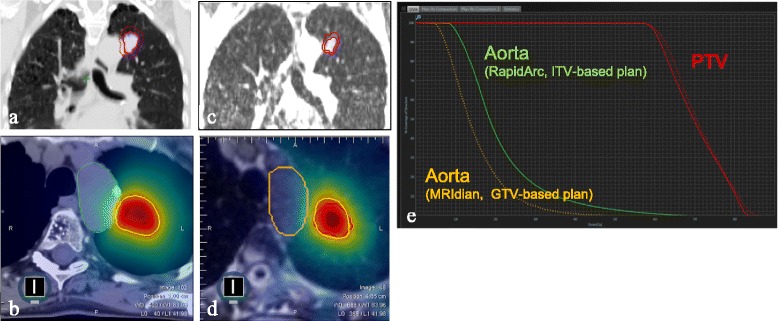
MRI‑guided SBRT vs ITV planning
Radiotherapy – IMRT vs VMAT comparison (66 Gy, dose-volume histogram)
Diagram – Automated radiotherapy planning (RatoGuide and RayStation workflow)
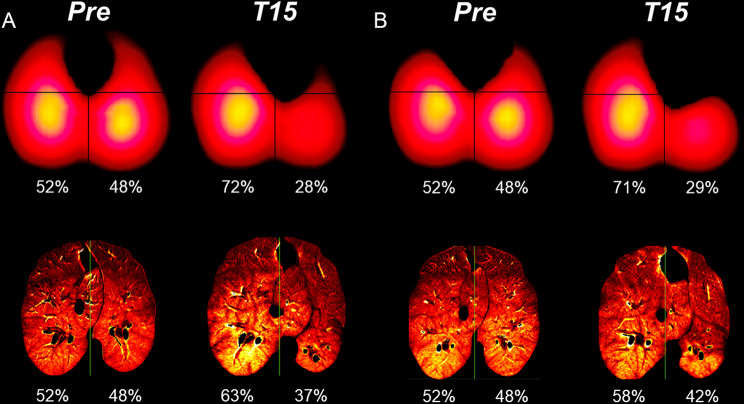
EIT/CT Correlation – BLVR perfusion distributions (balloon vs valves, left hemithorax)
Chartis Assessment (Patient 1; RUL vs LUL; EIT)
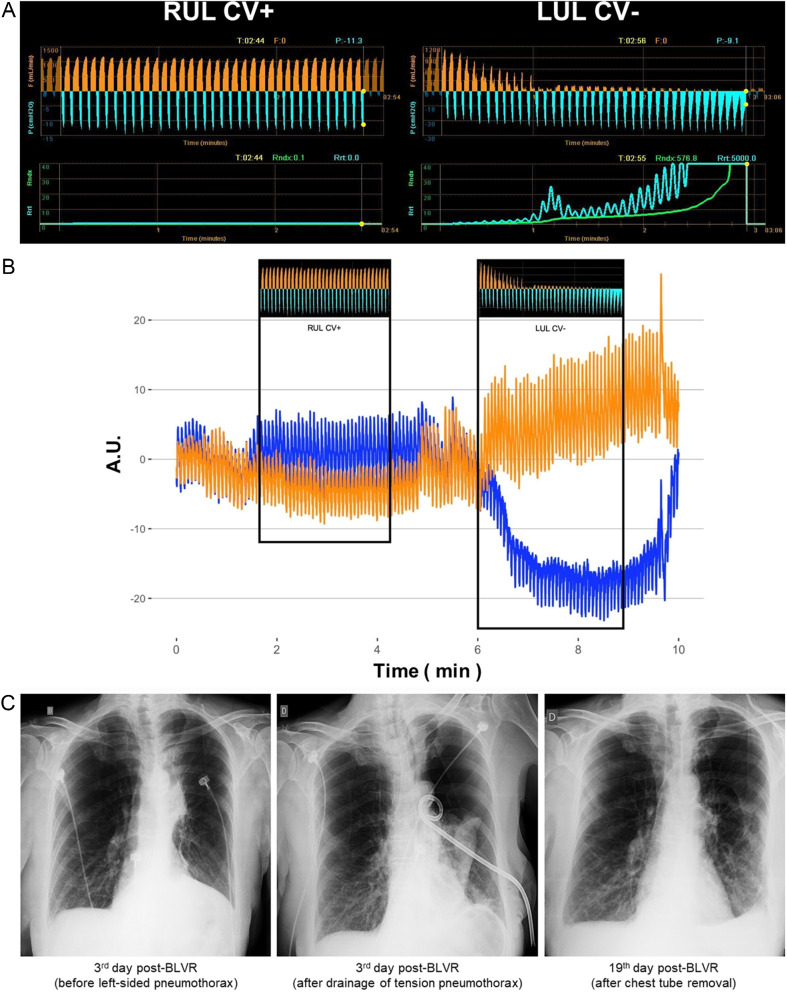
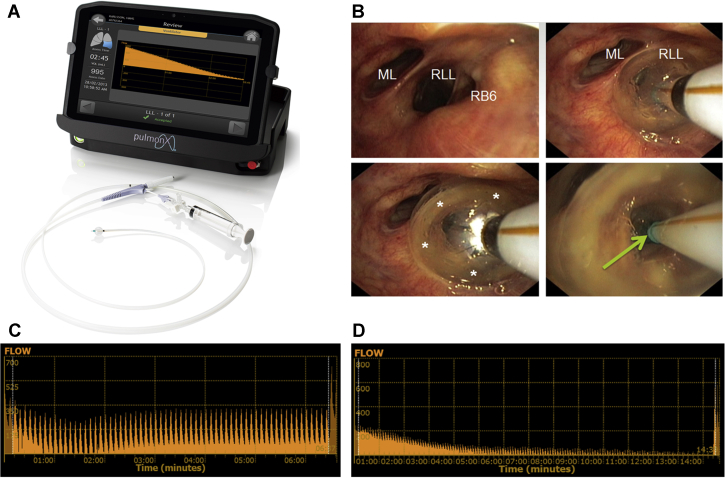
Chartis Pulmonary Assessment (System & Tracings)
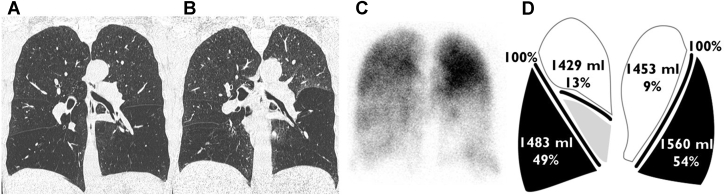
COPD evaluation (CT inspiration/expiration, perfusion, quantitative analysis)
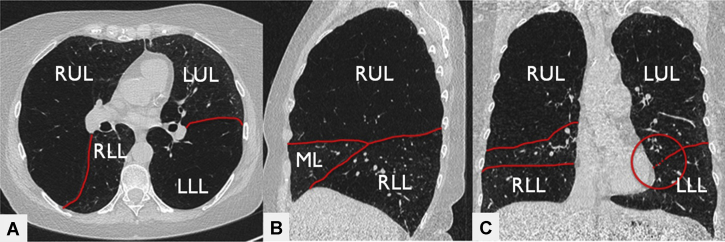
HRCT fissure assessment (visual)
NTM cavities pre/post valve
Post‑Transplant Hyperinflation (Patient 2; EIT+Chartis)
Zephyr valve placement (LB6 deployment sequence)
Zephyr Valves (RUL; RB1/RB3/RB2)
Zephyr vs Spiration (In Situ Comparison)
Nuclear Medicine – Lung perfusion scintigraphy
Amplatzer devices for bronchopleural fistula closure
Anthropomorphic Lungman phantom
Cryo Generator (ERBE; First‑Generation)
Double lumen ETT for Y-stent placement (pusher system with monitoring tube)
Electrosurgery (grounding plate, probe, snare, power unit with pedal)
Galaxy System (C-arm with TiLT tomosynthesis technology)
High-flow nasal oxygen (uses and contraindications)
Laser tube (double cuff, laser guard foil) and rigid bronchoscopy ventilation challenge
LaserJet catheter (dual lumen for gas delivery and pressure monitoring)
Marking coil and ICG loading kit
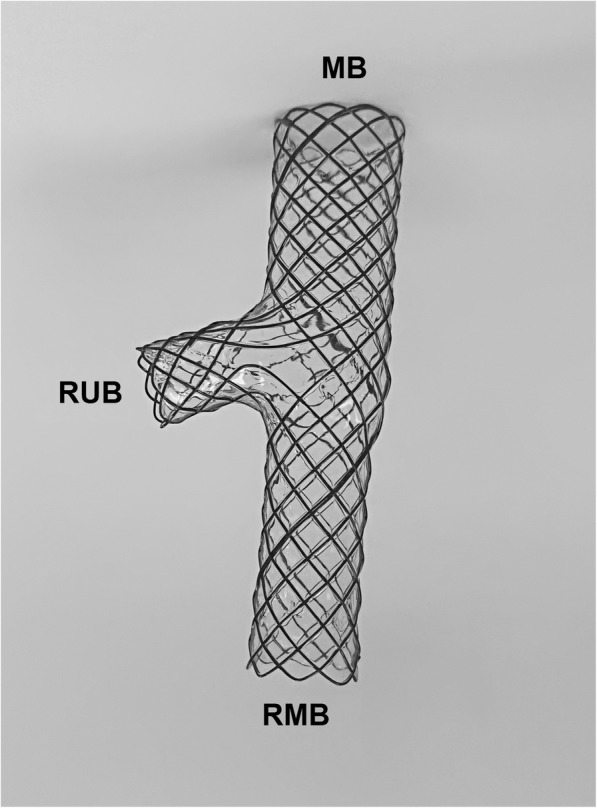
Metallic airway stent (main body, RUB, RMB branches)
Modified blade device (cylindrical handle with blade holder for bronchoscopy)
Modified silicone stent design (main, lateral, and occluded branches with rings)
Olympus Exera III tower (bronchoscopes and processors)
Pleuroscopy instruments (semirigid scope, forceps, Abram's needle, cryoprobe)
Radial ultrasound probes (UM-S20-17S and UM-S20-20R-3)
Radiation shielding setup (lead-equivalent plate and curtain for operators)
Rigid bronchoscope (shaft with fenestration, multifunction head components)
Rigid bronchoscope marking (intubation length measurement)
Rigid bronchoscope tools (Karl Storz system, various lengths and instruments)
Rigid suction catheter setup (three-way stopcock and gas analyzer)
Rigid suction catheter with gas analyzer connection
Robotic CBCT bronchoscope setup (designed bracket)
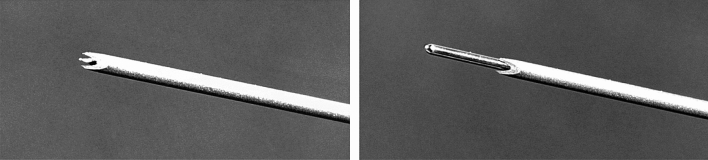
Self-retaining retractor (guidewire positioning with limiter ridge)
Silicon and metal stents comparison
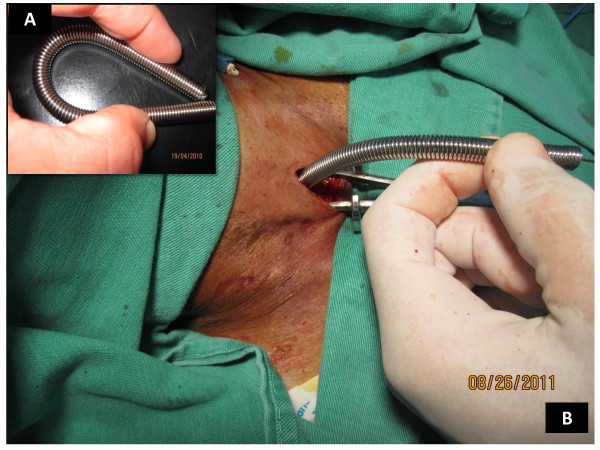
Spherical tip flexible introducer (elastic spring design)
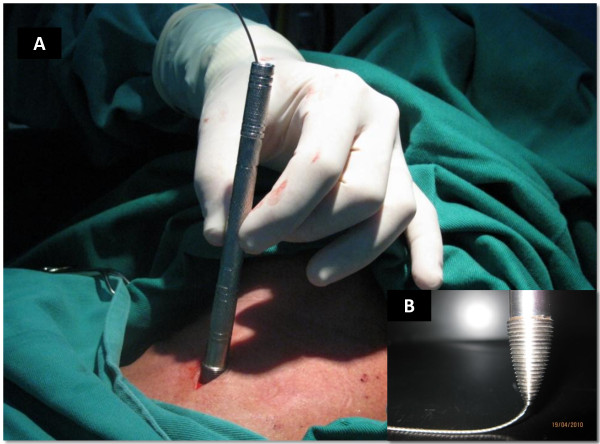
Threaded tip dilator (guidewire technique)
Y-shaped airway stents (large bilateral and single-plugged designs)
Airway stents comparison (Polyflex, Ultraflex, Silmet, Nova-Stent, Dumon, Freitag, Hood)
Instrumentation – Crown‑Cut Tip Needle
Instrumentation – Nodule Marking Kit (ICG/Guidewire/Brush/Coil)
Instrumentation – Olympus Accessories (Forceps, Guide Sheath)
Pleural Cryobiopsy vs Forceps (Tissue Integrity/Size)
Endometriosis (Visceral and Parietal; Lesion Types)
Medical Thoracoscopy – Cryobiopsy (Peripheral Tumor)
Medical Thoracoscopy – Precut Biopsy (Stepwise)
Patient Positioning (Thoracoscopy)
Precut Step‑Up Biopsy Strategy (Schematic)
Thoracoscopic Appearances (Solid/Fibrous/Thickened)
Thoracoscopy + Urokinase Fibrinolysis (Intrapleural Nets)
Trocar Placement (7th Intercostal Space)
Pleura/Vascular Tumor – CT/MR & pathology
Pleuroscopy – Biphasic mesothelioma and pleural metastasis (LTF-Y0032 with 180° curvature)
Pleuroscopy – Empyema (thick loculated with fibrin membrane)
Pleuroscopy – Lesion distribution map (visceral and parietal locations by segments)
Pleuroscopy – Malignant mesothelioma and lymphoma (NBI with vascular patterns)
Pleuroscopy Equipment – Conventional vs new pleuroscope comparison (biopsy forceps positioning)
Pleuroscopy Equipment – Diameter comparison (LTF-240 vs LTF-Y0032)
Pleuroscopy/Bronchoscopy – Pleural adhesions and whitish mass (right bronchus intermedius)
Pleuroscopy/Pathology – Normal parietal pleura pCLE features (chia seed sign, H&E correlation)
Pleuroscopy/Pathology – pCLE features (pleural metastasis with H&E correlation)
CT/Ultrasound/CEUS – Epithelioid mesothelioma (bronchial arterial enhancement, washout)
CT/Ultrasound/CEUS – Epithelioid mesothelioma (circular pleural thickening, systemic arterial enhancement)
CEUS – Subpleural lung tumor biopsy (needle positioning in vital tissue)
Chest X-ray/CT/Pleuroscopy – Precut and cryobiopsy technique (adenocarcinoma with HE staining)
Chest X-ray/CT/Pleuroscopy – Precut technique (biphasic mesothelioma biopsy with CAM/HE staining)
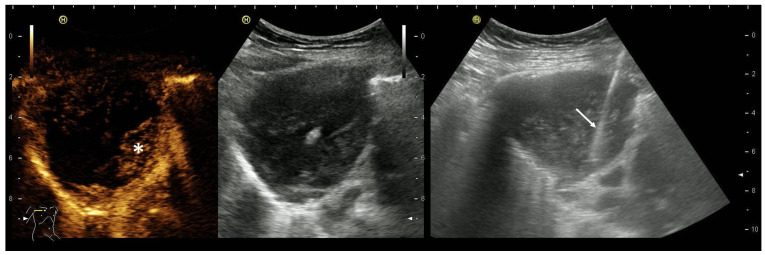
Ultrasound/Pleuroscopy – Pleural effusion patterns (anechoic, complex, septated, homogeneous)
Ultrasound/Pleuroscopy Correlation – Pleural sliding sign, effusion, and adhesions
Ultrasound – Pleural biopsy technique (target identification, vascularization assessment)
CT/Pleuroscopy Correlation – Pleural nodules (lung cancer metastasis vs tuberculous pleurisy)